Case Report
Austin Surg Case Rep. 2016; 1(1): 1001.
Acute Colonic Pseudo-Obstruction (Ogilvie’s Syndrome) as a Post-operative (Caesarean Section) Complication: A Rare Case Report
Urkan M¹*, Alakus U¹, Meral U² and Yagci G¹
¹Departments of Surgery, Gulhane Military Medical Academy, Turkey
²Departments of Surgery, University of IZMIR Medical Center, Turkey
*Corresponding author: Murat Urkan, Department of Surgery, Gulhane Military Medical Academy, 06018 Etlik, Ankara, Turkey
Received: October 12, 2015; Accepted: November 24, 2015; Published: January 20, 2016
Abstract
Introduction: Colonic Pseudo-Obstruction (CPO/OS) characterized by dilatation of the colon with the absence of any mechanic obstruction. This rarely complication occurs after medical/surgical conditions such as sepsis, trauma, Caesarean Section (CS).
Case: A 35-year-old, female was admitted for elective CS. She informed her gynecologist with the abdominal distension and no flatus. After treated with Disodium phosphate, she was examined with severely abdominal tenderness like the clinical evidence of peritonitis. Emergency laparotomy was performed, and caecal perforation with evidence of caecal ischemia was found. There weren’t find obstructive resons. A right hemicolectomy was performed with ileostomy and mucus fistulotomy.
Discussion: CPO/OS is reported as case series rarely. The pathogenesis of OS is still vaguely. Some concepts related pathogenesis of OS with the imbalance of colonic innervation. It can be misdiagnosed like a paralytic ileus. Early diagnosis and treatments are important steps in preventing ischemia and perforation.
Conclusion: To pay attention about careful management of early postoperative dilatation with increasing ratio of CS.
Keywords: Acute Colonic pseudo-obstruction; Ogilvie’ syndrome; Caesarean section; Peritonitis
Introduction
Colonic pseudo-obstruction refers to massive colonic distension with functional disorder of the colon (Ogilvie’s syndrome, OS) [1]. This rarely complication occurs after medical/surgical conditions such as electrolyte imbalance, sepsis, spinal trauma/surgery, malignancy, burns and Caesarean Section (CS) [2]. This situation may be misdiagnosed easily, as a dynamic ileus especially after CS. The pathophysiology of the OS is still unclear and characterized by a dramatic dilatation of the colon with the absence of any mechanic obstruction.
Commonly, right colon and caecum affected. Furthermore, if it is misdiagnosed, it can result in significant morbidity and mortality (31% and up to 45%) after spontaneous perforation [3]. We aim to show, right colon perforation, requiring right hemicolectomy, which occurred in early puerperium following CS.
Case Presentation
A healthy 35-year-old pregnant was directed to the elective CS with epidural anesthesia for previously cesareans. There were no operative complications except minimal blood loss. The total operating time was being up to standard. And a healthy baby girl weighing 3.3kg was delivered.
Firstly, the patient getting well at early postoperative day, and needed usual analgesia just as diclofenac (50mg 3× daily), paracetamol (1g 4 × daily). On the second Postoperative Day (POD), she had abdominal distension and no flatus. Although she had not any abdominal pain firstly. Therefore she was treated with Disodium phosphate. After than; she developed abdominal pain which is into colicky at POD 2. Although, she had passed flatus and had no vomiting. After two days with observation and treatment, she was consulted to our general surgery clinic. Firstly, we examined her and she has hard abdominal distension with severely abdominal tenderness like the clinical evidence of peritonitis.
A plain abdominal film and abdominal ultrasound was done. Massive gaseous distention of the bowels with fluid levels and no free air were described (Figure 1). Although she was threatened with conservative ways with which nasogastric tube and rectal tube insertion, patient’s condition did not have any symptomatic benefit. Moreover, with the clinical evidence of peritonitis, her condition deteriorated. Then, showed widespread colonic dilatation and a maximum caecal diameter of 10cm with CT imaging (Figure 1).
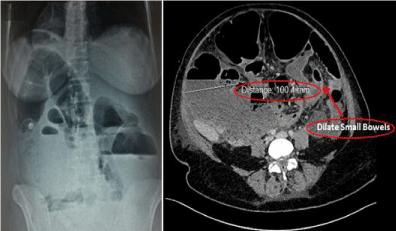
Figure 1: Plain abdominal radiograph and CT scan with Large Colon
Segments (100.4 mm).
Emergency laparotomy was performed and distended colon with caecal ischemia and perforation was found. However, we didn’t find any evidence of mechanical obstruction. A right hemicolectomy with dense irrigation and drainage was performed but couldn’t perform an anastomosis due to severely peritonitis (Figure 2). After that, terminal ileostomy with mucus fistulotomy was performed. Postoperative recovery was unremarkable, but we identified evisceration at POD 5. Then we threatened our patient with Vacuum Assisted Closure (VAC) (Figure 2). Then we sutured abdominal wall after second VAC procedure. But we go on VAC for skin defect, and sutured it on fourth day. The patient recovered and discharged 15th day.
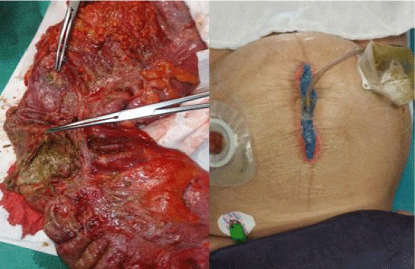
Figure 2: Right hemicolectomy material with 4-5 cm ischemic/perforation
area and abdominal wall closure using the Vacum Asisted Closure (VAC) for
evisseration and skin defect.
Discussion
OS is reported just case series scarcely. Some cases have been reported following pregnancies which are full of trouble (preterm labour, pre-eclampsia…etc). However, abdominal, orthopedic, and vascular surgery could associated with OS, CS is the most common surgery that is associated with OS [2].
The pathogenesis of OS is still vaguely. Some concepts related pathogenesis of OS with the imbalance of colonic innervation. Surgery and/or trauma accelerate the risk of injury. Robert et al., suggested that; pathogenesis of OS is most probably multifactorial and which group of women are predisposed to developing this complication is unclear [4].
Patients (OS) frequently present with regular symptoms such as massive abdominal distension and mild abdominal pain. It is associated with the presence of hyperactive or normoactive bowel sounds. There may be pan colonic dilatation or segmental colonic dilatation especially cecum and right colon. Cecal diameter (9-12 cm) ought to be considered as a critical point [5] and it can be misdiagnosed like a paralytic ileus easily. Non-surgical and surgical treatment can be applicable for OS. High rate mortality has been reported in cases without perforation (12-30%) and cases with perforation (40-50%) when there is a wrong diagnosis [6]. Initially, mostly cases diagnosis like paralytic ileus. Conservative management may be practicable until cecal diameter reaches 9 cm, but surgical management should be indicated when reaches more [7]. So early diagnosis and treatments are important steps in preventing ischaemia and perforation.
Conclusion
In this case, conservative management with which corrections of the fluid, electrolyte balance and nasogastric suction were not adequate initially. In addition, high level irrigation of colon may be accelerating the ischemia and perforation. Maybe, colonoscopic decompression could have been employed as part of the management. In literature, most cases can be diagnosed with colonoscopic decompression successfully [2,8]. Surgical procedure may have been avoided if pseudo-obstruction is diagnosed early and treated with effective decompression. But in lately cases surgery is the ideal procedure for patients’ mortality risk.
We should be more careful for the management of early postoperative dilatation among the increasingly ratio of cesarean sections and OS.
References
- Ogilvie H. Large-intestine colic due to sympathetic deprivation; a new clinical syndrome. Br Med J. 1948; 2: 671-673.
- Mander R, Smith GD. A systematic review of medical diagnosis of Ogilvie’s syndrome in childbearing: Midwifery. 2010; 26: 573-578.
- Zeba M, Tahir AM, Asad M. Ogilvie’s Syndrome (Acute Colonic Pseudo- Obstruction) After Caesarean Section; Journal of the College of Physicians and Surgeons Pakistan. 2013, 23: 298-300.
- Roberts CA. Ogilvie’s syndrome after cesarean delivery. Journal of Obstetric, Gynecologic and Neonatal Nursing. 2000; 29: 239-246.
- Ali Jabbir Shakir, Sajid MS, Kianifard B. Ogilvie’s syndrome-related right colon perforation after cesarean section: A case series. Kaohsiung Journal of Medical Sciences. 2011; 27: 234-238.
- Srivastava G, Pilkington A, Nallala D. Ogilvie’s syndrome: a case report: Arch GynecolObstet. 2007; 276: 555-557.
- Noory N, Abbaszadeh E. Cecal dilatation and perforation after cesarean section: International Journal of Gynecology and Obstetrics. 2003; 81: 47-48.
- Kotsev S. Ogilvie’s syndrome following cesarean delivery: the Dubai’s case. Saudi J Anaesth. 2011; 5: 335-338.