Research Article
Austin J Psychiatry Behav Sci. 2014;1(3): 1014.
Empathic Communication in Medical Students’ Interactions with Mental Health Virtual Patient Scenarios: A Descriptive Study Using the Empathic Communication Coding System
Adriana Foster1,2*, Jason Harms1, Brittany Ange2, Brent Rossen3, Benjamin Lok 3, Scott Lind D4, Christie Palladino2
1Department of Psychiatry and Health Behavior, Georgia Regents University, USA
2Education Innovation Institute Georgia Regents University, USA
3Department of Computer and Information Science and Engineering, University of Florida, USA
4Department of Surgery, Drexel University College of Medicine, USA
*Corresponding author: Adriana Foster, Department of Psychiatry and Health Behavior, Medical College of Georgia, Georgia Regents University, 997 St. Sebastian Way, Augusta, GA, 30912, USA
Received: March 31, 2014; Accepted: April 01, 2014; Published: April 03, 2014
Abstract
Empathy is the ability to identify another person’s feelings and to view the world from their perspective. Self-assessed empathy declines throughout medical school and residency training. Technology plays an increasing role in today’s medical education system, which requires delivery of curriculum and assessment of knowledge and skills in standardized manner at geographically distant campuses. Our project assessed whether students communicate empathy in interactions with technology-based teaching tools. We explored student interactions with virtual–patient scenarios and asked the following questions: 1) Do medical students respond empathically to virtual–patients portraying mental healthscenarios?2) If present, does empathy vary with students’ level of training? We analyzed empathy in 155 medical student interactions with depression and bipolar virtual–patients, using the Empathic Communication Coding System. The mean empathic intensity of responses was 1.5 (0–7 scale) for depression and 2.2 for a bipolar scenario. Third–year students responded to the depression virtual–patient with significantly more empathy than 1st (p<0.001) and 2nd–year students (p<0.001).Medical students communicated empathically with virtual patients, but showed less empathy than physicians interacting with live patients. The intensity of the empathic responses increased with the year of training in our sample, which supports the view that empathy can be learned.
Keywords: Empathic Communication; Virtual Patient Scenarios; Descriptive Study Using the Empathic
Abbreviations
ECCS : Empathic Communication Coding System; IRB : Institutional Review Board; GRU : Georgia Regents University; SP : Standardized Patient; VP : Virtual Patient.
Introduction
Empathy represents the ability to identify another person’s feelings and experiences, and to view the world from their perspective. In the physician –patient interaction, empathy improves interpersonal communication and fosters therapeutic alliance [1]. Empathy has been shown to correlate with patient satisfaction and interpersonal trust, to improve medical care outcomes and physician satisfaction [2–4]. Therefore, empathy is an essential communication skill for all physicians.
Some studies demonstrate that self–assessed empathy declines throughout medical school and residency [5–7]. However, other studies, using standardized patient (SP) interactions to measure the behavioral component of empathy, show that while self–measured empathy declines, students display more empathy in clinical encounters, as they progress through medical school [8]. In addition, targeted educational interventions, such as communication skills workshops, can enhance the behavioral dimension of empathy [4]. Yet, it is difficult to retrieve, quantify and provide feedback on student empathic responses and behaviors outside of a clinical skills center environment.
Virtual patient (VP) scenarios are computerized representations of real–life patients and may provide another avenue for evaluating students’ empathic responses. Studies involving hundreds of health professions’ students and practicing clinicians suggest that these virtual clinical scenarios mimic real clinical scenarios, lessen learner anxiety, improve communication skills, and provide tools for standardized, repetitive practice in a safe environment [9–13]. We have previously demonstrated that medical students respond empathically to a life–size VP with abdominal pain [13] but have not investigated such interactions in more portable, web–based VP scenarios. To expand this research, we sought to find out whether medical students express empathy in interactions with web–based VP scenarios focused on depression and bipolar disorder [9,10].
In this study, our research questions were:
1. Do medical students respond empathically to a webbased VP portraying a mental health scenario, like previously demonstrated with a life–size VP with a physical complaint?
2. If found, does medical students’ empathy vary with their level of training?
To answer these questions, we analyzed medical students’ empathic responses in mental health VP scenarios using the Empathic Communication Coding System (ECCS), which assesses how empathy is communicated verbally [14]. We intend to use the results of the analysis to enhance our VP’s capability to elicit empathy and potentially use them as an innovative tooltoteach and assess this fundamental clinical skill in medical school curricula.
Methods
VP scenarios
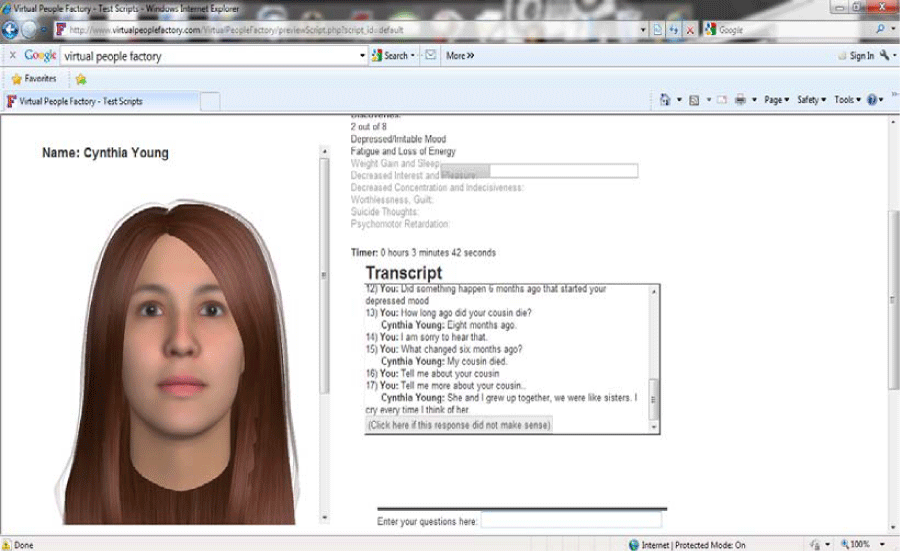
Through a collaborative effort involving medical educators at Georgia Regents University (GRU) and computer scientists at the University of Florida, we have created, evaluated, and integrated VP systems into health professions’ curricula. The two scenarios used for the present study were created in Virtual People Factory [15], a webbrowser interface that permits students to interact with VPs using text–based chat in which a user types an input and receives a textbased response (Figure1).
Students log into the system any wherewith Internet access. They are presented with a brief introduction similar to that encountered before an SP interview, and then are ushered into the chat interface. Once inside the interface, users can engage the virtual patient in a natural–language conversation by typing questions in their own words, to obtain a full medical history. In this study, we analyzed transcripts (i.e. VP–student exchanges) from two Virtual People Factory scenarios (depression and bipolar disorder). The depression VP scenario involves a 21–year–old college student referred to a physician by her campus counselor with complaints of fatigue and anhedonia [9]. The bipolar VP scenario involves a 43–year–old woman with three children who has just moved to the area and comes for her first visit to a psychiatrist, complaining of insomnia [10].
Empathy measurement tool
We coded how empathy is communicated in each of the transcripts using the previously validated ECCS [14,16]. The first part of the ECCS identifies empathic opportunities presented by the patient, divided into three categories:
1. Emotion opportunities are statements where the patient describes herself or himself feeling an emotion at the time, for example joy, fear, hate, sorrow [14] (e.g. statement: “I’ve been thinking a lot of death since my cousin died in a car wreck 8 months ago but I’m scared to kill myself”).
2. Progress opportunities are statements about positive physical or psychosocial developments in patients’ lives (e.g. I’ve cut down (smoking) quite a bit”). No examples of progress opportunities were found in the transcripts analyzed in our study.
3. Challenge opportunities are statements about the negative effect of a physical or psychosocial problem is having on patient’s quality of life (e.g. VP statement: “My clothes don’t fit anymore. It feels like all I do is eat and sleep“).
Figure 1 :Screen-shot of an on–line interaction with the virtual patient (VP) with depression.
The second part of ECCS codes provider responses to these empathic opportunities by one of seven hierarchical levels. In the remainder of the document, we refer to these levels as the “empathic intensity” of the responses.
- Level 6 defines a shared feeling or experience expressed by the clinician in response to a patient–generated opportunity [16] (e.g. Patient: “This back pain makes it difficult for me to work.” Physician: “Sometimes when I am in pain, I have a hard time functioning at work also.”).No such statements were found in our students’ responses to the VP transcripts.
- Level 5 defines the clinician’s confirmation of the patient’s perspective (e.g. VP–statement: “She (my cousin) and I grew up together, we were like sisters. I cry every time I think of her”. Student: “I know it is very hard to lose someone you are close to.”).
- Level 4 defines acknowledgement of the patient’s perspective with further pursuit (e.g.VP–statement: “My cousin died. “Student: “I’m sorry to hear that. When did your cousin die?”).
- Level 3 defines acknowledgement without pursuit (e.g.– statement: “It’s hard to get going. By the time I get up, I figure it’s too late to go to class. “Student: “So you did not go to class”).
- Level 2 defines implicit recognition of the patient’s perspective, which focuses on a peripheral aspect rather than the central issue in the empathic opportunity (e.g. VP–statement: “She (my cousin) and I grew up together, we were like sisters. I cry every time I think of her”. Student: “When did this happen?”).
- Level 1 represents automatic recognition of VP perspective (e.g. Patient: “I was so frustrated. “Physician: “hmmm” [14,16].
- Level 0 represents denial of the patient’s perspective (e.g. VP talks about her cousin who died recently: “She and I grew up together, we were like sisters. I cry every time I think of her”. Student: “How are your grades?”).
Sources of VP interaction transcripts and IRB approval
In this study, we analyzed 155transcripts from student interactions with two VP scenarios (depression and bipolar disorder) which took place in 2008–2010 as part of IRB–approved educational research studies (Table 1), designed to test students’ satisfaction with VP scenarios as educational tools. The 3rd year medical students who volunteered for the study completed the depression VP interaction in a lecture hall equipped with computers, while the 1st and 2nd year medical students who volunteered, used their personal computers to complete the interaction [9,10]. Each of the 155 transcripts was generated by a different student. All repeat transcripts and any transcripts lasting less than 2 minutes were not entered in the analysis. In 2011, we obtained Georgia Regents University IRB approval to analyze empathy in transcripts from these previously IRB–approved research studies of medical students’ interactions with VPs. This study was approved as exempt since the transcripts were de–identified and did not contain any personal health information. We were able to separate students by year of training only for the depression VP scenario, based on the date when they completed the interactions.
Time of the
interaction
N
(Total=155)
Subject description
Type of
interaction
September 2008 -
January 2009
73
3rd year medical students
Depression VP
November 2009
24
2nd year medical students
Depression VP
January 2010
44
2nd year medical students
Depression VP
January 2010
14
3rd& 4th year medical students
Bipolar VP
Table 1: Sources of student-virtual patient (VP) transcripts forempathic communication coding.
Rater Training and Inter–Rater Reliability
Empathy in the VP transcripts was assessed by three raters (2 physicians and a medical student) who trained through a comprehensive review of the ECCS manual and practiced by coding video and movie–clips demonstrating physician–patient interactions. After training, by consensus of all raters, we identified the empathic opportunities presented by the depression and bipolar VPs, using the three empathic response categories defined by the ECCS (emotion, progress and challenge). During this process, we also noted that students responded empathically to the VP’s description of mood symptoms and to the ways those symptoms interfered with daily life. However, patient symptoms do not meet criteria to be rated as empathic opportunities in ECCS. To capture empathic opportunities elicited from the depression and bipolar VP, which do not otherwise fit into an established ECCS category, and to capture and analyze the students’ responses to these opportunities, we created a “symptom” category of empathic opportunity (designated category #4).By doing so, we intended to increase the generalizability of the coding system to medical students’ interactions with patients with mental health complaints. This category included such statements as, “I feel worthless”, “I am nervous all the time”, “I’ve been irritable at everyone and everything “or “I just don’t care about anything, anymore. Everything makes me cry”. Expanding our coding system to include four categories of empathic opportunity reflects findings in the literature that addressing such broader opportunities may impact patient care. For example, Levinson [17], described a broader range of patients’ comments about emotional or social “clues” than those included in Bylund’s [14] empathic opportunity categories and demonstrated that encounters in which physicians missed these clues lasted longer than those where the clues were responded to.
Following training, each rater independently coded medical students ‘responses to VP empathic opportunities in a randomly selected sample of 10% of the transcripts. To assess agreement between the 3 raters, we calculated the intra–class correlation coefficient (ICC) using SAS 9.3, Cary, NC. The ICC was 0.725 for the empathic responses in depression VP transcripts and 0.642 for the responses in the bipolar VP, which represents substantial interrater agreement [18]. The raters met as a group to discuss coding, and discrepancies were resolved by group consensus. Each of the raters then independently coded the students’ empathic responses in a portion of the remaining transcripts.
Statistical analyses
All statistical analyses were performed using SAS 9.3. We performed descriptive statistics to report the mean number and category of empathic opportunities by scenario, and the mean level of empathic intensity of student responses for each scenario. Although the nature of the data was ordinal, we performed Independent t–testsand One–Way ANOVAs to compare the mean empathic intensity of the student responses. Conover and Iman [19] showed that these tests are equivalent to the Mann–Whitney–Wilcox on rank sum tests and Kruskal–Wallis tests on ordinal data, respectively, which we also verified with our data.
Results
Empathic opportunities and the type and intensity of students' empathic responses
We analyzed 141 depression VP transcripts and 14 bipolar VP transcripts, with an average of 10.58 and 11.71 empathic opportunities per transcript, respectively. The students’ responses by level of empathic intensity are shown in Table 2.
DEPRESSION VP
Total student responses to empathic opportunities from
141 VP transcripts= 1439
BIPOLAR VP
Total student responses to empathic opportunities from
14 VP transcripts= 163
Empathic intensity of students' responses
Number(percentage)
Number (percentage)
Level 0Denial of patient's perspective
683 (47.46)
51 (31.29)
Level 1Automatic recognition
3 (0.21)
0 (0.0)
Level 2 Implicit recognition
403 (28.01)
44(26.99)
Level 3 Acknowledgement without pursuit
67 (4.66)
2 (1.23)
Level 4Acknowledgement with pursuit
262 (18.21)
65 (39.88)
Level 5 Confirmation
21 (1.46)
1 (0.61)
Table 2: Empathic intensity of student responses in virtual patient (VP) interactions.
Students demonstrated denial (level 0) in 47.46%of responses in the depression scenario and 31.29% responses in the bipolar scenario. Approximately one–quarter of student responses in the depression scenario and over 40% of student responses in the bipolar scenario were rated at a level of 3 or higher (acknowledgement with and without pursuit or confirmation). No student responses fit empathic intensity level–6 (shared feeling or experience). The mean empathic intensity of response for the depression and bipolar scenarios was 1.5 (SD=1.6) and 2.2 (SD=1.7) respectively.
Empathic intensity of students' responses by year of training
A One–Way ANOVA results showed that the intensity of students’ responses by year of training were statistically different (F (2, 1436) =17.906, P<.001). We applied a Bonferroni adjustment (α=0.05⁄3=0.017) and found that3rdyear medical students’ empathy in response to the empathic opportunities, was significantly higher when compared to that of 1st (p<.001) and respectively 2ndyear (p<.001) students’ responses in the depression scenario. There was no significant difference between the intensity of the 1st and 2ndyear students’ responses (Table 3).
DEPRESSION
VP scenario
BIPOLAR
VP scenario
Overall mean (SD) empathic intensity of student responses*
1.50 (1.60)
2.20 (1.70)
Mean (SD) empathic intensity of 1st year student responses*
1.21 (1.40)
–
Mean (SD) empathic intensity of 2nd year student responses*
1.31 (1.44)↑
–
Mean (SD) empathic intensity of 3rd year student responses*
1.74 (1.72) ‡ §
–
Table 3: The empathic intensity of students' responses in interactions with the depression and bipolar virtual patient (VP) scenarios.
Empathic intensity of students' responses by category of empathic opportunity
There was a statistically significant difference found in the mean empathic intensity of the student responses for the different categories of empathic opportunities (categories 1=emotion, 3=challenge, and 4=symptom), using a One–Way ANOVA test (F (2, 1428) =21.72, P<.0001). We applied a Bonferroni adjustment (α=0.05⁄3=0.017) and found that for the depression VP scenario, the intensity of the empathic responses to category 1 (emotion) opportunities was significantly higher than the intensity of students’ responses to category 3 (challenge) or 4 (symptom) (Table 4). There were no category 2 (progress) VP empathic opportunities in the depression scenario. In the bipolar scenario, there were no category 1 (emotion) or 2 (progress) opportunities. Category 3 (challenge) VP empathic opportunities generated a significantly higher intensity of students ‘empathic responses than category 4 (symptom) in the bipolar VP transcripts (T (161) =2.32, P=0.02) (Table 4).
EMPATHIC OPPORTUNITY TYPE
MEAN (SD) EMPATHIC INTENSITY OF STUDENT RESPONSES*
DEPRESSION
VP scenario
BIPOLAR
VP scenario
EMOTION� (category 1)
Example "She (my cousin) and I grew up together, we were like sisters. I cry every time I think of her".
2.19� (1.73)†‡
none found
CHALLENGE (category 3)
Example:
"It's hard to get going. By the time I get up, it's too late to go to class".
1.39� (1.54)†
2.57� (1.55)
SYMPTOM (category 4)
Example: "I just don't care about anything, anymore. Everything makes me cry."
1.41� (1.56)
1.95� (1.76)§
Table 4: Empathic intensity of student responses by category of empathic opportunity offered by the virtual patient (VP).
Discussion
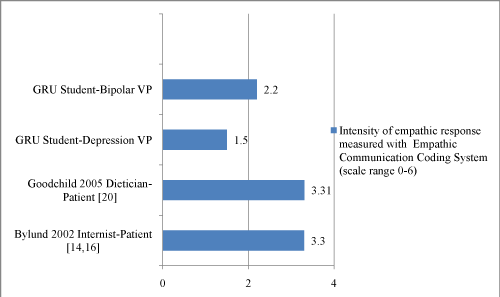
This study expands our previously reported research by demonstrating that medical students can demonstrate empathy in interviews with web–based VPs. Almost half of the student responses in the bipolar transcripts were coded at an empathic intensity of 3–5. However, the bipolar (mean empathic intensity of responses=2.2) and depression VP (mean empathic intensity=1.5) scenarios in our study generated much less empathy than real–life encounters of clinicians and patients [14,20] (Figure 2). In fact, almost half of student responses in our depression scenario represented denial of the patient’s perspective.
Figure 2: Comparison of empathic intensity in virtual patient (VP) and live patient interaction studies using the empathic communication coding system (ECCS).
There are several possible reasons for differences between students’ responses toour VP scenarios and physicians’ responses to real patients. The neural pathways implicated in understanding others’ actions and the intentions behind them (“the mirror neuron system”) and in communicating empathy through spoken versus written words may explain the differences in the empathic intensity of students’ responses to the VPF versus the real life patient encounters [21–23]. As our results seem to suggest, it is also possible that physicians’ empathic communication continues to improve throughout training and clinical practice, and thus practicing clinicians are more skilled at communicating empathy than medical students. Also, the lack of progress opportunities and the limited emotion–type opportunities in our scenarios may have not reflected the breadth of empathic opportunities present in real–life scenarios.
The social stigma associated with mental illness could also account for our findings. Pescosolido [24] showed that the stigma towards people with major depression did not decrease significantly from 1996 to 2006 and it is possible that the level of empathy expressed by medical students in the depression and bipolar scenarios reflects this stigma [25].
In this study, students’ communication of empathy improved as they progressed through medical school, confirming the results reported by Chen [8]. This finding suggests that empathy can be learned, and that learning may perhaps be reflected by VP assessment of empathic communication.
In this study, the students responded with higher empathic intensity to opportunities reflecting emotion than those reflecting challenge or psychiatric symptoms in the depression VP scenario. Bylund and Makoul [14] did not find a correlation between the intensity of empathic responses and the type of empathic opportunities in encounters between internists and adult patients. Possibly VPs are better suited than real patients to explore the correlation between the type of empathic opportunities and the empathic responses they generate, because they allow building all types of empathic opportunities into the scenarios.
Our study findings point to several potential areas for VP enhancement. Progress–type opportunities were not found in any of our scenarios and we will address this limitation by introducing them in future VP scenarios. Building progress and enhancing emotion empathic opportunities in the mental–health VP scenarios may also help elicit empathy similar to a real patient encounter.
Conclusions
This study builds upon previous work and not only shows that medical students can respond empathically to VPs but offers a glimpse into the quantity and quality of medical students’ empathic communication in these interactions. The fact that the intensity empathic responses to VP scenarios increases with the year of training supports the view that empathic communication can be learned. The VP scenarios may represent an innovative educational tool to assess, and possibly even to teach this essential communication skill. Further research should address the progression of empathy in controlled studies involving VP interventions that teach empathic communication throughout medical school, residency training and independent medical practice. Finally, given the low mean empathic intensity of student responses towards the VPs with psychiatric complaints, we need to further explore whether teaching empathic communication is as effective in mental health, an area open to stigma, as it appears to be in general medical interactions. However, mental health VP scenarios enhanced with progress and emotion statements may yield a different empathic response from students.
Acknowledgment
The first author’s time to complete this study was supported by an educational research fellowship from the GRU Education Innovation Institute.
References
- Charon R. The patient-physician relationship. Narrative medicine: a model for empathy, reflection, profession, and trust. JAMA. 2001; 286: 1897-1902.
- Hojat M, Louis DZ, Maxwell K, Markham F, Wender R, Joseph S Gonnella. Patient perceptions of physician empathy, satisfaction with physician, interpersonal trust and compliance, Int J Med Educ. 2010; 1: 83-87.
- Hojat M, Gonnella JS, Nasca TJ, Mangione S, Vergare M, Magee M. Physician empathy: definition, components, measurement, and relationship to gender and specialty. Am J Psychiatry. 2002; 159: 1563-1569.
- Stepien KA, Baernstein A. Educating for empathy. A review. J Gen Intern Med. 2006; 21: 524-530.
- Hojat M, Mangione S, Nasca TJ, Rattner S, Erdmann JB, Gonnella JS, et al. An empirical study of decline in empathy in medical school. Med Educ. 2004; 38: 934-941.
- Hojat M, Vergare MJ, Maxwell K, Brainard G, Herrine SK, Isenberg GA, et al. The devil is in the third year: a longitudinal study of erosion of empathy in medical school. Acad Med. 2009; 84: 1182-1191.
- Neumann M, Edelhäuser F, Tauschel D, Fischer MR, Wirtz M, Woopen C, et al. Empathy decline and its reasons: a systematic review of studies with medical students and residents. Acad Med. 2011; 86: 996-1009.
- Chen DC, Pahilan ME, Orlander JD. Comparing a self-administered measure of empathy with observed behavior among medical students. J Gen Intern Med. 2010; 25: 200-202.
- Shah H, Rossen B, Lok B, Londino D, Lind SD, Foster A. Interactive virtual-patient scenarios: an evolving tool in psychiatric education. Acad Psychiatry. 2012; 36: 146-150.
- Foster A, Noseworthy D, Shah H, Lind DS, Lok B. Evaluation of Medical Student Interaction with a Bipolar Virtual Patient Scenario Written by a Peer Support Specialist a Pilot Study. In Briscoe G, Spollen J. Proceedings of the 2010 Annual Meeting of the Association of Directors of Medical Student Education in Psychiatry (ADMSEP). Teaching & Learning in Medicine. 2011; 23: 96-102.
- Johnsen K, Raij A, Stevens A, Lind DS, Lok B. The Validity of a Virtual Human Experience for Interpersonal Skills Education, SIGCHI Conference of Human Factors in Computing Systems Proceedings. San Jose. 2007; 1049-1058.
- Stevens A, Hernandez J, Johnsen K, Dickerson R, Raij A, Harrison C, et al. The use of virtual patients to teach medical students history taking and communication skills. Am J Surg. 2006; 191: 806-811.
- Deladisma AM, Cohen M, Stevens A, Wagner P, Lok B, Bernard T, et al. Do medical students respond empathetically to a virtual patient? Am J Surg. 2007; 193: 756-760.
- Bylund CL, Makoul G. Empathic communication and gender in the physician-patient encounter. Patient Educ Couns. 2002; 48: 207-216.
- Rossen B, Lind DS, Lok B, "Human-centered Distributed Conversational Modeling: Efficient Modeling of Robust Virtual Human Conversations" 9th International Conference on Intelligent Virtual Agents Amsterdam, Netherlands. 2009; 5773: 474-481.
- Bylund CL, Makoul G. Examining empathy in medical encounters: an observational study using the empathic communication coding system. Health Commun. 2005; 18: 123-140.
- Levinson W, Gorawara-Bhat R, Lamb J. A study of patient clues and physician responses in primary care and surgical settings. JAMA. 2000; 284: 1021-1027.
- Landis JR, Koch GG. The measurement of observer agreement for categorical data. Biometrics. 1977; 33: 159-174.
- Conover WJ, Iman RL. Rank Transformations as a Bridge between Parametric and Non-parametric statistics, The American Statistician. 1981; 35: 124-129.
- Goodchild CE, Skinner TC, Parkin T. The value of empathy in dietetic consultations. A pilot study to investigate its effect on satisfaction, autonomy and agreement. J Hum Nutr Diet. 2005; 18: 181-185.
- Cattaneo L, Rizzolatti G. The mirror neuron system. Arch Neurol. 2009; 66: 557-560.
- Decety J, Jackson PL. The functional architecture of human empathy. Behav Cogn Neurosci Rev. 2004; 3: 71-100.
- Neumann M, Bensing J, Mercer S, Ernstmann N, Ommen O, Pfaff H. Analyzing the "nature" and "specific effectiveness" of clinical empathy: a theoretical overview and contribution towards a theory-based research agenda. Patient Educ Couns. 2009; 74: 339-346.
- Pescosolido BA, Martin JK, Long JS, Medina TR, Phelan JC, Link BG. "A disease like any other"? A decade of change in public reactions to schizophrenia, depression, and alcohol dependence. Am J Psychiatry. 2010; 167: 1321-1330.
- Schwenk TL, Davis L, Wimsatt LA. Depression, stigma, and suicidal ideation in medical students. JAMA. 2010; 304: 1181-1190.