Research Article
Austin J Public Health Epidemiol. 2014;1(2): 1007.
Who is Assisting Women to Deliver Babies within Health Facilities? An Analysis of Deliveries in Four Provinces in Zambia
Biemba G1,2,3*, Yeboah-Antwi K1,2, Semrau K1,2, Hammond EE1,3 and Hamer DH1,2,3
1Center for Global Health and Development, Boston University, USA
2Department of Global Health, Boston University School of Public Health, USA
3Zambia Centre for Applied Health Research and Development, Zambia
*Corresponding author: Biemba G, Department of Global Health, Zambia Centre for Applied Health Research and Development (ZCAHRD), 121 Kudu road, Kabulonga, P.O. Box 30910, Lusaka, Zambia
Received: July 10, 2014; Accepted: Aug 05, 2014; Published: Aug 08, 2014
Abstract
Skilled birth attendance (SBA) has been shown to reduce maternal mortality and improve birth outcomes. Because skilled professionals are supposed to be present in health facilities, increasing facility deliveries is expected to increase SBA. However, in a country with a critical shortage of skilled health personnel, is this always the case? We present data from three studies conducted in Zambia to understand SBA and delivery practices in health facilities.
In each of the studies, women were asked where and with whom they delivered their youngest child. We calculated the proportion of all deliveries that occurred at health facilities, and proportion of SBAs at health facilities.
Across all three studies, 62.5% of 39,419 were facility deliveries. Of 39,078 deliveries where data were available for the person assisting, SBA was 54.1%; non-SBA was 45.9%. TBAs assisted 18.5% of all deliveries, but of all non-SBAs, TBAs delivered 40.3%.
Among 24,254 health facility deliveries where data were available for person assisting, SBA was 86.3%; non-SBA was 13.7%; TBAs assisted 10% of all facility deliveries. Of all non-SBA deliveries within health facilities, 70.9% were assisted by TBAs.
Our studies revealed that unskilled personnel attended 14% of deliveries occurring within health facilities and TBAs assisted 71% of these. In a country with a critical shortage of skilled health personnel, facility deliveries may not directly translate into SBA. We recommend equipping TBAs with stronger skills to conduct deliveries and manage delivery-associated complications in addition to emphasizing the need to refer to health facilities.
Keywords: Skilled Birth Attendance; Facility delivery; Traditional Birth Attendants; TBA; Zambia
Abbreviations and Selected Definitions
BEmONC: Basic Emergency Obstetrical and Neonatal Care; CHA: Community Health Assistant; CHW: Community Health Worker; CSO: Central Statistics Office; DHS: Demographic and Health Survey; EmOC: Emergency Obstetric Care; LINCHPIN: Lufwanyama Integrated Newborn and Child Health Project in Zambia; MDG: Millennium Development Goal; MOH: Ministry of Health; SBA: Skilled Birth Attendant or Attendance; TBAs: Traditional Birth Attendants; UN: United Nations; UNDP: United Nations Development Program; UNICEF: United Nations International Children's Fund; WHO: World Health Organization; ZDHS: Zambia Demographic and Health Survey; ZamCAT: Zambia Chlorhexidine Application Trial
Traditional Birth Attendant
A person who assists the mother during childbirth and who initially acquired their skills by delivering babies themselves or through an apprenticeship to other TBAs1. Trained traditional birth attendants have received some level of biomedical training in pregnancy and childbirth care. In these studies, we considered both trained and untrained TBAs recognized by the community as such but excluded relatives.
Introduction
Globally, while maternal mortality has declined by 47% since 1990, from 400 maternal deaths per 100,000 live births in 1990 to 210 in 2010, this is still far short of the Millennium Development Goal (MDG) 5 target [1]. According to the UN MDG progress report [1], meeting MDG5 will require accelerated interventions, including improved access to emergency obstetric care and assistance from skilled health personnel at delivery. In Zambia, maternal mortality declined from 649 deaths/100,000 live births in 1996 to 483deaths/100,000 live births in 2010. Despite this reduction, the chance of meeting the MDG5 target for this indicator in 2015 is unlikely. The current level of maternal mortality, with approximately one woman dying every day during pregnancy, labor and delivery, is unacceptably high. Neonatal mortality has declined from 43 deaths per 1,000 live births in 1990 to 27 deaths/1,000 in 2012 [2]. Infant mortality decreased from 107.2 deaths per 1,000 live births in 1992 to 76.2 deaths per 1,000 live births in 2010. However, like maternal mortality, these reductions are not sufficient for Zambia to attain the MDG4 target.
The proportion of deliveries attended by skilled personnel, skilled birth attendance (SBA), rose from 55% in 1990 to 66% in 2011 in developing regions. Despite this increase, about 46 million of the 135 million women who delivered live babies in 2011 did so alone or with inadequate care. In sub-Saharan Africa, a SBA attends only half of all births [1]. In Zambia, SBA has declined from 50.5% in 1992 to 44% in 2010 [2].
There is recognition that countries that have significantly reduced neonatal deaths have focused on having trained midwives at all deliveries, increased pre-natal check-ups and nutritional care, and maternity waiting homes near clinics to reduce travel distances, especially if complications arise [2]. Both health facility delivery and SBA have been associated with reductions in maternal and neonatal mortality [3]. In a recent systematic review, health facility deliveries were found to have resulted in a 29% reduction in the risk of neonatal mortality in low- and middle-income countries [4]. However, this is only so under a conducive environment with skilled staff and EmOC facilities [5]. Both where the delivery takes place and who delivers the baby are important factors in maternal and neonatal survival.
Zambia's strategy to reduce maternal mortality includes ensuring universal access to family planning, skilled attendance at birth, and basic and comprehensive emergency obstetric and neonatal care (EmONC). The MDG progress report for Zambia highlights assisted or supervised deliveries as one of the most critical interventions for ensuring safe motherhood [2]. Supervised deliveries averaged just over60%between 2008 and 2010, which is said to partially explain the reduction in maternal mortality. Supervised deliveries include births assisted by traditional birth attendants (TBAs) and the report states that several typically rural provinces did well due to their high proportion of homebirths assisted by trained TBAs. The report recognizes the role of TBAs in helping to bridge the gap until more midwives are trained.
Zambia's efforts to reduce maternal mortality are hampered by the critical shortage of skilled health personnel. According to the MOH data Zambia has 48% of the midwives and 46% of the nurses it needs [6]. And one of Zambia's strategies is to increase facility deliveries with the aim of increasing the proportion of deliveries attended to by skilled personnel. However, with the critical shortage of skilled human resource, would increasing facility deliveries necessarily increase SBA? To address this question.
This paper presents data on who assisted women to deliver babies and where the deliveries took place. The paper analyses data on who assisted with deliveries outside of the health facilities and within the health facilities. The paper also provides information on non- SBA deliveries within health facilities and who assisted with those deliveries and discusses the challenges these issues pose to improving delivery outcomes and maternal and neonatal health in general.
Materials and Methods
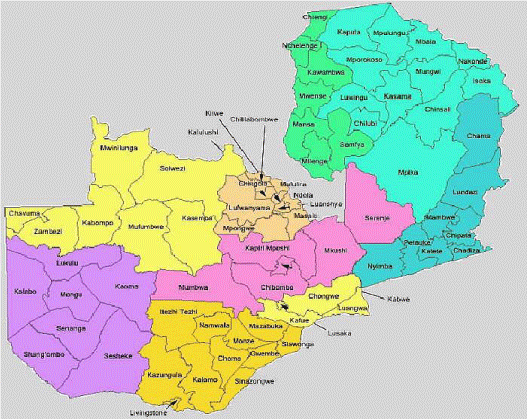
This paper presents and discusses data from three community-level studies in Zambia (Figure 1):
Figure 1 : Map of Zambia with Study Districts.
- Evaluation of the Effect and Cost of Deploying Community Health Assistants to Improve Maternal, New-born, and Child Health in Zambia (The CHA study), conducted 2012-2013.
- Zambia Chlorhexidine Application Trial (ZamCAT), 2011- 2013.
- Lufwanyama Integrated Neonatal and Child Health Project (LINCHPIN), 2011-2013.
The CHA study
This was a baseline cross-sectional household level survey conducted in three communities served by three health posts where a CHA was deployed and three communities served by three health posts where no CHA was available in Senanga District, Western Province, and Luwingu District, Northern Province, of Zambia. The survey was conducted in July 2012 and enrolled women with children under five years of age.Both Senanga and Luwingu districts are predominantly rural.
ZamCAT
This was a cluster, randomized controlled trial that evaluated the impact of 4% chlorhexidine cord washes on neonatal mortality and omphalitis in comparison to dry cord care in Southern Province. This was a longitudinal study conducted from February 2011 until September 2013 and followed pregnant women from the second trimester until 28 days postpartum.
LINCHPIN
This was a baseline cross-sectional household survey of a study that assessed the impact of an integrated, community-based newborn care and community case management delivered through an enhanced district-wide community health program linked to health facilities. The survey was conducted in March-April 2011 in Lufwanyama District, Copperbelt Province and enrolled women with children under five years of age. Lufwanyama is a large, rural, undeveloped district with an estimated population of 75,542 [7]. Despite its location in the mostly urban and industrialized Copperbelt, Lufwanyama district is plagued by deplorable physical infrastructure, poorly maintained roads that are frequently impassible during the rainy season, and a near complete absence of electricity except that produced locally by diesel generators, and no piped water or sewage.
From each of these studies, women were asked where they delivered and who delivered their youngest child. Figure 1 shows a map of Zambia with the districts and study sites for the three studies.
Data management and statistical analysis
Data for both the CHA and ZamCAT studies were collected on Teleforms survey instruments. Data from the TeleForms were scanned and transferred into a Microsoft Access database. After data entry, weekly reports were then generated using SAS v9.1.3 (Cary, NC) in order to conduct basic logic, range, and missing data checks on the database. All data analyses were conducted using SAS 9.1.3.For the LINCHPIN study data entry and cleaning were undertaken using CS Pro through customized data entry screens with in-built range and consistency checks. All forms were entered twice by independent data entry clerks and completed data files compared. Errors were validated and reconciled. Analysis was done using STATA/SAS software. Data from the three individual studies related to the goal of this paper were then entered into an Excel spreadsheet and analyzed to assess: proportion of deliveries conducted at health facility, at home, and at TBA hut; proportion of all deliveries attended by SBA; proportion of all deliveries attended by unskilled birth attendant; and proportion of facility-based deliveries attended by non-skilled birth attendant.
Definitions
For this paper, the following definitions were used:
Facility based delivery: Any delivery occurring in a hospital, health centre or health post, irrespective of the person assisting with the delivery.
Supervised delivery or assisted delivery: Refers to delivery conducted by a doctor, nurse, midwife, clinical officer or traditional birth attendant as inferred from the Zambia MDG report for 2013 [2]. The term "supervised delivery" has however, been used synonymously with SBA [8,9].
Skilled birth attendance (SBA): Any delivery assisted by a doctor, nurse, midwife or clinical officer [10].
Non-SBA delivery: Any delivery not conducted by a skilled person (doctor, nurse, mid-wife, clinical officer), including those assisted by a TBA, relative, or where nobody assisted.
TBA hut: Any delivery assisted by a TBA outside of a health facility.
Results
Sample characteristics
We analyzed data from 2,236 deliveries from the CHA study, 36,449 deliveries from the ZamCAT study and 735 deliveries from the LINCPIN study. The CHA study population consisted primarily of married young women, in the 20-35 year age group. Most of the respondents had educational background up to primary level and were farmers. The ZamCAT study population was younger than the CHA study, mainly in the age group 24 years and below. Like women in the CHA study, most of them had only a primary level of education and 82% were married. The socio-demographic characteristics of the women in the LINCHPIN study were similar to that of the CHA study. Overall, the study population was mostly young, less than 24 years of age, of low educational background up to primary school level, mainly farmers and most of them married (Table 1).
Respondents
CHA
N=2,236
n (%)
ZAMCAT
N=39,375
n (%)
LINCHPIN
N=735
n (%)
All studies
N=42,3446
n (%)
Age
24 years and below
825 (36.9)
20,160 (51.2)
263(35.8%)
21,248(50.2)
25-35 years
981 (43.9)
14,985 (38.1)
346(47.1%)
16,312 (38.5)
36-45 years
383 (17.1)
4,133 (10.5)
118(16.0%)
4,634 (10.9)
46-65 years
29 (1.3)
72 (0.2)
8 (1.1%)
109 (0.3)
> 65 years
18 (0.8)
0 (0)
8 (1.1%)
26 (0.1)
Level of Education
No education
176 (7.9)
3,894 (9.9)
86(11.7)
4,156 (9.8)
Primary
1,695 (75.8)
20,461 (51.9)
456(62.0)
22,612 (53.4)
Secondary
355 (15.9)
14,656 (37.2)
188(25.6)
15,199 (35.9)
Post-secondary
10 (0.5)
340 (0.9)
5(0.7)
355 (0.8)
Marital status
Married
1,774 (79.4)
32,606 (82.8)
623 (84.8%)
35,003 (82.7)
Separated/divorced
131 (5.9)
311 (0.8)
34 (4.6%)
476 (1.1)
Single/Unmarried
277 (12.4)
6,154 (15.6)
67 (9.1%)
6,498 (0.2)
Widowed
54 (2.4)
100 (0.3)
11 (1.5%)
165 (0.4)
Main occupation (N=2,970)
Business/self-employed
108 (4.8)
-
126(17.1)
234 (7.9)
Farmer
1,852 (82.9)
489(66.5)
2,341 (78.8)
Civil Servant
-
-
14(1.9)
Housewife
204 (9.1)
85(11.6)
289 (9.7)
Unemployed
52 (1.1)
-
-
Other Office work
-
2(0.3)
Other
19 (0.9)
19(2.6)
65 (2.2)
Place of Delivery. Table 1: CHA study socio-demographic characteristics of respondents and household.
Place of delivery
Among the three studies only about two thirds of the women (24,621 out of 39,418) delivered at a health facility; with 36.5% of the deliveries (14,375 out of 39,418) occurring at home. There were fairly large variations among the three studies in terms of facility deliveries, with the LINCHPIN study recording the lowest percentage of facility deliveries at 31.0% (228 out of 735) and the ZamCAT study recording the highest at 63.8%; while the CHA study recorded 51.7% facility deliveries. Less than 1%of the deliveries occurred at a TBA hut overall. However, in the LINCHPIN study 7.2% delivered at a TBA hut. A TBA hut refers to any place where a TBA conducts delivery, including the TBA's house (Table 2).
Indicator or characteristic
CHA (N=2234)
n (%)
ZamCAT (N=36,449)
n (%)
LINCHPIN (N=735)
n (%)
All Studies (N=39,418)
n (%)
Health facility
1156 (51.7)
23,237 (63.8)
228(31.0)
24,621(62.5)
Home
1019 (45.6)
12,906 (35.4)
450(61.2)
14,375(36.5)
TBA hut
50 (2.2)
-
53(7.2)
103(0.2)
Other
9(0.5)
306 (0.8)
4(0.6)
321(0.8)
Place of Delivery. Table 2: Delivery Location.
Person assisting with delivery (all deliveries; N=39,079)
Unskilled deliveries constituted 46% (n=17,923) of all the deliveries across the three studies. TBAs conducted 19% (n=7,218) and 3% (n=1,142) were unassisted. Among the non-skilled deliveries, 40% (7,218 out of 17,923) were delivered by TBAs. The greatest proportion of unskilled deliveries was observed in the LINCHPIN study (73.2%; n=538), followed by the CHA study (69.9%; n=1,563), and ZamCAT study with 43.8% (n=15,823) deliveries assisted by unskilled personnel (Table 3). In the LINCHPIN study, TBAs conducted 96% (n=515) of the deliveries assisted by unskilled personnel. However, in the ZamCAT study Family members conducted half of the unskilled deliveries and TBAs conducted just over one third of the deliveries (Table 3).
Indicator or characteristic
CHA (N=2236)
n (%)
ZamCAT (N=36,108)
n (%)
LINCHPIN (N=735)
n (%)
All Studies (N=39,079)
n (%)
Doctor/clinical officer
75 (3.4)
20(2.7)
95(0.24)
Nurse/Midwife
598 (26.7)
20,285 (56.2)
177(24.1)
21,060(53.9)
Traditional birth attendant
859 (38.4)
5,844(16.2)
515(70)
7,21(18.5)
Community health worker
32(1.4)
-
1(0.1)
32(0.08)
Family member
380 (17.0)
8,295 (23.0%)
19(2.6)
8,314(21.3)
Nobody assisted
95 (4.3)
1,044 (2.9%)
3(0.4)
1,142(2.9)
Other
197 (8.8)
640 (1.8%)
-
1.217(3.1)
Total assisted by skilled birth attendant
673 (30.1)
20,285(56.2)
197(26.8)
21,155( 54.1)
Total assisted by non-skilled birth attendant
1,563 (69.9)
15,823(43.8)
538(73.2)
17,923(45.9)
Proportion of non-skilled deliveries assisted by TBA
859(55.0)
5.844(36.9)
515(95.7)
7,218(40.3)
Proportion of non-skilled deliveries assisted by family member
380(24.3)
8,295(52.4)
19(3.5)
8,314(46.49)
Proportion of non-skilled deliveries unassisted
95(6.1)
1,044(6.6)
3(0.6)
1,142(6.4)
Table 3: Person assisting with delivery (all deliveries).
Person assisting with delivery at health facilities
Table 4 shows data on the person who delivered the woman within the health facility. Out of a total of 24,254 facility deliveries where data was available for this analysis, 86.3% were delivered by skilled birth attendants, mostly a nurse or midwife; and 14% by unskilled personnel. Ten percent (n=2,346) of all the facility deliveries across the three studies were conducted by TBAs and close to 1% (n=166) were delivered by family members.
Indicator or characteristic
CHA (N=1,156)
n (%)
ZamCAT (N=22,870)
n (%)
LINCHPIN (N=228)
n (%)
All Study (N=24,254)
n (%)
Doctor/clinical officer
70 (6.1)
-
20 (8.8)
90(0.37)
Nurse/Midwife
591(51.1)
20,086 (87.8)
176 (77.2)
20,853(86.0)
Traditional birth attendant
285(24.7)
2,029(8.9)
32(14.0)
2,346(10.0)
Community health worker
23 (2.0)
-
0
22(0.1)
Family member
4 (0.4)
162 (0.7%)
-
166(0.7)
Nobody assisted
1(0.1)
32 (0.1%)
0
33(0.1)
Other
182 (15.7)
561 (2.5%)
0
748(3.1)
Total assisted by skilled birth attendant
661 (57.2)
20,086(87.8)
196(86.0)
20,943(86.3)
Total assisted by non-skilled birth attendant
495(42.8)
2,784(12.2)
32(14.0)
3,311(13.7)
Proportion of non-skilled deliveries assisted by TBA
285(57.6)
2,029(72.9)
32(100)
2,346(70.9)
Proportion of non-skilled deliveries assisted by family member
4(0.8)
162(5.8)
0(0)
166(5.0)
Proportion of unassisted deliveries
1(0.2)
32(1.2)
0(0)
33(1.0)
Table 4: Person assisting with delivery at health facilities.
Out of the total of 3,311 unskilled deliveries, TBAs conducted 71%, family members conducted 5%, and 1% was unassisted. 25% (n=285) of the facility deliveries in the CHA study were assisted by TBAs. In the LINCHPIN and ZamCAT studies TBAs delivered 14% (n=32) and 9% (n=2,029) of the facility deliveries respectively.
Discussion
Both the LINCHPIN and CHA study results reveal low to medium [3] levels of health facility deliveries in the respective study areas, ranging from 31% to 52% respectively. This is within the Zambia national average of 48% [11]. It is also within the sub-Saharan region Figures [3]. ZamCAT data reveal high levels of facility deliveries. This is most likely due to the intense community sensitization and messages delivered to pregnant women encouraging them to deliver at health facilities. Health facility delivery has been used as a key maternal health indicator under the premise that it would facilitate and increase the number of births attended to by qualified health professionals and create conditions for safe delivery. Fretheim A. and Hviding K. [12] report that the presence of a skilled birth attendant with the necessary remedies at hand is the main argument for promoting facility-based deliveries. The authors of this paper did not find a formal definition of "facility-based deliveries", but according to them, the term implies having a permanent health facility where skilled attendance for deliveries is being provided. Despite the use of health facility deliveries as a proxy for SBA, there appears to be no clear definition in the literature of health facility delivery. The Zambia DHS for example, includes hospitals, health centres and health posts as facility deliveries irrespective of the staffing pattern at these facilities and irrespective of whether these facilities are designated delivery centers or not [11]. Our data shows that facility deliveries do not necessarily translate into 100% SBA. Part of this is due to the definition of facility deliveries. If we defined facility deliveries in the context of presence of skilled birth attendants, then facility deliveries should translate into 100% as SBAs. The fact that DHS, at least in Zambia, includes health posts as facilities is a problem if we are to promote facility deliveries in order to attain SBAs.
Overall, the proportion of unskilled deliveries of 46% observed in our data is lower than the national figure of 56% [2]. However, an examination of the individual studies reveals fairly high proportions of unskilled deliveries in the LINCHPIN and CHA studies, with 70-73% of the deliveries attended to by unskilled personnel respectively. This is not surprising, however, considering that there has been a general decline in the proportion of deliveries attended to by SBA in Zambia over the period 1992 to 2010 [2]. In the African region SBA is only 46.5%; hence unskilled delivery still stands at 55.5%. Overall, our data on unskilled deliveries is just lower than the Africa region average. Global literature shows that 34% of deliveries take place without SBAs [13]. The question is what should be done to help the large number of women currently delivering without skilled assistance? Is what Zambia calls "assisted delivery" using trained TBAs a workable interim measure? Would equipping the TBAs with greater delivery skills as well as skills to manage postpartum hemorrhage (PPH) be the interim solution? Recent evidence shows that TBAs could be trained to safely and correctly deliver misoprostol to control PPH and to correctly use blood collection delivery mat to measure PPH blood loss [14,15]. The related question is whether using TBAs to manage home deliveries better by equipping them with skills and supplying them with commodities to manage PPH would encourage home deliveries and reduce facility deliveries. We were not able to get any literature that indicates that this may be the case and it may be necessary to conduct rigorous implementation research to evaluate the effect of this approach.
Some of our data on facility deliveries reveal a fairly large number of unskilled deliveries occurring within the health facilities themselves. Data from the CHA study show that, while approximately half of the deliveries occurred at a health facility, a SBA attended less than two thirds of these (57%). This means that unskilled personnel conducted 43% or 495 deliveries within the health facilities. Even for the ZamCAT study where SBA at health facilities was 88%, in absolute terms there were 2,784 unskilled deliveries within health facilities during the study period. A large proportion of these unskilled deliveries in health facilities were conducted by TBAs, both trained and untrained. In the CHA study, 285 of the 495 unskilled deliveries within health facilities were conducted by TBAs. The ZamCAT study data revealed that 2,029 of the 2,784 unskilled deliveries (73%) within health facilities were conducted by TBAs. These data pose a number of challenges to the goal of achieving the millennium development goal number 5. First, in a country like Zambia with a critical shortage of staff for BEmONC, increasing facility deliveries may not necessarily reduce the number of unskilled birth attendance [16]. Secondly, the low proportions of facility deliveries, as shown by two of the three studies in Zambia, and considering that there are large numbers of unskilled deliveries occurring within health facility deliveries, poses great challenges to reducing maternal and neonatal mortality through SBA. Thirdly, the fact that most of the unskilled deliveries occurring in health facilities were attended to by TBAs adds to the debate on the role of TBAs in the delivery of babies and the skills TBAs should be equipped with. According to Prata et al. [17], in 2011 there were 28 countries from four major regions in which SBAs attended fewer than half of all births. And 69% of maternal deaths in those 4 regions could be attributed to the 28 countries, despite the fact that those countries only constituted 34% of the total population in those regions [18]. Prata and colleagues argue that while strengthening health systems makes excellent strategic sense, it does not address the immediate safe-delivery needs of the estimated 45 million women who are likely to deliver at home, without a skilled birth attendant. 46% of the women in the CHA study, 35% in the ZamCAT study, and 61% of the women in the LINCHPIN study respectively delivered at home. This constitutes 14,374 women who delivered at home during the study period of these three studies [19]. The question is who delivered these babies and more importantly, what was the outcome of these deliveries? An even more important question is, while efforts are being made to improve health systems and attain universal access to BEmONC, what should be done to assist these women who currently deliver at home? Prata and others recommend training of community-based birth attendants in primary and secondary prevention technologies (e.g. misoprostol, family planning, measurement of blood loss, and postpartum care) [20]. As stated above, equipping TBAs with more skills and resources may be an answer.
Lastly, we note that 3-4% of all deliveries were unassisted. For the CHA study, this translates to only 95 deliveries. However, for a large sample such as the one for ZamCAT, 3% of the deliveries translate into 1,000 unassisted deliveries. This scenario is not uncommon in sub-Saharan Africa, and thus requires urgent attention. For example, Fapohunda BM et al. [21] notes that not only are Nigerian women predominantly using unskilled attendants, but one in five births are delivered with No One Present (NOP).
Limitations
Although the studies on which this paper is based are fairly large and had representative samples to detect change in their original outcome measures, the sub-analysis presented here may not be representative of the Zambian population as a whole. Another limitation is the unequal sample sizes among the studies included in this paper. For example, ZamCAT with its large sample size may have skewed the results.
Conclusions and Recommendations
Results from the studies in this paper show that there is a fairly large proportion unskilled deliveries occurring within health facilities and TBAs are delivering babies both outside and within health facilities. Hence facility deliveries within the current definition in Zambia and elsewhere in Africa and globally may not translate into SBA and are therefore unlikely to lead to the desired maternal outcomes expected from skilled assistance at birth. We recommend a redefinition of facility delivery as "the proportion of births occurring in a health facility with skilled birth attendants." We also recommend a review of the role of TBAs and their training curriculum to ensure that the TBAs have stronger skills to conduct deliveries and control obstetric complications such as postpartum hemorrhage with misoprostol in addition to emphasizing the need to refer to health facilities. We make this recommendation in the light of the data that shows that in a country like Zambia, with a critical shortage of skilled health personnel for BEmONC, there are a large number of women assisted by TBAs, not just outside of health facilities but even within health facilities.
Acknowledgment
We wish to acknowledge and thank the various funding agencies that provided the resources to conduct the three studies part of whose data is presented in this paper. We thank the Clinton Health Access Initiative (CHAI) through the UK Department for International Development (DFID) for providing funds for the CHA study; the Bill and Melinda Gates Foundation for financing the ZamCAT study; and USAID for providing finances to carry out the LINCHPIN study. We also wish to thank the Ministry of Health for approving the implementation of the three studies.
References
- The United Nations (2013). The millennium development goals report 2013.
- The United Nations Development Programme (UNDP). The millennium development goals progress report, Zambia. 2013.
- Moyer CA, Dako-Gyeke P, Adanu RM. Facility-based delivery and maternal and early neonatal mortality in sub-Saharan Africa: a regional review of the literature. Afr J Reprod Health. 2013; 17: 30-43.
- Tura G, Fantahun M, Worku A. The effect of health facility delivery on neonatal mortality: systematic review and meta-analysis. BMC Pregnancy Childbirth. 2013; 13: 18.
- Goli S, Jaleel AC. What is the cause of the decline in maternal mortality in India? Evidence from time series and cross-sectional analyses. J Biosoc Sci. 2014; 46: 351-365.
- Anyait A, Mukanga D, Oundo GB, Nuwaha F. Predictors for health facility delivery in Busia district of Uganda: a cross sectional study. BMC Pregnancy Childbirth. 2012; 12: 132.
- World Health Organization. Making pregnancy safer: the critical role of the skilled attendant. A joint statement by WHO, ICM and FIGO. 2004.
- Patience M. Etsey. Towards the Millenium Development Goal 5: Assessing the quality of supervised delivery in The GA west district, Ghana. Kwame Nkrumah University of Science and Technology, Kumasi. 2008.
- Sarah M Wablembo, Henry V Doctor. The influence of age cohort differentials on antenatal care attendance and supervised deliveries in Uganda. Journal of Nursing Education and Practice. 2013; 3: 11.
- Canavan A. Review of global literature on maternal health interventions and outcomes related to skilled birth attendance. KIT Working Papers Series H3. Amsterdam: KIT. 2009.
- MOH/CSO. Personal communication.
- Fretheim A, Hviding K. The evidence-base for facility-based deliveries in low- and middle income countries. Working paper. Oslo: Nasjonalt kunnskapssenter for helsetjenesten. 2008.
- MOH/CSO. ZDHS, 2007.
- WHO. Maternal mortality. Fact sheet No.348. Key facts. 2010.
- Mobeen N, Durocher J, Zuberi N, Jahan N, Blum J, Wasim S, et al. Administration of misoprostol by trained traditional birth attendants to prevent postpartum haemorrhage in homebirths in Pakistan: a randomised placebo-controlled trial. BJOG. 2011; 118: 353-361.
- Prata N, Passano P, Rowen T, Bell S, Walsh J, Potts M. Where there are (few) skilled birth attendants. J Health Popul Nutr. 2011; 29: 81-91.
- Prata N, Quaiyum MA, Passano P, Bell S, Bohl DD, Hossain S, et al. Training traditional birth attendants to use misoprostol and an absorbent delivery mat in home births. Soc Sci Med. 2012; 75: 2021-2027.
- Kreyberg I, Helsingen LM. Skilled attendance at delivery; how skilled are institutional birth attendants? An explorative study on birth attendants at Bansang Hospital, The Gambia. Institute of Public Health, Faculty of Medicine. 2010.
- Bailey P, Paxton A, Lobis S, Fry D. Measuring progress towards the MDG for maternal health: including a measure of the health system's capacity to treat obstetric complications. Int J Gynaecol Obstet. 2006; 93: 292-299.
- Graham WJ, Bell JS, Bullough CHW. Can Skilled Attendance at Delivery Reduce Maternal Mortality in Developing Countries. In: de Brouwere V, Lerberghe WV, editors. Safe Motherhood Strategies: A Review of the Evidence. Antwerpe: ITGPress. 2001: 97-129.
- Fapohunda BM, Orobaton NG. When women deliver with no one present in Nigeria: who, what, where and so what? PLoS One. 2013; 8: e69569.