Research Article
Austin J Psychiatry Behav Sci. 2014;1(4): 1019.
Evaluation of Antiepileptic for Behavioral Symptoms in Severe Intellectual Disabilities
Ken Taniguchi1, 2, Kouzin Kamino1, 2,*, Takashi Kudo2 and Masatoshi Takeda2
1National Hospital Organization, Yamato Mental-Medical Center, Japan
2Department of Psychiatry, Osaka University Graduate School of Medicine, Japan
*Corresponding author: Kouzin Kamino, National Hospital Organization, Yamato Mental-Medical Center, 2815 Koizumi, Yamatokoriyama, Nara 639-1042, Japan
Received: May 08, 2014; Accepted: May 20, 2014; Published: May 21, 2014
Abstract
Antiepileptic, known to manage mood disorders, has been prescribed for behavioral symptoms in severe intellectual disabilities, but often results in multiple prescriptions.
Objective: To classify the behavioral symptoms and evaluate the prescription of antiepileptic for the extent of the behavioral symptoms.
Method: The extent of the behavioral symptoms was scored using Severe Behavior Disorder Assessment Scale, composed of the 11–items and 4–frequency scale, in 80 hospitalized subjects with severe intellectual disabilities, and analyzed in relation to the number and dose of prescribed antiepileptic. Phenytoin was prescribed for 4 subjects, and their scores were evaluated at baseline and after the prescription.
Results: The subjects with organic brain disease or epilepsy showed lower frequency of the behavioral symptoms compared to those without. Factor analysis indicated that the behavioral symptoms were classified into 3 factors; representatively, obsessive⁄hyperactive, aggressive and self–injurious behavior. The extent of the symptoms was inversely correlated to the number of antiepileptic, including valproic acid, carbamazepine and phenytoin. While valproic acid was significantly inversely correlated with the symptoms of obsessive⁄hyperactive and self–injurious behavior, phenytoin was possibly effective for the aggressive behavior. When phenytoin was prescribed in 4 subjects, the score of aggressive behavior was significantly decreased after the prescription of phenytoin, but paroxysmal tonic upgaze was often observed.
Conclusion: Valproic acid was effective for the behavioral symptoms, similarly to mood disorders, and phenytoin could stabilize the aggressive behavior. Therefore, among antiepileptic, valproic acid could be the first choice to the symptoms, and prescriptions of antiepileptic could be symptomatically selected.
Keywords: Intellectual disabilities, Behavioral symptom, Antiepileptic, Valproic acid, Carbamazepine, Phenytoin
Introduction
Aggressive, self–injurious, and the other aberrant behaviors are troublesome in nursing and care for subjects with severe intellectual disabilities [1]. Because of resulting in self–injury and injury to their caregivers, the subjects are extremely difficult to stay at home, and necessary to intensive care in nursing home or hospital. The behavioral symptoms of the subjects, frequently and intensively acting these behaviors in the unusual manner, are symptomatically categorized as an entity called severe behavior disorder, and also synonymously “disruptive behavior disorder”, “destructive behavior”, “challenging behavior”, “aggression”, etc. Severe Behavior Disorder Assessment Scale; SBDAS has been utilized to evaluate the behavioral symptoms in Japan [2]. The total scores of the scale more than 10 were observed in 50% of inpatients admitted in national facilities for those with severe intellectual disabilities, and behavioral symptoms were more evident in those without disabled motor activity [3].
The symptoms are thought to be complicatedly caused by genetic, brain organic, physical and circumstantial factors. Winter showed that there were significant and independent associations of challenging behavior with urinary incontinence, pain related to cerebral palsy, chronic sleep problems, and visual impairment, but not with hearing impairment, bowel incontinence, mobility impairment or epilepsy [4]. Cooper reported a cohort study to examine factors affecting aggressive behavior and self–injury in those with intellectual disabilities; aggressive behavior is correlated to lower intelligence, female, not living with family care–giver, no Down syndrome, attention–deficit hyperactivity disorders (AD⁄HD), and urinary incontinence, and that self–injury is the most strongly correlated to lower intelligence and AD⁄HD, and also correlated to no Down syndrome, not living with family care–giver and urinary incontinence [1,5]. Psychological management of the behavioral symptoms is principally the most important, but often results in care–givers exhausted. A number of studies have been undertaken with psychotropic such as antipsychotics, antiepileptic, lithium and anti depressant, and reviewed that risperidone is well demonstrated to be effective for the behavioral symptoms [6]. Because of unwilling adverse effects, such as dizziness, fall, apathy, weight gain, the dose of antipsychotics is limited, resulting in insufficient management of the behavioral symptoms, especially aggressive behavior. The selection of prescription remains in practical experiences, and often results in multiple prescriptions.
To examine psychiatric characters of the severe behavior disorder, we evaluated and analyzed the behavioral symptoms of institutionalized subjects. To evaluate the effectiveness of antiepileptic, we also analyzed the relation between the extent of the behavioral symptoms and the number and dose of prescribed antiepileptic.
Subjects and Methods
Subjects
Subjects with severe intellectual disabilities were 80 inpatients in National Hospital Organization, Yamato Mental–Medical Center, composed of 59 males and 21 females, with their mean ± SD age of 37.6 ± 8.8 years. The causes underlying in intellectual disability were identified in 12 cases; tuberous sclerosis (2 cases), carbohydratedeficient syndrome (2 cases), head trauma (2 cases), encephalitis (3 cases), microcephaly (1 case), fragile X syndrome (1 case) and Down syndrome (1 case), but unknown in the other 68 cases. Information of this study was given to the subjects, when possible, and their guardians, and the informed consent to participate in this study was obtained from each guardian. The study was approved by the Ethics Committee of Yamato Mental–Medical Center.
Definition of severe behavior disorder
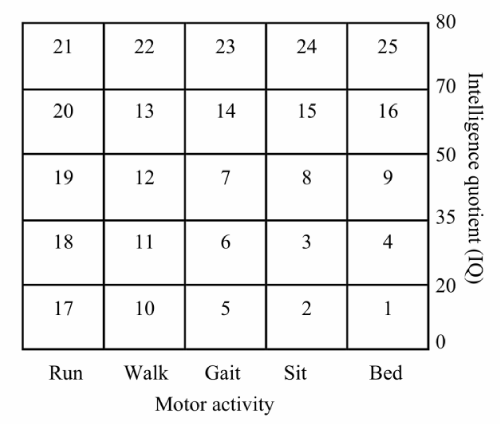
Clinical information of the subjects was obtained from their case records, and intelligence quotient (IQ) had been evaluated by clinical psychologists using Tanaka–Binet Intelligence Scale [7] or the Enjoji developmental test that evaluates physical abilities of the whole body, skilled hand motor activities, behavior, interpersonal skills, speech ability, and language comprehension [8]. Motor and intellectual disability of each subject was evaluated for their IQ and motor activity, and classified in Oshima's classification (Figure 1) [9]. Severe behavior disorder with intellectual disabilities corresponds to type 5, 6, 10, 11, 17 and 18 in the classification, where IQ level is ranged from 0 to 35, and motor activity is normal or mildly disabled (Table 1). The total score of Severe Behavior Disorder Assessment Scale; SBDAS, abbreviated hereafter, has been shown to be correlated with all five sub–scores on the Japanese version of the Aberrant Behavior Checklist–Community (ABC–J), namely, (I) Irritability, Agitation, Crying; (II) Lethargy, Social Withdrawal; (III) Stereotypic Behavior; (IV) Hyperactivity, Noncompliance; and (V) Inappropriate Speech[10,11].
Figure 1 :The score matrix of Oshima's classification of intelligence quotient (IQ) and motor activity. Run: able to run, Walk: able to walk, Gait: gait disturbance, Sit: able to sit, bed: bedridden.
Classification
type
Motor activity
Intelligence
quotient (IQ)
Total
in subjects
Percent
Type2
Able to sit
0 - 20
1
1.25
Type3
Able to sit
21 - 35
0
0
Type5
Gait disturbance
0 - 20
7
8.75
Type6
Gait disturbance
21 - 35
0
0
Type10
Able to walk
0 - 20
25
31.25
Type11
Able to walk
21 - 35
0
0
Type17
Able to run
0 - 20
44
55
Type18
Able to run
21 - 35
3
3.75
Table 1: Type of Oshima's classification of subjects.
Severe behavior disorder assessment scale (SBDAS)
The information's of behavioral symptoms are obtained by interview of their care–giver, nurse, nurse teacher and medical doctor, and scored using SBDAS [2]. This instrument is composed of 11 items; self–injury, physical harm, obsessive⁄repetitive behavior, destruction of property, sleep problems, eating problems, toilet problems, hyperactivity, screaming, sudden agitation, and explosive violent behavior. Each itemed behavior is scored into 0 to 5 points, in accord with its frequency, where the higher point indicates the more frequent behavior (Supplement 1). The total score of SBDAS can be ranged from 0 to 55 points, and the score more than 10 points is classified as severe behavior disorder, based on the criteria defined by Ministry of Health, Labour and Welfare of Japan [2].
Item
Examples of behaviors
Score 1
Score 3
Score 5
1 Self-injury
Harm itself by hitting to cut flesh or deform head, nail-peeling, etc.
1 - 2 / week
1 - 2 / day
all day long
2 Physical harm
Harm the others by biting, kicking, hitting, hair-pulling, head-butting, etc.
1 - 2 / month
1 - 2 / week
many times / day
3 Obsessive/repetitive behavior
Impossible to control the action; for example, against strong direction, take off clothes, reject to go outside, fuss over a tiny matter strongly such as coming back from long distances to pick up something, etc.
1 - 2 / week
1 - 2 / day
many times / day
4 Destruction
Break glass, furniture, door, tableware, chair, glasses, resulting in inflicting injury itself as well as the others, including tearing clothes, etc.
1 - 2 / month
1 - 2 / week
many times / day
5 Sleep problems
Days and nights being reversed, do not stay in bed and break objects or inflict troublesome on the others
1 - 2 / month
1 - 2 / week
almost every day
6 Eating problems
Cannot eat with the others, and turn over table, throw dishes, not sit down and walk around, etc. Eat feces, nail, stone, etc. Reject to eat food. Take unbalanced diet resulting in unhealthy condition.
1 - 2 / week
almost every day
almost every meal
7 Toilet problems
Play with and throw feces, slather wall with feces, repeat urination and evacuation obsessively.
1 - 2 / month
1 - 2 / week
almost every day
8 Hyperactivity
Run out incautiously and dangerously. Run around continually when not observed. Climb up a high space dangerously, for example, balcony, etc.
1 - 2 / month
1 - 2 / week
almost every day
9 Screaming
Shout intolerably. Once cry, continue to cry for several hours.
almost every day
all day long
continually
10 Sudden agitation
Once agitate, caregivers cannot calm it and cannot take care.
-
-
observed
11 Explosive violent behavior
When directed slightly, act explosively and make caregivers be afraid of it.
-
-
observed
Supplement 1: Severe behavior disorder assessment scale: SBDAS.
Epilepsy, neuroimaging, dosage of antiepileptic
Epilepsy was diagnosed by past history and EEG of all subjects, and neuroimaging study was done by brain CT or MRI. All subjects were divided into two groups by the history of epileptic attack within two years or not, and also by the existence of abnormal finding in brain neuroimaging studies. Dosage of prescribed antiepileptic was counted in each subject.
Administration of phenytoin
Four subjects were prescribed 100 mg per day of phenytoin for one week, followed by 200mg per day for 3 weeks. At baseline and after 4 weeks of the prescription, the behavioral symptoms were evaluated by care–givers using SBDAS and ABC–J scores [11].
Statistical analysis
The differences of the score of SBDAS were tested by Mann– Whitney U test, for groups divided by the history of epileptic attack, and by the existence of neuroimaging abnormality. Factor analysis was conducted against the score of 11 items of SBDAS, using principal component analysis. Correlation of the dosage of antiepileptic with the total score was tested by Spearman's rank correlation, where minimum correlation efficient detectable at power 0.8 were 0.4 for valproic acid (n=48), 0.45 for carbamazepine (n=39), and 0.6 for phenytoin (n=19). The relation of dosage of antiepileptic to the score of each factor obtained was also tested by Spearman's rank correlation. In phenytoin administration study, the scores at baseline and after 4 weeks are compared by paired t–test. P values less than 0.05 were considered significant.
Results
Factor analysis of severe behavior disorder
The subjects in this study showed mean ± SD of the total score of SBDAS at 16 ± 10.8. Among 80 subjects, at least one problem behavior was found in 73 subjects (91%), and 55 subjects (69%) were categorized as severe behavior disorder. The frequency of each behavior was ranked by obsessive⁄repetitive behavior (71.3%), hyperactivity (53.8%), self–injury (51.3%), physical harm (48.8%), eating problem (47.5%), toilet problem (40.0%), destruction (25.0%), sudden agitation (23.8%), sleep problem (22.5%), screaming (17.5%) and explosive violent behavior (10.0%). Factor analysis of each item yielded a 3–factor solution (Table 2). Factor I included obsessive⁄repetitive behavior, representatively, and also destruction of property, sleep problems, eating problem, toilet problems and hyperactivity. Factor II included physical harm, sudden agitation and explosive violent behavior. Factor III did self–injury, physical harm and screaming.
Item
Factor I
Factor II
Factor III
1 Self-injury
0.24
-0.18
0.68*
2 Physical harm
0.05
0.52*
0.62*
3 Obsessive/repetitive behavior
0.54*
0.12
-0.01
4 Destruction
0.56*
0.19
0.20
5 Sleep problems
0.79*
-0.03
0.03
6 Eating problems
0.71*
-0.04
-0.04
7 Toilet problems
0.65*
-0.21
0.12
8 Hyperactivity
0.87*
0.08
-0.14
9 Screaming
-0.04
-0.03
0.78*
10 Sudden agitation
0.06
0.85*
-0.10
11 Explosive violent behavior
0.05
0.82*
0.01
Eigenvalue
3.52
1.72
1.20
(*Factor loadings > 0.5)
Table 2: Items and factor loadings for SBDAS.
Neuroimaging and epilepsy
The group with abnormal neuroimaging findings (40 cases) showed lower total score compared to the group without (20 cases), significantly in the sub–score of self–injury and destruction of property and sudden agitation (Table 3). The group with epileptic attack within two years (22 cases) indicated lower total score compared to the group without (58 cases), significantly in the sub–score of selfinjury, eating problems, toilet problems and hyperactivity (Table 4). Therefore, the subjects with organic brain disease, as a whole, showed lower frequency of behavioral symptoms.
Abnormality in neuroimaging
Wilcoxon
rank sum test(+)
(-)
Number in total
40
20
Item
Mean (SD)
Mean (SD)
p value
1 Self-injury
1.10 (1.85)
2.30 (1.69)
0.004
2 Physical harm
1.28 (1.91)
2.15 (2.23)
0.140
3 Obsessive/repetitive behavior
2.88 (2.27)
3.80 (2.04)
0.123
4 Destruction
0.63 (1.50)
1.70 (2.18)
0.024
5 Sleep problems
0.70 (1.49)
0.60 (1.44)
0.964
6 Eating problems
1.98 (2.35)
2.75 (2.55)
0.319
7 Toilet problems
1.45 (2.09)
2.15 (2.32)
0.164
8 Hyperactivity
2.20 (2.48)
3.45 (2.26)
0.055
9 Screaming
0.33 (1.12)
0.50 (0.95)
0.122
10 Sudden agitation
0.63 (1.67)
1.75 (2.45)
0.043
11 Explosive violent behavior
0.38 (1.33)
0.50 (1.54)
0.756
Total score
13.43 (10.03)
21.75 (10.94)
0.003
Table 3: The score of SBDAS in the groups divided by abnormality in neuroimaging.
Epilepsy
Wilcoxon
rank sum test(+)
(-)
Number in total
22
58
Mean (SD)
Mean (SD)
p value
1 Self-injury
0.73(1.16)
1.74(1.92)
0.037
2 Physical harm
1.55(2.18)
1.74(1.98)
0.450
3 Obsessive/repetitive behavior
2.82(2.38)
3.36(2.17)
0.391
4 Destruction
0.73(1.64)
1.07(1.88)
0.346
5 Sleep problems
0.64(1.56)
0.72(1.45)
0.637
6 Eating problems
1.18(2.13)
2.48(2.41)
0.032
7 Toilet problems
0.59(1.56)
2.02(2.22)
0.005
8 Hyperactivity
1.36(2.28)
2.95(2.36)
0.010
9 Screaming
0.18(0.66)
0.41(1.08)
0.237
10 Sudden agitation
0.91(1.97)
1.29(2.20)
0.478
11 Explosive violent behavior
0.23(1.07)
0.60(1.64)
0.325
Total score
10.91(10.61)
18.40(10.28)
0.007
Table 4: The score of SBDAS in the subjects divided by the history of epilepsy.
Prescription and dosage of antiepileptic
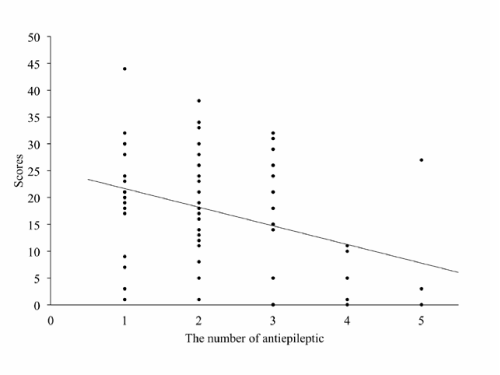
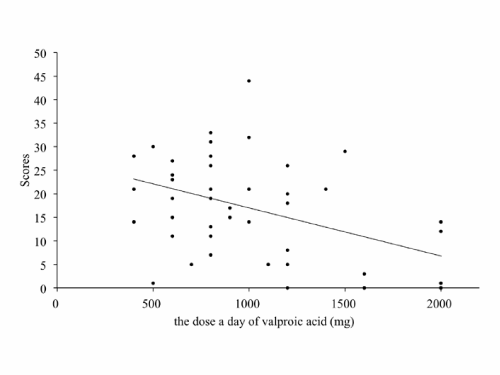
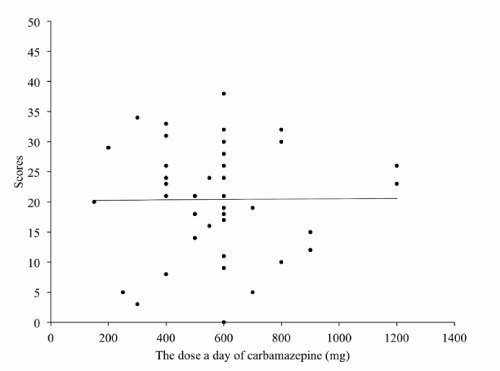
Antiepileptic was prescribed in 67 cases, among those 34 cases had epileptic episode within 2 years. The numbers of prescribed antiepileptic were 0 (13 cases), 1 (21 cases), 2 (23 cases), 3 (14 cases), 4 (6 cases) and 5 (3 case). Among those prescribed antiepileptic, the total score of SBDAS was inversely correlated to the number of antiepileptic (Spearman's rank correlation, rs = – 0.32, p = 0.007; Figure 2). The total score of SBDAS was inversely correlated to dosage of valproic acid, but not to carbamazepine and phenytoin (Figure 3–5). Dosage of valproic acid inversely correlated significantly to 2 sub–scales, representatively, self–injury and hyperactivity (Table 5). Dosage of phenytoin suggested a trend to inversely relate to toilet problems and sudden agitation, while carbamazepine showed no change of the total score in any dosages. When analyzed by Factors obtained by the factor analysis, dosage of valproic acid showed an inverse correlation to Factor III, and did a trend inversely to correlate to Factor I (Table 6).
Figure 2: Scatter plot of the scores on SBDAS in the groups classified according to the number of prescribed antiepileptic. Line indicates a liner regression curve.
Figure 3: The relation between dosage of valproic acid and the total score of SBDAS. Line indicates a liner regression curve.
Figure 4: The relation between dosage of carbamazepine and the total score of SBDAS. Line indicates a liner regression curve.
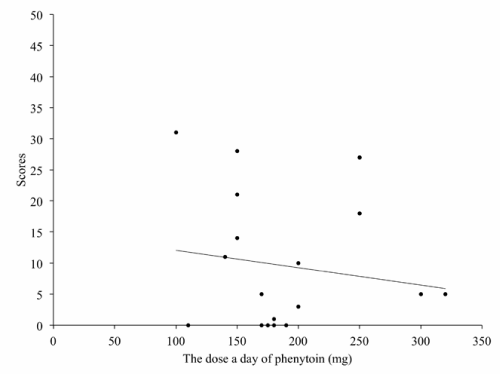
Figure 5: The relation between dosage of phenytoin and the total score of SBDAS. Line indicates a liner regression curve.
Valproic acid(n=48)
Carbamazepine(n=39)
Phenytoin(n=19)
Item
rs
p
rs
p
rs
p
1 Self-injury
-0.56
<.0001
-0.12
0.451
-0.26
0.285
2 Physical harm
-0.18
0.232
-0.08
0.638
-0.01
0.965
3 Obsessive/repetitive behavior
-0.19
0.202
0.25
0.132
-0.20
0.413
4 Destruction
-0.07
0.620
-0.22
0.178
0.04
0.872
5 Sleep problems
-0.05
0.750
-0.21
0.202
0.28
0.244
6 Eating problems
-0.25
0.089
0.21
0.199
0.06
0.800
7 Toilet problems
-0.13
0.396
0.16
0.336
-0.44
0.059
8 Hyperactivity
-0.37
0.009
-0.05
0.745
-0.30
0.218
9 Screaming
-0.16
0.268
0.02
0.896
-0.22
0.374
10 Sudden agitation
-0.06
0.662
-0.07
0.688
-0.45
0.053
11 Explosive violent behavior
-0.01
0.960
0.07
0.659
NA
NA
12 Total score
-0.39
0.006
-0.05
0.762
-0.12
0.637
rs, Spearman's correlation; NA, not available
Table 5: Spearman's correlation between the dosage of antiepileptic and the score of SBDAS.
Valproic acid(n=48)
Carbamazepine(n=39)
Phenytoin(n=19)
rs
p
rs
p
rs
p
Factor I
-0.28
0.051
-0.01
0.944
0.04
0.858
Factor II
-0.15
0.325
0.04
0.802
-0.23
0.344
Factor III
-0.45
0.001
-0.11
0.499
-0.19
0.447
rs: Spearman's correlation
Factor I: obsessive/repetitive behavior, destruction, sleep problems, eating problem, toilet problems, and hyperactivity
Factor II: physical harm, sudden agitation and explosive violent behavior
Factor III: self-injury, physical harm and screaming
Table 6: Spearman's correlation of the factors of the score of SBDAS with the dosage of antiepileptic.
Evaluation of phenytoin administration
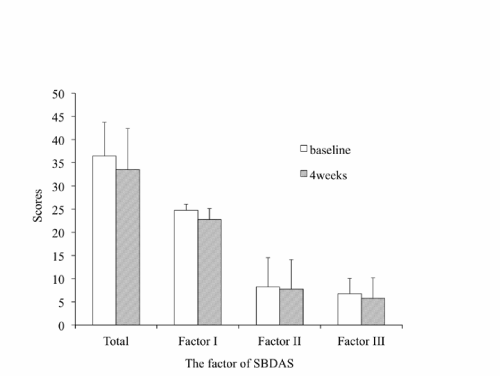
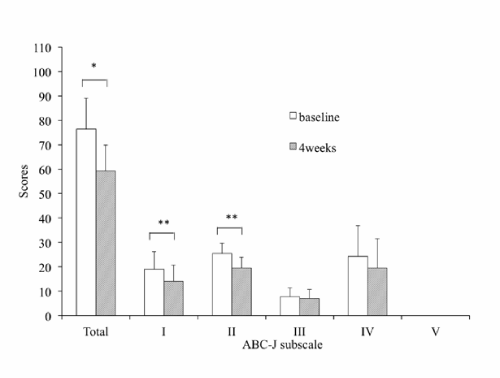
To examine the effectiveness of phenytoin, we performed a phenytoin administration study. The score of SBDAS showed a trend to decrease by the administration of phenytoin, but not significantly (Figure 6). We also evaluated ABC–J score in 4 subjects at baseline and after 4–week administration of phenytoin. The total score after the administration was significantly decreased, and the scores of the subscale of (I) Irritability, Agitation, Crying and (II) Lethargy, Social Withdrawal were significantly lowered after the administration compared to the baseline (Figure 7). However, paroxysmal tonic upgaze was observed in 2 out of 4 subjects.
Figure 6: Comparison of the scores of SBDAS at baseline and after the prescription of phenytoin for 4 weeks (n=4). SBDAS subscales are Factor I: obsessive/hyperactive; Factor II: aggressive; and Factor III: self-injurious behavior, representatively.
Figure 7: Comparison of the scores of ABC-J at baseline and after the prescription of phenytoin for 4 weeks (n=4). ABC-J subscales are (I) Irritability, Agitation, Crying; (II) Lethargy, Social Withdrawal; (III) Stereotypic Behavior; (IV) Hyperactivity, Noncompliance; and (V) Inappropriate Speech. Bars indicate the standard deviation. *p<0.05, **p<0.01 (paired t-test).
Discussion
Severe behavior disorder
The prevalence of aggressive behavior with intellectual disabilities varied across studies. High frequency of behavioral symptoms in this study (91%) is caused by the selection bias of the subjects, because those were institutionalized in the wards of severe intellectual disabilities. Crocker reported that among 3165 adult with intellectual disability, aggressive behavior was found in 51.8% during 12 months, and the most frequent symptom was verbal aggression (37.6%) [12]. Poppes showed that the prevalence of self–injury and stereotypical behavior in people with profound intellectual disability was 82%, and aggressive⁄destructive behavior was 45% [13]. Cooper reported that the point prevalence of aggressive behavior and self–injurious behavior was 9.8% and 4.9%, respectively, among the adult population of intellectual disabilities in community–based setting in UK [1,5].
Factor analysis of the symptoms indicated that 11 classified behaviors could be grouped into 3 factors. Factor I could be encountered in daily activity and mainly caused by stereotypy, and could represent manic symptoms. Factor II could be excitement symptoms caused by impulsive aggression. Factor III could be psychological irritation occasionally associated with agitation. Physical harm was included in both factor II and III, suggesting that physical harm could be caused by impulsive aggression or psychological irritation. Therefore, these behavioral symptoms need to be managed by appropriate prescription.
Neuroimaging and epilepsy
Subjects with no abnormal findings in neuroimaging studies showed higher total scores of SBDAS, suggesting that organic brain diseases often result in reduced behaviors possibly caused by decreased activity. Comai described in their reviews that the most important areas in the control of aggression are prefrontal cortex, and impairments of many neurotransmitter systems, including serotonin (5–HT), dopamine (DA), and norepinephrine (NE), are implicated in the biology of aggression [14]. Subjects with epileptic attack also showed lower total score in this study. Matthews reported that among 318 adults with intellectual disability from 40 general practices, there was no significant difference in challenging behavior between epilepsy and non–epilepsy groups [15]. Therefore, epilepsy, in itself, unlikely relates to the frequency of behavioral symptoms.
Prescription of antiepileptic
The number of antiepileptic was correlated to the lower total score of SBDAS in this study. There are a large number of studies in antiepileptic medication for the aggressive behavior [16–18]. Antiepileptic has potential to act as mood–stabilizer, but not consistently, possibly caused by instability of blood concentration and occurrence of unwilling side effect. We found that the dosage of valproic acid inversely correlated to the total score, significantly to the sub–score of self–injury and hyperactivity. Ruedrich reported that a compound of sodium valproate and valproic acid improved aggressive or self–injurious behavior in adults with intellectual disability [19]. Muehlmann made model animals of self–injury by administrating pemoline to male Long Evans rats, showing that risperidone, valproic acid and topiramate significantly attenuate pemoline–induced self–injurious behavior, and raised a possibility that valproic acid might attenuate self–injurious behavior by inhibiting monoaminergic neurotransmission through increasing extracellular GABA concentration [20].
Phenytoin showed a trend to improve the score of toilet problems and sudden agitation in this study, though the number of subjects prescribed phenytoin was small (19 out of 80 subjects). We showed that phenytoin is effective to reduce behavioral symptoms, also sudden agitation, but the number of the subject in the administration study of phenytoin was limited in our study because of the high frequency of paroxysmal tonic upgaze. Phenytoin stabilizes effectively for patients with bipolar mania [21]. Phenytoin affects voltage–gated potassium currents [22], and when treated rats with phenytoin, the expression of genes potentially associated with mechanisms of mood regulation [23]. Phenytoin was limitedly utilized as mood–stabilizer, but has potential to design another mood–stabilizer. However, the number of subjects is small in this study and for a short period, the effectiveness of phenytoin should be evaluated in a large number of subjects by long–term evaluation. It is important to follow–up the patients by neuroimaging study to prevent them from cerebellar atrophy and ataxia. On the other hand, our results did not support that carbamazepine is effective on behavioral symptoms, though the number of sample was quite small to detect a low effectiveness. While Stanford reported that carbamazepine was effective in treating impulsive aggression [24], Cueva showed in an double–blind and placebo–controlled study that carbamazepine was not effective in treating aggressive behavior of children with conduct disorder [25]. Therefore, carbamazepine should be carefully prescribed in multiple medications.
Conclusion
We scored the behavioral symptoms in intellectual disabilities by the scoring of SBDAS, and the symptoms can be classified to 3 Factors. Among antiepileptic, valproic acid was effective to control the symptoms of obsessive⁄hyperactive and self–injurious behavior. We showed that phenytoin attenuates the aggressive behavior. Because of unwilling side effect, multiple antiepileptic treatments are not recommended, and considering to the behavioral symptoms, the appropriate antiepileptic could be selected to manage behavioral symptoms in intellectual disabilities.
References
- Cooper SA, Smiley E, Jackson A, Finlayson J, Allan L, Mantry D, et al. Adults with intellectual disabilities: prevalence, incidence and remission of aggressive behaviour and related factors. J Intellect Disabil Res. 2009; 53: 217-232.
- Application of additional benefits for special care to intellectually disabled persons with severe behavior disorder: Notification No.36. Welfare Division for Persons with Disabilities, Ministry of Health and Welfare. 1998.
- Egusa Y, editor. Juusyoushinshinsyogai Ryouiku Manual (Habilitation Manual for Persons with SMID-Severe Motor and Intellectual Disabilities). 2nd edn. In: Tokyo: Ishiyaku Publishers. 1998; 39-48.
- de Winter CF, Jansen AA, Evenhuis HM. Physical conditions and challenging behaviour in people with intellectual disability: a systematic review. J Intellect Disabil Res. 2011; 55: 675-698.
- Cooper SA, Smiley E, Allan LM, Jackson A, Finlayson J, Mantry D, Adults with intellectual disabilities: prevalence, incidence and remission of self-injurious behaviour, and related factors. J Intellect Disabil Res. 2009; 53: 200-216.
- Hässler F, Reis O. Pharmacotherapy of disruptive behavior in mentally retarded subjects: A review of the current literature. Dev Disabil Res Rev. 2010; 16: 265-272.
- Shimada M, Meguro K, Inagaki H, Ishizaki J, Yamadori A. Global intellectual deterioration in Alzheimer's disease and a reverse model of intellectual development: an applicability of the Binet scale. Psychiatry Clin Neurosci. 2001; 55: 559-563.
- Orito Y, Oku H, Kubota S, Amino N, Shimogaki K, Hata M, Thyroid function in early pregnancy in Japanese healthy women: relation to urinary iodine excretion, emesis, and fetal and child development. J Clin Endocrinol Metab. 2009; 94: 1683-1688.
- Oshima K. Basic issue on severe motor and intellectual disabilities. Kosyu Eisei. 1971; 35: 648-655.
- Ono Y. Factor validity and reliability for the Aberrant Behavior Checklist-Community in a Japanese population with mental retardation. Res Dev Disabil. 1996; 17: 303-309.
- Inoue M, Okada R, Nomura K, Ueda A, Adachi J, Tsuji M, Analysis of severe behavioral disorders in people from facilities for mental retardation. Seishin Igaku. 2011; 53: 639-645.
- Crocker AG, Mercier C, Lachapelle Y, Brunet A, Morin D, Roy ME. Prevalence and types of aggressive behaviour among adults with intellectual disabilities. J Intellect Disabil Res. 2006; 50: 652-661.
- Poppes P, van der Putten AJ, Vlaskamp C. Frequency and severity of challenging behaviour in people with profound intellectual and multiple disabilities. Res Dev Disabil. 2010; 31: 1269-1275.
- Comai S, Tau M, Gobbi G. The psychopharmacology of aggressive behavior: a translational approach: part 1: neurobiology. J Clin Psychopharmacol. 2012; 32: 83-94.
- Matthews T, Weston N, Baxter H, Felce D, Kerr M. A general practice-based prevalence study of epilepsy among adults with intellectual disabilities and of its association with psychiatric disorder, behaviour disturbance and carer stress. J Intellect Disabil Res. 2008; 52: 163-173.
- Deb S, Chaplin R, Sohanpal S, Unwin G, Soni R, Lenotre L. The effectiveness of mood stabilizers and anticonvulsant medication for the management of behaviour problems in adults with intellectual disability: a systematic review. J Intellect Disabil Res. 2008; 52: 107-113.
- Stanford MS, Anderson NE, Lake SL, Baldridge RM. Pharmacologic treatment of impulsive aggression with antiepileptic drugs. Curr Treat Options Neurol. 2009; 11: 383-390.
- Jones RM, Arlidge J, Gillham R, Reagu S, van den Bree M, Taylor PJ. Efficacy of mood stabilisers in the treatment of impulsive or repetitive aggression: systematic review and meta-analysis. Br J Psychiatry. 2011; 198: 93-98.
- Ruedrich S, Swales TP, Fossaceca C, Toliver J, Rutkowski A. Effect of divalproex sodium on aggression and self-injurious behaviour in adults with intellectual disability: a retrospective review. J Intellect Disabil Res. 1999; 43 : 105-111.
- Muehlmann AM, Brown BD, Devine DP. Pemoline (2-amino-5-phenyl-,3-oxazol-4-one)-induced self-injurious behavior: a rodent model of pharmacotherapeutic efficacy. J Pharmacol Exp Ther. 2008; 324: 214-223.
- Mishory A, Winokur M, Bersudsky Y. Prophylactic effect of phenytoin in bipolar disorder: a controlled study. Bipolar Disord. 2003; 5: 464-467.
- Pisciotta M, Prestipino G. Anticonvulsant phenytoin affects voltage-gated potassium currents in cerebellar granule cells. Brain Res. 2002; 941: 53-61.
- Mariotti V, Melissari E, Amar S, Conte A, Belmaker RH, Agam G, et al. Effect of prolonged phenytoin administration on rat brain gene expression assessed by DNA microarrays. Exp Biol Med (Maywood). 2010; 235: 300-310.
- Stanford MS, Helfritz LE, Conklin SM, Villemarette-Pittman NR, Greve KW, Adams D, et al. A comparison of anticonvulsants in the treatment of impulsive aggression. Exp Clin Psychopharmacol. 2005; 13: 72-77.
- Cueva JE, Overall JE, Small AM, Armenteros JL, Perry R, Campbell M. Carbamazepine in aggressive children with conduct disorder: a double-blind and placebo-controlled study. J Am Acad Child Adolesc Psychiatry. 1996; 35: 480-490.