Abstract
Background: Communication during the End of Life (EOL) is essential for successful navigation through the end of life continuum. However, critical care nurses’ communication during EOL is a phenomenon with limited research.
Objective: This study’s objective was to describe critical care nurses’ perceptions concerning their EOL communication in a tertiary teaching hospital.
Methods: A cross-sectional study was used. Fifty-four critical care nurses were recruited using simple random sampling between December 2014 and February 2015. A 20-item caring for Terminally Ill Patients Nurse Survey (CTIPNS) questionnaire was employed to collect the data. Data was analyzed using SPSS 22.0 for descriptive and inferential analysis.
Results: The mean perception of EOL communication score was 3.28 (SD 0.20). A significant association was found between the critical care nurses’ perceptions of EOL communication and working experience (p = 0.04).
Conclusion: Working experience influences critical care nurses’ perceptions of EOL communication. It can be concluded that specific nursing education programs such as those offered by the EOL Nursing Education Consortium should continue to improve the capacity of critical care nurses to deliver quality EOL communication to dying patients and their families.
Keywords: Critical care nurses; Perception; End of life; Communication; Dying
Introduction
Communication is a central element of nursing to provide Endof- Life (EOL) care. All nurses will at some point be required to care for patients who are dying and communication is the key to doing this efficiently. Good communication enables nurses to establish the patient’s priorities and wishes, and to support them to make informed decisions about healthcare. It also provides an opportunity to explore any anxieties or gaps in understanding of the situation, reassure patients and their families, and alleviate anxiety and distress. Good communication allows patients and their families to prepare for the future, and to express and meet their preference for EOL care [1]. Ironically, all too often good EOL communication is not achieved [2]. Dying is the final portion of the life cycle for a human. Barriers to EOL communication among nurses include uncertainty about prognosis, which can make nurses reluctant to discuss EOL care with their patients in a clinical environment [3]. This is particularly the case for patients with non-cancer conditions, which are often characterized by relapses and remissions, and have a less predictable dying phase. In some instances, if a patient is faced with a serious illness and little time to live, they may choose to prioritize quality of life over extending the amount of time left, while acknowledging the uncertainty of their situation [4]. A descriptive correlational survey study on 31 oncology nurses in a Magnet-designated hospital in Southern California has shown that despite nurses having fairly positive attitudes toward hospice and engaging in discussions about prognosis with terminally ill patients, they reported missed opportunities for discussions and patient referrals to hospice [5]. There is scant literature regarding critical care nurses’ perceptions of EOL communication in acute care settings. Several early studies focused on nurses caring for patients who were nearing the EOL [6- 9]. Critical care nurses were found to experience various emotions, feelings, and thoughts as they faced EOL issues in the critical care unit. While providing important information, these studies were limited to patients with terminal diagnoses.
Relatively little is known about how critical care nurses perceive EOL communication in Malaysia. It is thus important to investigate this issue. This paper reports a study that sought to fill this gap in knowledge at the local level and share it at the international level to contribute to the evidence base for informing future critical care nursing practice when dealing with EOL communication.
Methods
Design, settings, and participants
A cross-sectional research design was employed for the purpose of determining critical care nurses’ perceptions of EOL communication in a tertiary teaching hospital in Malaysia between December 2014 and February 2015. The sample size was determined through Power and Sample (PS) Size calculation software and based on the 95% confidence interval and 80% power in Boyd, Merkh, Rutledge and Randall’s 2011 study [5]. This was done to ensure the accuracy of the sample by avoiding sampling errors, and to determine the sample’s representativeness and parameters. Using the PS calculation, the sample size was 54 participants. Simple random sampling was undertaken using the Microsoft Excel software to recruit eligible study participants. Participants were eligible if they had at least one year of critical care nursing experience and were willing to participate. Participants were excluded if they were unavailable during the data collection period for reasons such as maternity leave or study leave.
Data collection
Data was collected using the 20-item Caring for Terminally Ill Patients Nurse Survey (CTIPNS)developed by Boyd et al. [5], which has been tested for validity and reliability (Cronbach a = 0.7). The dependent variables were critical care nurses’ perceptions of EOL communication, while the independent variables were demographic information including age, gender, years of working experience, and level of nursing education. The CTIPNS questions require Likert-type responses ranging from 1 (strongly agree) to 5 (strongly disagree). On the Likert-type items, higher scores indicate more agreement regarding EOL communication. The main researcher, who knew the system of this critical care service, collected data after shift work.
Ethical considerations
The participating hospital and the researchers’ institution approved the study in accordance with their ethical guidelines. Permission to use the Caring for Terminally Ill Patients Nurse Survey (CTIPNS) questionnaire was sought and granted from its original author. Participants who met the research inclusion criteria were given information about the research, and participation was voluntary.
Data analysis
Statistical analyses were conducted using the Statistical Package Social Sciences (SPSS) software version 22. Descriptive statistics were used to describe frequencies and measures of central tendencies. Associations among selected demographic data (age, gender, years of working experience, and level of nursing education) and nurses’ perceptions were calculated using Pearson’s correlation coefficients, independent t-test, and one-way ANOVA. The significance level was set at 0.05.
Results
Participant characteristics
Table 1 describes the demographic characteristics of the 54 critical care nurses who participated in the study. The majority (66.7%) were females, while 33.3% were males. Most of the nurses’ ages fell between 25-30 years old (40.7%). More than half of the nurses had one to five years’ working experience in critical care nursing. Only two nurses had a Bachelor’s Degree, four had a Post Basic Diploma, while the rest had a Diploma as their highest level of nursing education.
Critical care nurses’ perceptions of EOL communication
Critical care nurses’ perceptions of EOL communication were measured using the 5-point Likert scale. The six domains of perception tested are presented in Table 2. The mean score for self-rated perception was 3.36, while comfort with initializing had the lowest mean score of 2.65. The mean score for benefit of communication to patients was 3.46, while perceived doctors’ comfort and responsibility was 3.23. The mean score for perceived patients’ perception was 3.28, and the highest mean score (3.72) was recorded for palliative care team.
Figure 1 shows that the overall, the nurses’ perception of EOL communication was “good”. The mean perception score for all 54 respondents was 3.28, with a standard deviation of 0.20. The distribution of data was positively skewed. The median (3.25) is slightly lower than the mean.
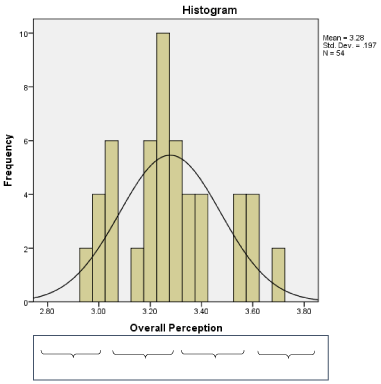
Figure 1: Critical care nurses’ overall perception of EOL communication.
Association between critical care nurses perceptions of EOL communication and their demographic variables
One-way ANOVA analysis revealed a significant association between years of clinical working experience in nursing and nurses perceptions of EOL communication (p=0.04). There was no significant association between critical care nurses perceptions of EOL communication and their age (p=0.055), gender (p=0.39), or highest nursing educational level (p=0.22). This study highlighted that critical care nurses with more years of working experience in nursing scored higher for perception than those with lesser years of working experience (Table 3).
Discussion
The majority of the critical care nurses were female, aged between 25 and 30 years, had a diploma level of nursing education, and less than five years of critical care experience in nursing. The reason that there were a higher percentage of female nurses in the study probably due to the fact that nursing is a female-dominated career. This finding corroborates the argument of Mead us and Twomey [10], which purported that little change has occurred in gender representation in relation to female-dominated employment; and no field better exemplifies this situation than nursing. This finding is also in agreement with Hsu et al [7], who indicated that nursing was established as a womens profession. However, the findings of the current study differ from Massaroli et al.s study [11], which is predominantly of the male gender. These findings may help us to understand that despite more men entering the career of nursing and adding diversity to the workforce, nurses are typically regarded as female.
As for the participants age, the fact that the majority were between 25 and 30 years old indicates they were a young population; a finding similar to Preto and Pedraos study [12] performed in ICUs, in which 47.6% of nurses were in the young age group, leading to the conclusion that younger nurses are those who get more involved in high complexity healthcare disciplines. This finding also matches those observed in Happ et al.s study [13]. There are several possible explanations for this finding. Younger nurses may desire most intensely to work in the critical care unit to develop their professional skills, or when these health care professionals come to older age, they are absorbed into other less complex areas such as clinics or administrative positions.
This studys findings corroborate those expressed by Boyd et al [5]. Critical care nurses in the present study reported experiencing difficulties initializing conversations about EOL. The finding that the aspect of comfort with initializing had the lowest perception mean score (2.65) among the six domains demonstrates that critical care nurses barely met the “satisfy” level regarding their initiative in EOL communication. One of the challenges for them was their in ability to make an appropriate, sensitive assessment of the patient – whether he or she is ready for a conversation about death and dying – and then to be supportive of the person whether they are ready to talk or not. There are similarities between the perceptions expressed by critical care nurses in this study and those described by Fitch [14], where critical care nurses faced EOL communication challenges when dealing with critically ill patients within a clinical situation. This finding may be explained by the supposition that EOL communication between nurses, patients and families can be perplexing, therefore further interventions with critical care nurses may enhance future EOL communication.
The present study revealed that nurses with more years of clinical experience in the nursing field scored higher on the perception scale than those with lesser years of working experience. Therefore, it can be suggested that nurses with years of clinical experience were better able to engage in EOL communication. These findings are consistent with Hebert, Moore and Rooneys study [15], which found that nurses who lack clinical experience specifically in EOL care may not readily see the needs of these patients and their families. Hence, experience may positively influence nurses advocacy behaviors [15]. This also accords with Braun, Gordon, and Uziely [16], who suggested that nurses working experience may in hibit emotions that may adversely affect their information-giving for dying patients. The present studys findings seem to be consistent with Thacker [17], who found that novice nurses reported a lack of communication as a barrier to their practice of advocacy.
Culture has often been identified as the root of communication challenges, and can act as both a facilitator and a barrier to communication [18]. For this reason, it seems possible that the lack of EOL communication may be explained by the perception in many Asian cultures that directly informing a patient of a cancer diagnosis is unnecessarily cruel. Furthermore, most nurses perceive significant barriers to effective communication, some as a result of active decisions on their part, and some beyond their control [19]. As suggested by Li, Ang, and Hegney [20], effective communication is an important aspect of patient care that improves the nurse-patient relationship, and has a profound effect on the patients perceptions of health care quality and treatment outcomes. A possible explanation for these findings may be that few people engage in conversation about EOL issues. In addition, communication styles are different for people from different ethnic groups. Therefore, the need for effective EOL communication is essential to achieve the patients desired outcomes at the EOL.
Strengths and Limitations
Potential generalizability of the findings was increased by random selection of critical care nurses for participation in the study. The Caring for Terminally Ill Patients Nurse Survey (CTIPNS) questionnaire was considered valid for investigating the critical care nurses perceptions of EOL communication. This study was limited to one critical care unit in one tertiary teaching hospital in Northeast Peninsular Malaysia. Therefore, this studys findings may not reflect the perceptions of critical care nurses in other settings (for example, those in West Coast Malaysia).
Conclusion
This study highlights that working experience influences critical care nurses perceptions of EOL communication. Ongoing development of communication skills related to discussing EOL among critical care nurses, patients and families is needed to create abetter understanding of a patients values and treatment preferences, which will lead to a care plan consistent with these. It can be concluded that specific nursing education programs such as those offered by the EOL Nursing Education Consortium should continue to improve the capacity of critical are nurses to deliver quality EOL communication to dying patients and their families.
Acknowledgement
We would like to thank all the critical care nurses who kindly volunteered to participate in the study. We also would like to thank Professor Dana N. Rutledge for permission to use the CTIPNS instrument.
References
- Sleeman KE. End-of-life communication: lets talk about death. Roy. Coll Physician. 2013; 43: 197-199.
- Mayor S. Care of dying patients and safety dominate report on NHS complaints. BMJ. 2007; 334: 278.
- Heaven C, Clegg J, Maguire P. Transfer of communication skills training from works place: The impact of clinical supervision. Patient Education and Counseling. 2006; 60: 313-325.
- Higginson IJ, Gomes B, Calanzani N, Gao W, Bausewein C, Daveson BA, et al. Priorities for treatment, care and information if faced with serious illness: a comparative population-based survey in seven European countries. Palliat Med. Forthcoming. 2013.
- Boyd D, Merkh K, Rutledge DN, Randal V. Nurses perceptions and experiences with end-of-life communication and care. Oncol Nurs Forum. 2011; 38: 229-239.
- Bradley EH, Cherlin E, McCorkle R, Fried TR, Kasl SV, Cicchetti DV, et al. Nurses use of palliative care practices in the acute care setting J Prof Nurs. 2001; 17: 14-22.
- Hsu H, Chen SH, Yu HY, Lou HJ. Job stress, achievement motivation and occupational burnout among male nurses. JAdv Nurs. 2010; 66: 1592-1601.
- Ferrell B. Beyond the Supreme Court decision: nursing perspectives on endof- life care. Oncol Nurs Forum. 2000; 27 : 445-455.
- Thompson G. Nurses perceptions of quality end-of-life care on an acute medical ward. J Adv Nurs. 2006; 53: 169-177.
- Meadus RJ, Twomey J. Men Student Nurses: The Nursing Education Experience. Nurs Forum. 2011; 4: 269-279.
- Massaroli RR, Martini JG, Massaroli A, Lazzari DD, de Oliveira SN, Bruna Canever P. Nursing work in the intensive care unit and its interface with care systematization. Esc. Anna Nery. 2015; 19.
- Preto VA, Pedrao LJ. Stress among nurses who work at the intensive care unit. Rev Esc Enferm USP. 2009; 43: 841-848.
- Happ MB, Garrett K, DiVirgilio Thomas D, Tate J, George E, Houze M, et al. Nurse-patient communication interactions in the intensive care unit. Am J Crit Care. 2011; 20: e28-40.
- Fitch MI. Understanding Oncology Nurses Experiences Talking About Death and Dying.
- Hebert K, Moore H, Rooney J. The nurse advocate in end-of-life care. The Ochsner J. 2011; 11: 325-329.
- Braun M, Gordon D, Uziely B. Associations between Oncology Nurses Attitudes toward Death and Caring for Dying Patients. Oncol Nurs Forum. 2010; 37: E43-E49.
- Thacker K. Nurses advocacy behaviors in end-of-life nursing care. Nurs Ethics. 2008; 15: 174-185.
- Okougha M, Tilki M. Experience of overseas nurses: The potential for misunderstanding. BJN. 2010; 19: 102-106.
- Adam AM, Mannix T, Harrington A. Nurses communication with families in the intensive care unit – a literature review. Nurs in Crit Care. 2015; 22: 70-80.
- Li H, Ang E, Hegney D. Nurses perceptions of the barriers in effective communicaton with impatient cancer adults in Singapore. J Clin Nurs. 2012; 21: 2647-2658.
