
Research Article
Austin J Nutri Food Sci. 2018; 6(1): 1097.
Oxidative Stress and Biochemical Parameters in Childhood Obesity
Marcela AS¹*, Tarraf HS², Nicoletti CF¹, Percário S³, Oliveira BAP¹, Oliveira CC¹, Gregório ML², Pinhanelli VC² and Dorotéia RS²
¹Department of Internal Medicine, Faculty of Medicine of Ribeirao Preto, University of São Paulo Ribeirão Preto, Brazil
²Department of Molecular Biology, Faculty of Medicine of São Jose do Rio Preto. São Jose do Rio Preto - SP, Brazil
³Research on Oxidative Stress Laboratory, Federal University of Pará. Belém, Brazil
*Corresponding author: Marcela Augusta de Souza Pinhel, DepartmentofInternal Medicine, Ribeirao Preto Medical School, Universityof São Paulo, Ribeirão Preto - SP, Brazil. Avenida dos Bandeirantes, 3900. Ribeirao Preto, SP, Brazil
Received: January 08, 2018; Accepted: February 02, 2018; Published: February 20, 2018
Abstract
Aim: Obesity in children has been associated with increased oxidative stress a factor that may play a key role in the pathophysiology of cardiovascular and metabolic events of obesity. The main aim this study was to analyze risk predictors for Cardiovascular Disease (CVD) including lipid profile and oxidative stress in children with and without obesity and the correlation between sedentary lifestyle and breastfeeding history.
Methods: Were enrolled 66 children randomized into two groups: G1: 35 children with obesity and G2: 31 children with normal weight. Anthropometric, biochemical, personal and family history data were collected, besides a peripheral blood sample. Statistical analysis included t, Fisher tests and Pearson correlation. Significance level was assumed for p<0.05.
Results: The mean age of G1 was 8±1.5 years and Body Mass Index (BMI) of 25.6±2.5 kg/m². For G2 mean age of 7±1.4 years and BMI 16.5±1.4 kg/m². It was observed that G1 had higher TG and malondialdehyde (MDA) levels compared to G2 (p<0.05). It was noted positive correlation between MDA levels, TG and VLDLc only in the obese group (p<0.0001). Children with normal weight and breastfeeding have higher levels of HDLc.
Conclusion: High levels of TG and MDA are associated with obesity. Breastfeeding history associated with high levels of HDLc in normal weight children, suggests its protective effect for CVD. We suggest that pediatricians should be aware of the importance of assessing the degree of oxidative stress in children with obesity in an attempt to prevent the development of comorbidities.
Keywords: Oxidative stress; Obesity; Childhood; Cardiovascular diseases
Introduction
The increase in the number of children with obesity is a major health problem, mainly because of its association with comorbidities, including atherosclerosis and type 2 diabetes mellitus; factors that can lead the development of cardiovascular disease [1]. It is estimated that in Brazil the prevalence of childhood obesity is approximately 16.6% in boys and 11.8% in girls, probably due to high consumption of highcalorie foods and beverages and reduced physical activity [2].
Obesity in children is one of the risk factors for obesity in adults and for the development of chronic diseases during childhood and adulthood [3]. Cardiovascular Diseases (CVD) are responsible for high mortality in Brazil, requiring further clarification, especially in children. There is an association between plasma cholesterol levels and mortality from cardiovascular disease [4], and among the main risk factors for CVD are high concentrations of low-density lipoprotein (LDLc) and low concentrations of high-density lipoprotein (HDLc) [5].
Moreover, other mechanisms that link obesity to the CVD have been widely investigated and include the state of inflammation and oxidative stress resulting from the increased adipose tissue [5,6]. Thus, obesity in children has been associated with increased oxidative stress [7], a generated condition when the production of reactive oxygen species exceeds the body’s ability to remove them. Thus, the increased oxidative stress may play a key role in the pathophysiology of cardiovascular and metabolic events of obesity8 and contributing to the development of obesity-related comorbidities [8].
However, the oxidative process remains to be elucidated. The investigation of biomarkers may contribute to early diagnosis of the implications of childhood diseases. It limited the number of studies on the oxidative damage caused by obesity in childhood; however associations between oxidative stress and diseases related to obesity, such as hypercholesterolemia [9] and insulin resistance [10] are being reported in children.
In this context, the present study aimed to analyze risk predictors for CVD including lipid profile and oxidative stress in children with and without obesity by sex and age and the correlation between the presences or absence of a sedentary lifestyle, breastfeeding history and background family of CVD.
Material and Methods
For the present study, 66 children with age between 5 and 10 years, of both sexes were enrolled in a Basic Health Unit Care. It is case-control study in which children were randomized into two groups according to nutritional status: Group 1 (G1): 35 children with obesity and Group 2 (G2): 31 children with normal weight. Children with heart diseases, metabolic diseases, and genetic disorders associated with dyslipidemia and in use of medication were excluded. This study was approved by the Ethics Committee of the institution. Parents or guardians were informed about the study and their consent was obtained.
Anthropometric, biochemical and personal and family history data were collected in a single moment. The anthropometric assessment was based on measurements of weight and height and calculate Body Mass Index (BMI). Weight was measured with a mechanical scale (capacity of 150 kg and 0.1 kg of precision) and height was measured with vertical stadiometer (graduation 0.1 cm). BMI (kg/m2) was calculated by the formula weight (kg) / height2 (m) and their values applied in graphic NCHS (National Center for Health Statistics) [11] according to gender and age to determine the nutritional status. For evaluation of personal history, lifestyle habits, comorbidities and breastfeeding applied specific questionnaire.
Peripheral blood samples were collected after 12 hours of fasting for lipid profile analysis including serum total cholesterol (TC) and its fractions, LDLc, HDLc, very low density lipoprotein (VLDL-c) and triglycerides (TG) and stress oxidative analysis by measuring levels of malondialdehyde concentration (MDA). Serum concentrations of lipid fractions were performed by colorimetric enzyme method. The serum MDA concentration was performed according to the method of Khon & Liversedg [12], considering as normal limits serum 0-440 ng/dL.
Statistical analysis
The data were presented as mean ± standard deviation. The Kolmogorov-Smirnov test was performed to verify the normality of the data. Groups of children with obesity and normal weight were compared by applying the t test for independent samples. The Fisher exact test was used to check the frequency of altered biochemical markers in groups considering gender, age and BMI. The Pearson correlation coefficient was used to correlate variables related to the lipid profile, MDA and age. It is also applied multivariate principal component analysis compared the variables TC, HDLc, LDLc, VLDLc and MDA, in order to determine the association of factors between those variables. To verify the effect of other dichotomous variables (presence or absence of a sedentary lifestyle, breastfeeding, CVD history and gender) applied the t test. Significance level was assumed for p<0.05.
Results
Group 1 consisted of 35 children with a mean age of 8±1.5 years, 40% of female, with an average BMI of 24.3±3.1 kg/m² and 21 (60%) male with BMI 25.6±2.5 kg/m&su. The group 2 included 31 normal weight children with mean age of 7±1.4 years, predominantly male (61%), BMI 16.5±1.4 kg/m². Indeed for group 2, females (39%) had BMI 16.6±2.3 kg/m².
It was observed that the group with obesity had higher TG levels (108.8±44.3 mg/dL) and VLDL-c (21.7±8.9 mg/dL) compared to normal weight group (81.5±49, 5 mg/dl, 16.3±9.9 mg/dL, respectively, p=0.02 for both). However, both groups showed similar levels of LDLc, HDLc and CT (Table 1). Also, there was a higher frequency of individuals with altered levels of VLDL-c (51.4%) and TG (51.4%) in the obese group compared to normal weight (22.6%; p=0.02 for both variables).
Variables of lipid profile (mg/dL)
Children with obesity (n=35)
Children with normal weight (n=31)
p*
CT
171.7±30
164.2±29.2
0.14
LDLc
91.8±26.4
90.4±28.3
0.58
HDLc
58.8±13.7
57.5±12.5
0.17
VLDLc
21.7±8.9
16.3±9.9
0.02
TG
108.8±44.3
81.5±49.5
0.02
*T test; p: level of significance; n: number of individuals; CT: total cholesterol; LDLc: cholesterol fraction of low-density lipoprotein; HDLc: high-density lipoprotein cholesterol fraction; VLDLc: cholesterol fraction of very low density lipoprotein; TG: triglycerides
Table 1: Lipid profile of children with obese and normal weight.
Among normal individuals, women showed higher frequency of increased serum concentrations of CT (67%) and LDLc (50%) compared to men (21%, 5%, p=0.02; p=0.007, respectively). The comparative analysis between the group with obesity and normal weight, according to sex, showed high frequency of LDLc in males with obesity (33%), as compared to healthy (5%; p=0.04) (Table 2).
Variables of lipid profile (mg/dL)
Children with obesity (n=35)
Children with normal weight (n=31)
Total
Male (n=21)
Female (n=14)
p1*
Total
Maale (n=19)
Female (n=12)
p2*
p3*
p4*
p5*
n
%
n
%
n
%
n
%
n
%
n
%
CT
20
57
10
48
10
71
0,29
12
39
4
21
8
67
0,02
0,14
0,10
1,00
LDLc
11
31
7
33
4
29
1,00
7
23
1
5
6
50
0,007
0,58
0,04
0,42
HDLc
1
3
1
5
0
0
1,00
4
13
2
11
2
17
0,63
0,17
0,59
0,20
VLDLc
18
51
10
48
8
57
0,73
7
23
4
21
3
25
1,00
0,02
0,10
0,13
TG
18
51
10
48
8
57
0,73
7
23
4
21
3
25
1,00
0,02
0,10
0,13
*Fisher test; p: level of significance; n: number of individuals; CT: total cholesterol; LDLc: cholesterol fraction of low-density lipoprotein; HDLc: high-density lipoprotein cholesterol fraction; VLDLc: cholesterol fraction of very low density lipoprotein; TG: triglycerides p1: comparison between genders in obesity group; p2: comparison between genders in eutrophic group; p3: comparison between groups (total); p4: male comparison between groups; p5: female comparison between groups
Table 2: Frequency of children with abnormal concentrations of lipids in the groups of children with obesity and normal weight.
There was higher serum concentrations of MDA in the obese group (939.9±2.464 ng/mL) compared to normal weight (434.1±228.3 ng/mL; p=0.03). The comparative analysis between groups considering gender, revealed similar concentrations among obese boys (560.3±1.285.7 ng/ml) and normal (484.1±1171.2 ng/mL; p=0.49); however girls of obesity group showed higher levels of MDA (583.0±1.543 ng/mL) compared to normal weight (327.4±640.3 ng/ mL; p=0.02).
Figure 1 shows the MDA correlation coefficients with the lipid profile. It was noted positive correlation between MDA levels, TG and VLDL-c only in the obese group (r=0.61; p<0.0001 for both correlations). There was no correlation between age and MDA.
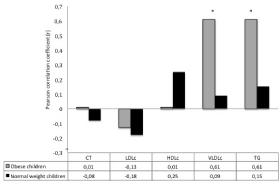
Figure 1: Correlation coefficients (r) between lipid profile variables and levels
of malondialdehyde (MDA) in individuals with obesity and normal weight. CT:
total cholesterol; LDLc: cholesterol fraction of low-density lipoprotein; HDLc:
cholesterol fraction of high-density lipoprotein; VLDLc: cholesterol fraction of
very low-density lipoprotein; TG: triglycerides; *: p<0.05 (Pearson correlation).
Multivariate principal component analysis compared the variables HDLc, LDLc, TG, VLDL-c and MDA was performed. In the obesity group, factor 1 explained with 43.1% of the total variation. This factor accounted for individuals with high or low levels of MDA, TG and VLDL-c together. In this same group, factor 2 explained 30.3% of variation in the sample and identified individuals with reduced or increased levels of TC and HDL-c together. Factor 3 which associated increased concentrations of LDLc and reduced levels of HDLc or vice versa, explained 18% of the total variation of biochemical indicators in this group.
Among normal weight individuals, Factor 1 represented by the increase or decrease in CT concentrations, LDLc, TG and VLDL-c together explained 42.8% of the total variation. Factor 2, identified by increased levels of TC and LDLc and reduced MDA, TG and VLDL-c or vice versa, contributed 24.7% of total variation in this group. Factor 3 accounted for 20.5% of the total variation, characterized by increasing or decreasing concentrations of TC, HDL-c and MDA together.
In each group the respective factors 1, 2 and 3 were associated with sex, family history of CVD, physical inactivity, and breastfeeding and the results of which are shown in (Tables 3 and 4), for the groups with or without obesity, respectively. In the group of eutrophic children the Factor 2 stood out, with a value of 0.85±0.87, indicating significantly higher concentrations CT and LDLc and reduced MDA, TG and VLDL-c in females as opposed to males (Factor 2=-0.53±1.11; p=0.001). For the other variables there was no significant difference between groups (p>0.05). The relationship of these variables with Factor 3, which is in the normal weight increase or decrease the levels of TC, HDL-C and MDA identified for breastfeeding significantly high levels of these variables (Factor 3=0.31±1.09) compared to the absence breastfeeding (Factor 3=-0.49±0.31; p=0.047; Table 4).
Factors
Gender
History of CVD
Sedentary lifestyle
Breastfeeding
Female
Male
Yes
No
Yes
No
Yes
No
(n=14)
(n=21)
(n=8)
(n=27)
(n=21)
(n=14)
(n=18)
(n=17)
Factor 1
0,39±1,28
-0,26±1,78
0,01±1,48
-0,00±1,67
0,35±1,59
-0,53±1,55
-0,38±1,53
0,40±1,64
p</span>*
0,219
0,977
0,113
0,158
Factor 2
-0,32±1,29
0,22±1,38
0,25±1,32
-0,07±1,37
0,11±1,36
-0,16±1,37
-0,01±1,28
0,01±1,46
p*
0,249
0,556
0,572
0,964
Factor 3
0,05±1,12
-0,03±1,01
0,21±1,26
-0,06±0,98
0,18±1,09
-0,27±0,93
-0,04±0,94
0,05±1,16
p*
0,824
0,595
0,204
0,803
*T test; Factor 1: Increase or decrease of MDA levels, TG and VLDL-c; Factor 2: increase or decrease in levels of TC and LDLc; Factor 3: increased levels of LDLc and reduced levels of HDLc or vice versa. CT: total cholesterol; LDLc: cholesterol fraction of low-density lipoprotein; HDLc: cholesterol fraction of high-density lipoprotein; VLDLc: cholesterol fraction of very low-density lipoprotein; TG: triglycerides; CVD: cardiovascular disease; p: significance level.
Table 3: Correlation of the major components identified as factors 1, 2 and 3 and the personal history for obesity group in both genders.
Factors
Gender
History of CVD
Sedentary lifestyle
Breastfeeding
Female
(n=12)
Male
(n=19)
Yes
(n=12)
No
(n=19)
Yes
(n=20)
No
(n=11)
Yes
(n=19)
No
(n=12)
Factor 1
-0,53±1,65
0,33±1,52
-0,04±1,49
0,02±1,71
0,19±1,63
-0,35±1,57
0,16±1,54
-0,26±1,74
p*
0,161
0,921
0,370
0,496
Factor 2
0,85±0,87
-0,53±1,11
0,13±1,65
-0,08±0,88
0,15±1,21
-0,27±1,24
0,19±1,16
-0,30±1,29
p*
0,001
0,678
0,368
0,295
Factor 3
-0,08±1,06
0,05±1,16
-0,25±0,791
0,16±1,26
-0,08±1,22
0,15±0,907
0,31±1,09
-0,49±0,31
p*
0,748
0,275
0,562
0,047
*T test; Factor 1: Increase or decrease the levels of TC, LDLc, TG and VLDL-c; Factor 2: increased levels of TC and LDLc and reduced MDA, TG and VLDL-c or vice versa; Factor 3: increased levels of LDLc and reduced levels of HDLc or vice versa. TC: total cholesterol; LDLc: fraction of cholesterol low-density lipoprotein; HDLc: cholesterol fraction of high-density lipoprotein; VLDL-C: fraction of cholesterol and very low-density lipoprotein; TG: triglycerides; CVD: cardiovascular disease; p: significance level
Table 4: Correlation of the major components identified as factors 1, 2 and 3 and the personal history of eutrophic group in both genders.
Discussion
This study confirms the association between obesity and high levels of TG and VLDL-c and oxidative stress in childhood, in positive correlation with MDA levels. The current epidemic of obesity among children has increased the need for health professionals to know risk factors for CVD and implement changes aimed at preventing this disease or early clinical intervention5. Admittedly, childhood obesity is a complex disease with different genetic components; metabolic, environmental and behavioral factors are interrelated, making it difficult to define the causal pathways.
Although recognized that atherosclerosis develops in childhood, the determinants of this preclinical phase still remain unclear. Freedman et al. [13] in a study of students between 5 and 17 years of age found that overweight individuals were more likely to present altered concentrations of CT and its fractions and TG.
In this study, the altered concentrations of TC and LDLc were more frequent in females, corroborating other studies that confirm higher frequency of high levels of TC in girls (37.5 and 32.2%) compared to boys (32.4 and 29.2%) [14]. Risk factors for obesity modify up according to age and may depend on the timing of sexual maturation, differences in locations, sample size and cultural or socioeconomic causes [14,15].
In relation to nutritional status in this study, children with obesity had higher concentrations of VLDL-c and TG compared to normal weight children. Moreover, obese male children showed higher frequency of high levels of LDLc to the controls of the same sex, corroborating with a Brazilian study, which showed that 50% of overweight boys had undesirable levels of LDLc [9]. Although the present study did not show difference in CT concentrations between groups, Friedland et al. [16] found TC and TG concentrations higher in obese compared with eutrophic; however does not detect the degree of obesity effect in the lipid profile, whereas a BMI between 85 and 95 % compared to values above 95%. However, controversy is a causal relationship between obesity and hypercholesterolemia, being relatively common observation of individuals with severe obesity and desirable concentrations of CT [17].
In this study there was no difference of LDLc and HDLc concentrations between groups with obesity and normal weight. However, Lamb et al. [18], in the analysis of risk factors for clinical and metabolic complications among adolescents with obesity, highlighted lower levels of HDL-c in obese compared with nonobese, results in agreement with other studies [8,17].
It was observed in this study, higher concentrations of MDA in children with obesity compared to normal weight, corroborating studies in Brazilian17 and Spanish children [19]. In contrast, reduced MDA values were observed in a study of children with severe obesity compared to normal children [20]. Lima et al. [9] also observed that high concentrations of MDA are more prevalent in males, contrasting with the findings of this study, which revealed a similarity of MDA concentrations between the genders.
This study showed MDA values within the desirable limit in normal children, disagreeing with the findings of Lima et al. [9]. MDA is one of the most abundant aldehydes resulting from tissue lipid peroxidation, enabling the indirect analysis of the resulting oxidative damage of lipid peroxidation [19]. Obesity in children has been linked to increased oxidative stress, which favors the development of comorbidities [8]. Previous studies have shown that the degree of childhood obesity is closely related to cardiovascular morbidity in the adult21. Adverse cardiovascular outcomes are more likely when several risk factors are present. Recently, it has been suggested that an evaluation of the oxidative state can help to identify patients at increased risk for subsequent cardiovascular and metabolic complications [22].
Targets phospholipids on the particle surface of LDLc, and lipid particle and internal proteins are exposed to oxidation with consequent formation of oxidized LDL (oxLDL) and accumulation of byproducts such as MDA [23], which is often used as a marker oxidative stress. In this context, it is disturbing the findings of this study showing the high frequency of children with increased levels of LDLc in the groups with (31.4%) or without obesity (22.6%), although the average levels of LDLc in both groups remained in the desirable limit.
Further, the BMI is associated not only with increased oxidative stress, but also with high systemic inflammation and activation of the coagulation cascade [24,25]. The elevation of coagulation factors and, therefore, blood hypercoagulability may be associated with hypertriglyceridemia [24]. This confirms the importance of controlling TG levels in childhood, especially children with obesity that in the present study showed increased concentrations of TG, considered an independent risk factor for CVD in positive correlation with levels of VLDL-c and MDA.
The main cause of increased oxidative stress in individuals with obesity is not yet fully elucidated. The Framingham Heart Study [26] confirms the association between markers of this process and BMI and waist / hip ratio, adiposity is the main factor, suggesting that higher fat mass also determines greater degree of oxidative stress [27]. Other factors in addition to oxidative stress should be highlighted for obesity. In this study, multivariate principal component analysis identified the association between changes in the lipid profile and MDA and the correlation with sex, sedentary lifestyle, breastfeeding and familial history of CVD. Thus it was possible to identify the profile of children with and without obesity. In this context, it is possible that exercise, in addition to power, influencing the total body fat by their effect on fat tissue and intracellular TG, can reduce systemic inflammation and oxidative stress [19,27], in order that adipocytes produce cytokines that stimulate the oxidative pathway [27].
In this study, considering the equivalent factors the combinations of variables was also related to breastfeeding, suggesting greater protection against oxidative stress and cardiovascular disease in children with obesity. Thus, it is likely that exclusive breastfeeding for more than four months is associated with slower weight gain during the second semester of the first year, which could be part of the reason behind the reduced risk of later overweight or obese [28]. There is also evidence that breastfeeding provides likely beneficial effects on blood pressure and blood cholesterol levels in adulthood [28].
Given the association between obesity, cardiovascular disease and family history of CVD in this study as well as in clinical studies in general, these data were recorded based on the parent information, becoming a limiting factor in the data analysis. The potential risk factor for child becoming obese, with consequent chronic complications, is the sum of genetic influences and environmental factors such as eating habits and family lifestyle [13]. The literature is scarce in relation to the prevention studies involving obesity, dyslipidemia and markers of lipid peroxidation, especially in children and adolescents [9,10,19]. Weight loss programs, including diet and physical activity should be encouraged in childhood to reduce the risk admittedly increased cardiovascular diseases.
In conclusion, data from this study shows that high levels of TG and MDA are associated with obesity in childhood, increasing the risk for CVD in men with also increased levels of LDLc. Moreover, in females, increased age is related to higher degree of obesity, suggesting that controlling for BMI may delay the manifestation of CVD and that for normal weight children to breastfeeding history associated with high levels of HDL-c, suggests its protective effect for CVD. Like other authors [8], we suggest that pediatricians should be aware of the importance of assessing the degree of oxidative stress in children with obesity in an attempt to reverse this condition as soon as possible and thereby preventing the development of comorbidities.
References
- Codoñer-Franch P, López-Jaén AB, De La Mano-Hernández A, Sentandreu E, Simó Jordá R, Valls-Bellés V. Oxidative markers in children with severe obesity following low-calorie diets supplemented with mandarin juice. Acta Paediatr. 2010; 99: 1841-1846.
- Instituto Brasileiro de Geografia e Estatística. Pesquisa de Orçamentos familiares 2008-2009. Antropometria e estado nutricional de crianças, adolescentes e adultos no Brasil. Rio de Janeiro, 2010.
- Allcock DM, Gardner MJ, Sowers JR. Relation between Childhood Obesity and Adult Cardiovascular Risk. Int J Pediatr Endocrinol. 2009; 108187.
- Kelishadi R, Zadegan NS, Nadery GA, Asgary S, Bashardoust N. Atherosclerosis risk factors in children and adolescents with or without family history of premature coronary artery disease. Med Sci Monit. 2002; 8: 425- 429.
- Codoner-Franch P, Murria-Estal R, Tortajada-Girbés M, del Castillo- Villaescusa C, Valls-Bellés V, Alonso-Iglesias E. New factors of cardiometabolic risk in severely obese children: influence of pubertal status. Nutr Hosp. 2010; 25: 845-851.
- Wildman RP, McGinn AP, Lin J, Wang D, Muntner P, Cohen HW, et al. Cardiovascular disease risk of abdominal obesity vs. metabolic abnormalities. Obesity (Silver Spring). 2011; 19: 853-860.
- Murer SB, Aeberli I, Braegger CP, Gittermann M, Hersberger M, Leonard SW, et al. Antioxidant supplements reduced oxidative stress and stabilized liver function tests but did not reduce inflammation in a randomized controlled trial in obese children and adolescents. J Nutr. 2014; 144: 193-201.
- Codoñer-Franch P, Tavárez-Alonso S, Murria-Estal R, Tortajada-Girbés M, Simó-Jordá R, Alonso-Iglesias E. Elevated advanced oxidation protein products (AOPPs) indicate metabolic risk in severely obese children. Nutr Metab Cardiovasc Dis. 2012; 22: 237-243.
- Lima SCVC, Arrais RF, Almeida MG, Souza ZM, Pedrosa LFC. Perfil lipídico e peroxidação de lipídeos em crianças e adolescentes co m sobrepeso e obesidade. J Pediatr. 2004; 80: 23-28.
- Atabek ME, Keskin M, Yazici C, Kendirci M, Hatipoglu N, Koklu E. Protein oxidation in obesity and insulin resistance. Eur J Pediatr. 2006; 165: 753-756.
- Centers for Disease Control and Prevention. CDC growth charts: United States: percentile data files with LMS values. 2003.
- Khon HI, Liversedge M. On a new aerobic metabolite production by brain is inhibited by apomorhine, emetine, ergotamine, epinephrine and menadione. J Pharamcol Experment Ther. 1944; 82: 292-300.
- Freedman DS, Dietz WH, Srinivasan SR, Berenson GS. The relation of overweight to cardiovascular risk factors among children and adolescents: The Bogalusa Heart Study. Pediatrics. 1999; 103: 1175-1182.
- Kivimäki M, Smith GD, Juonala M, Ferrie JE, Keltikangas-Järvinen L, Elovainio M, et al. Socioeconomic position in childhood and adult cardiovascular risk factors, vascular structure, and function: cardiovascular risk in young Finns study. Heart. 2006; 92: 474-480.
- Zoair AM, Muhammad KT, Abu-Ammo DE, Motawea MM. Lipid profile and some cardiac functions in children with obesity. Egyptian Pediatric Association Gazette. 2013; 61: 15-22.
- Friedland O, Nemet D, Gorodnitsky N, Wolach B, Eliakim A. Obesity and lipid profiles in children and adolescents. J Pediatr Endocrinol Metab. 2002; 15: 1011-1016.
- Hancox RJ, Poulton R. Watching televisin is associated with childhood obesity: but is it clinically important ? Int J Obes (Lond). 2006; 30: 171-175.
- Carneiro JRI, Giugliano R. Fatores associados à obesidade em escolares. J Pediatr. 2004; 80: 17-22.
- Codoñer-Franch P, Tavárez-Alonso S, Murria-Estal R, Megías-Vericat J, Tortajada-Girbés M, Alonso-Iglesias E. Nitric oxide production is increased in severely obese children and related to markers of oxidative stress and inflammation. Atherosclerosis. 2011; 215: 475-480.
- Mohn A, Catino M, Capanna R, Gianini C, Marcovecchio M, Chiarelli F. Increased oxidative stress in prepubertal severely obese children: effect of a dietary restriction-weight loss program. J Clin Endocrinol Metabol. 2005; 90: 2653-2658.
- Clapp BR, Hingorani AD, Kharbanda RK, Mohamed-Ali V, Stephens JW, Vallance P, et al. Inflammation-induced endothelial dysfunction involves reduced nitric oxide bioavailability and increased oxidant stress. Cardiovasc Res. 2004; 64: 172-178.
- Hopps E, Noto D, Caimi G, Averna MR. A novel component of the metabolic syndrome: the oxidative stress. Nutr Metab Cardiovasc Dis. 2009; 20: 72-77.
- Morrow JD, Roberts LJ. The isoprostanes: current Knowledge and directions for future research. Biochem Pharmacol. 1996; 51: 1-9.
- Eckel RH, Barouch WW, Ershow AG. Report of the National Heart, Lung, and Blood National Institute of Diabetes and Digestive and Kidney Diseases Working Group on the Pathophysiology of Obesity-Associated Cardiovascular Disease. Circulation. 2002; 105: 2923-2928.
- Chan JCN, Cheung JCK, Stehouwer CDA, Emeis JJ, Tong PC, Ko GT, et al. The central roles of obesity - associated dyslipidaemia, endothelial activation and cytokines in the metabolic syndrome: an analysis by structural equation modeling. Int J Obes Relat Metab Disord. 2002; 26: 994-1008
- Keaney JF, Larson MG, Vasan RS, Wilson PW, Lipinska I, Corey D, et al. Obesity and systemic oxidative stress: clinical correlates of oxidative stress in the Framinghan Study. Arterioscler Thromb Vasc Biol. 2003; 23: 434-439.
- Fenster CP, Weinsier RL, Darley-Usmar VM, Patel RP. Obesity aerobic exercise, and vascular disease: the role of oxidants stress. Obes Res. 2002; 10: 964-968.
- Hörnell A, Lagström H, Lande B, Thorsdottir I. Protein intake from 0 to 18 years of age and its relation to health: a systematic literature review for the 5th Nordic Nutrition Recommendations. Food Nutr Res. 2013; 23: 57.