Research Article
Austin J Psychiatry Behav Sci. 2014;1(6): 1027.
Service Use, Physical Function, and Community Integration for People Who Were Once Homeless: a Geographic Information Systems (GIS) Approach
Chan DV1
1Department of Allied Health, University of North Carolina, USA
*Corresponding author: Chan DV, Department of Allied Health, Division of Rehabilitation Counseling and Psychology, The University of North Carolina at Chapel Hill, Campus Box 7205, Chapel Hill, NC 27599-7205, USA
Received: June 02, 2014; Accepted: July 04, 2014; Published: July 08, 2014
Introduction
The impact and prevalence of mental illness within the homeless community is often difficult to measure but estimated at 30-45% [1,2]. It is well established that people who are homeless have significant unmet physical and mental health needs [3-6]. For individuals who are homeless and have a psychiatric disability, disproportionately poorer health outcomes include increased mortality, premature death, increased use of emergency services due to advanced illness, and higher risk of communicable disease [7].
Despite the established prevalence of physical and mental health conditions while homeless, the theory of competing priorities, which identifies a hierarchy of needs by examining the needs that go unmet, suggests that meeting basic needs of food, temporary shelter, and clothing is what is most important to individuals while homeless rather than health and treatment services [4,6,8,9]. Once in housing, health outcomes research comparing individuals pre- and post-housing show housing is associated with better physical and mental health [10-12] and decreased health care utilization [13,14]. It would seem that improved health outcomes lead to improved community functioning, but individuals transitioning to permanent housing continue to struggle with social isolation, meaningful role involvement, and limited community integration.
Housing and community integration
Community integration is considered a concrete, measurable, observable manifestation of recovery [15]. Successful integration has been linked to greater self-confidence, hope, self-determination, and subjective well-being [15-17]. Wong and Solomon [18] present a conceptual framework for understanding multiple dimensions of community integration, including physical, social, and psychological integration. Physical integration considers time spent in the community, resources used, and participation in activities. Social integration includes the amount and quality of social interactions and support. Psychological integration comprises feeling connected to the community and a sense of belonging.
Community integration has received increasing attention as an ongoing challenge for individuals transitioning from homelessness into permanent housing. For example, in their first year of independent housing, people with a mental illness fostered either a sense of belonging and gains in psychological integration, or social isolation, loneliness, and limited social integration [12]. Longitudinal research also shows little change in social integration with supported housing [19]. To date, there are minimal findings related to length of time housed, specific treatment interventions, clinical symptoms, or life satisfaction associated with gains in social or psychological integration [13,20,21]. In addition, demographics of ethnic match with neighbors, and factors of age, education and length of time homeless are not significantly associated with community integration [22].
Environment and person factors affecting community integration
There is support, however, for both person and environment factors impacting integration. For example, access to public transportation and living in a higher quality neighborhood is associated with greater participation in community activities [23- 25].Similarly, level of function, symptomology, and perseveration of homeless behaviors can affect one's participation, social interactions, and affinity with the neighborhood and community. Because physical and psychosocial level of function can impact all three dimensions of community integration, disability experience must be incorporated into measures of participation and sense of community [26]. In research on community living for people with a mental illness, disability factors were significantly related to neighborhood relations, isolation, psychiatric distress, and adaptive functioning in predicting community integration outcomes, with greater psychological symptoms associated with decreased integration [27,28]. However, overall there are mixed findings related to the impact of psychiatric symptoms on integration outcomes [29,30].
If the presence of physical or psychiatric symptoms can augment physical, social and psychological integration, it is possible that treatment or service use may positively impact integration efforts [28,31]. In contrast to relying on emergency services while homeless, housing is associated with increased access to planned health care services [32]. Improved access specifically to mental health treatment with housing could mitigate psychiatric symptoms that can interfere with integration. Contingency based housing models that require treatment first, however, demonstrate poor housing stability rates compared to Housing First program models that provide individuals who are homeless immediate housing without requirements of sobriety or involvement in treatment, although substance abuse and mental health services are readily available if the person chooses to seek treatment [7,12,28]. Housing First programs are associated with decreased urgent health care utilization and decreased social service and health care expenditures, but have limited findings related to gains in community integration to date [19,33-35].
Difficulty measuring community integration
Because of the complexity of the integration process, research strategies that can obtain valid assessments of the community integration processes and the effectiveness of interventions from a multi-dimensional approach are needed [25,36]. There is also a call for individual determinants of how "community" is defined and measured [28], particularly as many meaningful activities often occur outside the boundaries of one's neighborhood [37,38]. One such method uses participatory mapping, where individuals identify places in the community that are important to them through drawing personal maps, in conjunction with Geographic Information Systems (GIS), which plots these locations on a geographic map [17]. Combining information from participatory mapping and GIS to create an individual's "activity space" shows promise in mixed methods research to meet the methodological challenges of measuring multiple aspects of re-integration. Activity space is the subset of all locations within which an individual has direct contact as a result of day-to-day activities, such as work, shopping, and interacting with friends and family [39]. Activity space size can be compared by area and related to other measures of community integration or function.
A study using GIS and participatory mapping techniques to measure community integration for people who have a serious mental illness, but not previously homeless, found those with larger activity spaces had greater life satisfaction, but less sense of community compared to those with smaller activity spaces [17]. Previous research replicating these methods with individuals with disabilities who were formerly homeless did not find that community integration outcomes varied by measures of spatial presence in the community, but rather that larger activity spaces were associated with greater use of homeless services that were geographically spread throughout the city [40]. Level of function, however, was not included in the analysis, which could impact integration efforts.
The purpose of this exploratory study was to extend the prior research by completing a secondary analysis to examine differences in GIS measures of community integration related to service use and health function in adults with disabilities who were previously homeless. The research was guided by five questions: 1) What types of services are individuals using after housing? 2) Does treatment use correspond to better community integration outcomes? 3) Are there specific services associated with better community integration outcomes? 4) Is there a significant difference in community integration for individuals with the presence of a psychiatric disorder? 5) What is the relationship between physical function and community integration? It was hypothesized that better function and use of more treatment services would be associated with better community integration, using multiple measures of integration
Materials and Methods
Participants
Data was collected from 37 individuals with a history of homelessness who now had permanent housing in Boston, MA, USA. All participants self-reported a physical or psychiatric disability, with 62% reporting both. Participants were recruited from one of two housing programs that consisted of either scatter site housing (40.5%) or single room occupancy in congregate housing (59.5%). Demographics for the sample are included in Table 1. All participants were recruited from a larger ongoing study teaching Life Skills in Food and Nutrition Management, Home and Self-Care, Safe Community Participation, and Money Management in a group setting [41-44].
Age
Mean
52.4(SD=7.8)
Range
28-65 years
Gender
Male
45.9%
Female
54.1%
Ethnicity
White
51.4%
African American
43.2%
Other
5.4%
Education
Some High School
18.9%
High School
29.7%
Some College
27.0%
College Graduate
24.3%
Primary Psychiatric Diagnosis
Mood
45.9%
Anxiety
13.5%
Schizophrenia
5.4%
Personality
2.7%
None
32.4%
Primary Physical Diagnosis
Orthopedic/Bone/Joint
Cardiac/Pulmonary
32.4%
45.9%
Other
13.5%
None
8.1%
Housing Site
Congregate SRO
59.5%
Independent
40.5%
Substance Abuse
History of Use
66.7%
Current Usea
35.1%
Employment status
Unable due to disability
62.2%
Time Homeless
Mean
Range
8 years (SD 11 yrs)
6 mo - 47 years
Time Housed
Mean
Range
4 years (SD 4 yrs)
1 mo - 16 years
Income
Mean
Range
$9,182� (SD $5,035)
$0 - $23,000
Table 1: Demographic characteristics of the sample (N = 37).
Measures
Demographics
Demographic information was obtained through the Survey of Income and Program Participation (SIPP; 45). The SIPP was administered as part of the larger Life Skills Study, typically within 3 months of the interview for the current study.
Service Use
The SIPP also included questions regarding current use of 13 psychiatric rehabilitation services: case management, vocational programs, job coaching or supported employment, mental-illness/ substance abuse services (e.g., AA or NA), housing program/supported housing services; treatment groups, self-help groups, support groups, day programming, drop-in services, seeing a psychiatrist, and seeing a therapist, psychologist, or social worker. Answers consisted of a Yes/No categorical response. The number of services used was also summed for a total service use score.
Function
Questions regarding current function were assessed through 24itemsin the SIPP. Examples of physical functional questions include whether one has difficulty lifting 10 pounds, walking, stooping crouching or kneeling, reaching overhead, using the stairs, hearing normal conversation, seeing, getting out of a chair, sitting or standing for one hour, and performing basic activities of daily living (ADLs) such as bathing, dressing, and eating. Answers to functional items also consisted of Yes/No categorical responses. A total functional score was obtained by summing the number of items individuals indicated difficulty with, where higher scores indicated lower functional ability. Use of assistive devices and specific use of a cane was also queried. Additional questions related to psychosocial function included difficulty coping with day-to-day stresses, concentrating long enough to finish everyday tasks, and getting along with people and making or keeping friends. Participants were also asked to rate their health in general as either "Excellent,""Very good,""Good,""Fair," or "Poor." Current medication use and difficulty taking medications were also examined.
Community integration
A 20-item community integration questionnaire, termed the "Integration Assessment" was created from existing community integration measures. Eight questions measured physical integration [46,47], 7 questions measured social integration (taken from the Participation Objective, Participation Subjective [POPS, 48]), and 5 questions measured psychological integration (taken from the Community Integration Measure [CIM, 49]). Each item was rated on a 5 point Likert scale ranging from "Never" to "Very Often" for how often one participated in community activities or social interactions and from "Strongly Disagree" to "Strongly Agree" for questions related to how much one felt a part of the community.
GIS
Using a participatory mapping technique, participants produced sketch maps of locations, activities, and resources in the community they identified as important. Addresses for locations on these drawn maps were identified through Google Maps and geocoded using gpsvisualizer.com to obtain the latitude and longitude coordinates. Once geocoded, locations were plotted on a geographic map using ArcGIS v.10.0. GIS analysis calculated the area of each individual's "activity space" using a one standard deviation ellipse, which captures 66% of the locations identified to represent the participant's general spatial distribution of interactions in the community. Use of the one standard deviation ellipse is a typical measure of spatial presence and is highly correlated with other spatial measures such as the convex hull approach, which encompasses all locations identified [38,40]. In addition to the area of the activity space size, a count was completed of the total number of locations identified. Each location was grouped into one of five categories: Instrumental Activities of Daily Living (IADLs), Vocational, Leisure/Recreational, Health, and Homeless Services (Table 2). Due to the range in number of locations identified, instead of relying on comparisons of count data, the proportion of each of these locations identified as important was calculated for comparison to the other measures.
Type of location
Examples
Health
Hospitals, community health clinics, counseling, pharmacy
Instrumental Activities of Daily Living (IADL)
Banking, grocery shopping, post office, paying bills, laundry, transportation stops
Leisure
Parks, libraries, coffee shops, churches, restaurants, movie theatres
Homeless Services
Shelters, food pantries, housing programs, community centers
Vocational
Employment, school, volunteer locations
Table 2: The five categories of types of locations identified with examples.
Data collection
Data collection for the participatory mapping interview and drawing activity consisted of individual in-person interviews. After completing Integration Assessment, individuals were given a blank sheet of paper and asked to draw any current locations, activities, or resources important to them [17]. Following this drawing activity, all participants complete a semi-structured interview to narrate the personal meaning of these places. Participants received a $10 grocery store gift card for their time. The Boston University review board approved all aspects of this study. Additional information regarding the above procedures and measures can be found in a related study [40].
Data analysis
Results of service use and health function were compared to the integration assessment, spatial measures of community integration, and the number and types of locations identified. Despite a small sample, data analyses included Chi-square using Fisher's exact test and one-way between subjects ANOVA tests for differences in health function, service use and community integration measures based on demographic variables, including the presence or absence of a psychiatric disability.
Service use
Frequency counts were completed for each type of service used. Differences in service use by categorical demographic variables were tested with Chi Square using SPSS v.21. Pearson product-moment correlation coefficients were computed to assess the relationship between total service use and activity space size, total number of locations identified, and percentage of types of locations identified. Data was also analyzed using independent t tests for differences in community integration measures and level of function based on use of specific services.
Function
Because of low endorsement (N= 7 or fewer) of difficulty with bathing, dressing, eating, using the bathroom, getting around inside the home, getting in and out of bed or a chair, performing light housework, and preparing meals, these 9items were consolidated into one item representing whether one had difficulty with basic functions. The resulting total physical function score consisted of 15 items. Additional questions related to use of a cane, use of an assistive device and the three psychosocial questions were analyzed separately. Total functional score and perceived health rating were correlated with total service use and community integration measures. Based on initial findings, subsequent analysis comparing differences in community integration measures based on the ability to perform specific functions was explored using independent samples t test. Since this was primarily an exploratory study of health function and community integration, conservative adjustments of Type 1 error rates for multiple comparisons was deemed premature because it was more important to identify promising leads in the effects associated with successful integration [27]. As a byproduct, it is possible that spurious effects may have been incorrectly identified, but future studies will likely weed them out. Because of the small sample and likelihood of unequal variances, results were checked for significance when unequal variance was assumed and not assumed.
Results
Sixty-eight percent of participants self-reported a psychiatric disability (N= 25, Table 1), with 42% of these participants reporting multiple psychiatric disorders (Table 3). Depression was the most common reported single and co-occurring diagnosis, followed by Post Traumatic Stress Disorder (PTSD), and bipolar disorder. Participants with a psychiatric disability had significantly lower physical integration scores compared to individuals who did not report the presence of a psychiatric disability, but did not differ in social or psychological integration, number of locations identified, or activity space size (Table 4). Participants with psychiatric disabilities also identified a significantly lower proportion of leisure locations and a significantly higher percentage of health related locations as important compared to those without a psychiatric disability. There was no significant difference, however, in reported health function or general health ratings between these groups.
Diagnosis
Total sample
(N= 37)
Participants with psychiatric disability
(N = 25)
Single Diagnosisa
(N = 13)
Co-occurringa
(N = 12)
Depression
45.9%
68.0%
40.0%
28.0%
PTSD
21.6%
32.0%
8.0%
24.0%
Bipolar
18.9%
28.0%
4.0%
24.0%
Anxiety
16.2%
24.0%
0%
24.0%
Schizophrenia
5.4%
8.0%
0%
8.0%
Borderline Personality
2.7%
4.0%
0%
4.0%
Table 3: Frequency of diagnosis reported by total sample, participants with a psychiatric disability, and single versus co-occurring disorders.
Service use
Participants averaged three different types of services used (= 3.32, SD = 1.99, range 0 - 10). The most frequently reported services used were case management (73.0%), seeing a therapist, psychologist, or social worker (59.5%), housing program or supported housing (54.1%), and seeing a psychiatrist (51.4%). For physical health care, 86.4% of the sample reported having a primary care visit in the last three months, whereas only 13.5% reported use of emergency department services during that same time.
There were limited demographic differences in service use with a few exceptions. First, people with psychiatric disabilities were more likely to be seeing a psychiatrist (χ2 = 45.9% vs. 29.7%, p = .002) and/ or a counselor, social worker, or psychologist than individuals who did not report the presence of a psychiatric disability (χ2 = 54.1% vs, 29.7%, p< .001).Second, women were more likely to report seeing a therapist, social worker, or psychologist than men (χ2 = 70% vs. 30%, p =0.007). Finally, when examining total services use, there was a weak to moderate negative correlation between length of time housed and service use (r = -.336, p = .042), perhaps suggesting some stability with housing tenure and less reliance on services. The low frequency of use of the remainder of services, including treatment groups and vocational services (N = 6 or less) prohibited meaningful analyses, however observed trends are noted below.
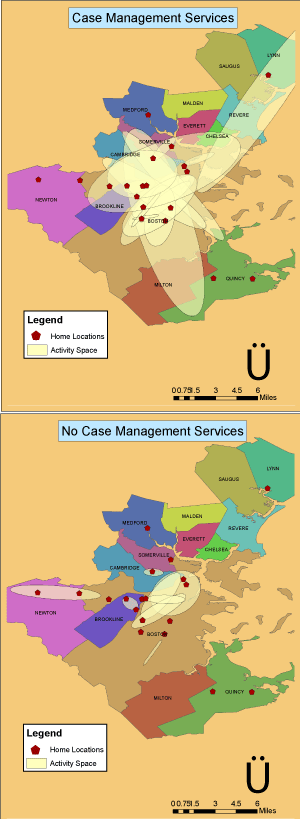
In comparing community integration measures by use of services, participants who used case management services had significantly larger activity spaces and significantly better psychological integration or feelings of belonging than those who were not involved with case management (Table 4 and Figure 1). Participants who reported seeing a psychiatrist had significantly higher scores of total function overall, but did not differ in self-perceived ratings of general health or any community integration measures.
Figure 1 :Comparison of activity space size by use of case management services. approaches.
Community Integration
Psychiatric Disability
Case Management
Psychiatrist
Mean (SD)
N = 37
Yes
(N =25)
No
(N =12)
Yes
(N =27)
No
(N = 10)
Yes
(N = 19)
No
(N = 18)
Participatory Mapping/GIS
Activity Space (mi2)
9.13 (12.69)
9.43
8.51
7.17*
2.07*
9.94
8.28
Number of Locations
12.65 (6.46)
12.72
12.50
12.96
11.80
12.11
13.22
Integration Assessment
Physical
19.76 (4.83)
18.48
22.42*
19.59
20.20
18.89
20.67
Social
22.11 (4.90)
21.44
23.50
22.70
20.50
21.47
22.78
Psychological
18.11 (4.58)
18.16
18.00
19.30*
14.90*
18.26
17.94
Physical Function
5.65 (4.1)
6.20
4.50
5.70
5.50
7.32
3.89*
Health Rating
2.43 (0.96)
2.36
2.58
2.41
2.50
2.37
2.50
Locations
IADL
.27 (0.16)
.27
.19
.28
.26
.25
.30
Health
.20 (0.16)
.20
.02*
.20
.19
.21
.18
Vocational
.03 (0.07)
.03
.06
.02
.06
.02
.04
Homeless Services
.09 (0.11)
.12
.07
.09
.09
.1
.1
Leisure
.37 (0.17)
.32
.54*
.39
.32
.37
.38
Table 4: Differences in community integration, health function and percentage of types of locations identified as important based on presence of a psychiatric disability and use of case management and psychiatric services.
Finally, number of locations identified overall was moderately correlated with total services used (r = .379, p = .021). The use of multiple services could certainly contribute to an increased number of locations identified, if these related locations were identified as important, but this relationship could also speak to the potential effects of these services to increase the individual's engagement in the community. For example, examining the trends of the lesser reported services used suggests participants who attended self-help groups and treatment groups had significantly more locations identified (= 21.67 vs. 11.85, p = .010;= 23.67 vs. 11.68, p = .001, respectively). The social interaction of those attending treatment groups may contribute to increased awareness of and comfort with participating in community activities.
Function
Total functional score for the sample averaged5.65 (SD = 4.1, range 0 - 14) across the 15physical health related items. Activities with the most frequent reports of difficulty included lifting over 25 pounds (62.2%), standing over one hour (56.8%), and stooping/kneeling (54.1%). In addition, many participants reported trouble coping with day to day stress (45.9%) and difficulty concentrating long enough to finish everyday tasks (32.4%). Over 90% of participants reported taking some form of medication, for physical (35.1%), psychological (8.1%), or both (35.1%) conditions (note, 10.8% unreported). Average self-perceived health rating on the 5 point scale was 2.43, corresponding to a rating between "Fair" (2) and "Good" (3) health, but "Fair" (2) was both the median and mode.
There were no significant relationships between spatial measures of community integration and total function or health ratings. It is of note that there was an unexpected significant negative relationship between the measure of total function and self-reported health rating, where higher levels of function were associated with lower health ratings. Examining t-test comparing specific functional abilities with community integration from the exploratory analysis revealed participants who reported trouble getting along with people and making or keeping friends had significantly lower social integration ( = 17.60 vs. 22.81, p = .025), consistent with the intent of the subscale measure. Although there were minimal findings related to community integration and physical function, some additional trends were noted when looking at specific functional activities that may impact community integration. For example, people who reported difficulty seeing had significantly smaller activity spaces than those without vision problems ( = 1.93 vs. 7.21, p = .023), whereas those who reported difficulty sitting for one hour had significantly larger activity spaces ( = 10.70 vs. 2.83, p = .050). In addition, participants who reported trouble concentrating long enough to finish everyday tasks had significantly more locations identified compared to those who did not have difficulty with concentration ( = 15.67 vs. 11.20, p = .047). The above results are noted as additional trends observed in this exploratory study, but interpreted with caution due to small sample size or marginal significance.
When comparing level of function to the proportion of different types of locations identified as important, limitations in a number of areas were associated with significantly less use of IADL locations, namely use of an assistive device and use of a cane specifically, difficulty lifting 10 pounds, and difficulty walking (Table 5). A similar pattern emerged with individuals reporting less use of homeless service locations, reported by those who have difficulty lifting 10 pounds, stooping or kneeling, and using the stairs. At the same time, those who reported difficulty stooping or kneeling, using the stairs, or walking identified significantly more leisure/recreation locations. However, those with difficulty lifting 25 pounds had less leisure locations identified. Individuals who had difficulty stooping, using the stairs, or walking, along with those reporting difficulty with reaching overhead or sitting over one hour also had significantly lower self-perceived health ratings.
Community Integration
Difficulty Lifting 10#
Uses a Cane
Uses an Assistive Device
Yes
(N =18)
No
(N =19)
Yes
(N =11)
No
(N = 26)
Yes
(N = 13)
No
(N = 24)
Participatory Mapping/GIS
Activity Space (mi2)
5.19
12.87
9.35
9.04
9.56
8.90
No. Locations
12.17
13.11
5.64
9.85*
12.00
13.00
Integration Assessment
Physical
19.06
20.42
19.38
20.64
19.92
19.67
Social
19.78
24.32*
21.09
22.54
21.54
22.42
Psychological
16.33
19.78*
18.27
18.04
18.15
18.08
Physical Function
8.72
2.74*
7.00
5.08
7.15
4.83
Health Rating
2.28
2.58
2.27
2.50
2.38
2.46
Locations
IADL
.22
.33*
.17
.32*
.17
.33*
Health
.24
.16
.22
.18
.23
.18
Vocational
.05
.02
.00
.05*
.02
.04
Homeless Services
.05
.13*
.08
.10
.10
.08
Leisure
.40
.35
.40
.36
.45
.33*
Table 5: Differences in community integration, health function, and percentage of types of locations identified as important based on function by specific function.
Community Integration
Difficulty Walking
Difficulty Stooping or Kneeling
Difficulty Using Stairs
Yes
(N =10)
No
(N =27)
Yes
(N =20)
No
(N = 17)
Yes
(N = 19)
No
(N = 18)
Participatory Mapping/GIS
Activity Space (mi2)
7.96
9.57
5.36
13.57
10.31
7.89
No. Locations
11.80
12.96
12.55
12.76
12.47
12.83
Integration Assessment
Physical
18.90
20.07
19.90
19.59
19.37
20.17
Social
20.10
22.85
20.95
23.47
21.21
23.06
Psychological
17.40
18.37
17.40
18.94
17.11
19.17
Physical Function
8.75
3.29*
8.60
2.18*
8.32
2.83*
Health Rating
2.20
2.52*
2.05
2.88*
2.00
2.89*
Locations
IADL
.18
.31*
.25
.31
.24
.31
Health
.20
.20
.20
.20
.20
.20
Vocational
.06
.02
.05
.02
.05
.01
Homeless Services
.04
.11
.04
.15*
.05
.14*
Leisure
.49
.33*
.42
.31*
.43
.31*
Table 5: Continued.
Community Integration
Difficulty Reaching Overhead
Yes
(N =15)
No
(N =22)
Participatory Mapping/GIS
Activity Space (mi2)
12.40
6.91
No. Locations
13.53
12.05
Integration Assessment
Physical
17.80
21.09*
Social
21.07
22.82
Psychological
17.87
18.27
Physical Function
9.07
3.32
Health Rating
1.93
2.77*
Locations
IADL
.26
.28
Health
.22
.18
Vocational
.06
.01
Homeless Services
.05
.12
Leisure
.43
.33
Table 5: Continued.
Discussion
In examining service use of individuals who were previously homeless who transitioned into permanent housing, the current study showed the majority of individuals who reported having a psychiatric disability were significantly more likely to be receiving psychiatric services than those who did not have a psychiatric disability. Although this finding seems intuitive, in conjunction with the finding that health-related locations were identified at significantly higher rates as important, the fact that over 70% of participants reporting a psychiatric disability are currently receiving psychiatric or counseling services lends support for mental health treatment becoming a priority once stable housing is obtained. While homeless, individuals frequently report mental health treatment as a low priority, even when it is rated as easy to obtain [4, 50-52]. Consistent with the theory of competing priorities, one explanation proposed is that individuals, such as those who have a psychiatric disability, who have more difficulty meeting basic needs, are less likely to seek mental health treatment [53]. Obtaining permanent housing provides the opportunity for stability in areas of personal health, safety, meaningful relationships and stable resources not often found while homeless [12,34,54]. The current research suggests that once in stable housing, individuals with psychiatric disabilities are seeking and receiving treatment and specifically identifies health related locations at a high level of importance. In addition, the majority of the sample was actively using primary care and preventative services, with low use of emergency services. These findings lend support for the vision of Housing First program models, that if given a safe, stable place to live, other areas of stability of health and mental health treatment will fall into place [55].
Contrary to expectations, health and mental health treatment use was not associated with better community integration, as assessed through multiple dimensions. However, findings from the current study suggest individuals receiving case management services had greater feelings of belonging to their community and geographically larger defined areas of "community". High rates of case management services were expected as a common component of supported housing and it is certainly possible these individuals were connected to more resources in the community through case management services. Benefits of case management services are well documented in the literature. When coupled with supported housing for people who were once homeless, case management is associated with cost savings [56], improved access to health care [57], self-perceived improvements in health [58], and better quality of life [59]. The current study contributes to the literature by suggesting that involvement in case management can also positively impact community engagement and spatial extent in the community. The importance of individuals increasing their physical presence in the community can be seen as social isolation continues to characterize the transition from homelessness to permanent housing. Although a larger spatial presence in the community is not equivalent to social and psychological integration, there is support that increased physical presence is associated with greater opportunity to make social contacts [16].
The difference in physical function related to seeing a psychiatrist but not associated with seeing a therapist, social worker or psychologist is unclear, particularly in light of the high rates of medication use for both physical and psychiatric conditions by the majority of the sample. There were no other significant differences in medication use that would seem to account for these findings. Ratings of perceived health, which could have certainly included both physical and mental health in the individual's consideration, also did not differ. It is possible that individuals specifically seeing a psychiatrist for medications may have improved psychiatric symptoms, but the relationship to physical functioning is not well documented in the literature. The absence of an objective or subjective measure of psychiatric symptoms is a main limitation to the study.
There is some evidence that limitations in function related to vision and mobility also limited integration efforts and one's physical presence in the community, whereas discomfort with prolonged sitting may encourage mobility and exploring the community area. It is noted that use of a cane or other assistive devices did not appear to impact individual's function, perceived health ratings, or community integration, including measures of spatial extent in the community, which may support increased function with use. The limited number of types of locations identified as important and lower perceived health ratings associated with those reporting mobility issues suggest a need for additional assistance, particularly with IADL related locations. Although Boston is an accessible city that offers public transportation and has a high walkability index, IADL locations such as going grocery shopping often include a level of difficulty that is physically taxing. In research on individuals with multiple sclerosis, even mild mobility loss was associated with substantial limitation in IADL function [60]. Without personal vehicles, participants in the current study relied on walking, public transportation, or housing shuttles where they could only shop for as many items as they could carry.
Limitations in mobility were also associated with less homeless service locations and more leisure locations. As mentioned above, results of the prior research identified homeless service locations were geographically spread throughout the Boston area, often far from the participant's new homes [40]. For those with less mobility, the distance associated with these locations may make it more difficult to continue to access these services. However, leisure based locations, such as going to a park, going for a walk in the neighborhood, coffee shops, or fast food restaurants may be activities within one's immediate area, and therefore may be more accessible than locations related to health services, vocational activity or homeless services, and less demanding than IADL locations. Despite limitations in function, these individuals were still able to engage in leisure locations. These are encouraging findings based on previous self-reported skill deficits in leisure engagements for people who are homeless [61]. Findings from the related study indicate high prevalence and importance of leisure based activities for these individuals who have transitioned to permanent housing [40]. The current results suggest, however, that there perhaps is a threshold in function corresponding to medium level strength that prohibits use of leisure activities.
Limitations
Although the current study attempted to assess the relationship between health function, service use, and community integration, there were several limitations. First, there was no objective measure of physical functioning. Similarly, as noted above, there was no objective or subjective measure of psychiatric symptoms or function, which can contribute to community integration. Increased psychiatric symptoms are related to decreased community integration, and specifically decreased psychological integration [28]. In addition, the question asking participants to rate their health "in general" did not specify whether this assessment included both physical and mental health. This ambiguity may contribute to the unexpected finding of the inverse relationship between physical health function score summed from self-reported activities, and perceived health ratings. There is some evidence to support that, when asked to rate health, individuals who are homeless or vulnerably housed include both physical and mental health [62]. There is also a potential issue of order effects in these questions. Namely, the perceived health rating question occurs before questions regarding the specific items related to physical and psychosocial functioning. It is possible that if individuals were asked to rate their overall health after considering each individual item, the relationship may have been more consistent with responses to individual items.
Additional limitations include a small sample size limiting generalizability of findings, lack of a comparison group from the general population, recruitment based on participation in an intervention study, and a lack of information on the proximity or accessibility of treatment services that could impact utilization. As this was a secondary analysis of health and service use data, it was also unclear where case management services in particular took place, and at what frequency, which could be important considerations. It is possible these meetings occurred at various locations in the community, which could contribute to the idea of exposure to different resources, creating larger activity spaces. Case management activities would have been categorized as a homeless service location, which was also associated with larger activity spaces in the prior study, providing some support for this notion. Further research is needed to assess the proximity of services and activity locations identified as important for integration, and the impact of psychiatric services on physical function.
Conclusion
This study examined the impact of use of specific psychiatric services and physical function on community integration, as measured through multiple dimensions. Consistent with previous research, after obtaining stable housing individuals reported high rates of planned health care utilization in primary care visits and higher rates of psychiatric services by individuals with psychiatric disabilities. Although there were significant differences in physical integration and the importance of health locations for individuals with psychiatric disabilities, the overall lack of findings add support to prior research on the homogeneity of needs across disability status and diagnoses [33,63-65]. These findings overall present policy implications of broad structural solutions and less segmenting of the population.
As individuals move from homelessness into housing, identifying the external supports that will best augment their personal strengths to move beyond housing into community integration and meaningful role involvement will receive increasing attention from service provision and individual perspectives. Individuals continued to have high rates of health needs following housing, but with supports such as case management they may be better able to access needed services. Results from the current study suggest case management services may also keep people with disabilities who are transitioning to permanent housing connected to the community and geographically expand opportunities to build resources and social connections. Longitudinal investigations of how needs change as individuals transition into housing are needed in future research.
References
- Substance Abuse and Mental Health Services Administration. Blueprint for change: Ending chronic homelessness for persons with serious mental illness and/or co-occurring substance abuse disorders. Rockville, MD: U.S. Department of Health & Human Services. 2003.
- U.S. Department of Housing and Urban Development. The 2008 annual homeless assessment report to Congress. Washington, D.C: U.S. Department of Housing and Urban Development; Office of Policy and Development Research. 2009.
- Baggett TP, O'Connell JJ, Singer DE, Rigotti NA. The unmet health care needs of homeless adults: a national study. Am J Public Health. 2010; 100: 1326-1333.
- Garibaldi B, Conde-Martel A, O'Toole TP. Self-reported comorbidities, perceived needs, and sources for usual care for older and younger homeless adults. J Gen Intern Med. 2005; 20: 726-730.
- Martins DC. Experiences of homeless people in the health care delivery system: a descriptive phenomenological study. Public Health Nurs. 2008; 25: 420-430.
- O'Toole TP, Pollini RA, Ford DE, Bigelow G. The health encounter as a treatable moment for homeless substance-using adults: The role of homelessness, health seeking behavior, readiness for behavior change and motivation for treatment. Addict Behav. 2008; 33: 1239-1243.
- Massachusetts Housing and Shelter Alliance. Home and healthy for good: A statewide pilot Housing First program. Progress report. 2008
- Gelberg L, Browner CH, Lejano E, Arangua L. Access to women's health care: a qualitative study of barriers perceived by homeless women. Women Health. 2004; 40: 87-100.
- Power R, Hunter G. Developing a strategy for community-based health promotion targeting homeless populations. Health Educ Res. 2001; 16: 593-602.
- Drury LJ. From homeless to housed: caring for people in transition. J Community Health Nurs. 2008; 25: 91-105.
- Mares AS, Rosenheck RA. One-year housing arrangements among homeless adults with serious mental illness in the ACCESS program. Psychiatr Serv. 2004; 55: 566-574.
- Yanos PT, Barrow SM, Tsemberis S. Community integration in the early phase of housing among homeless persons diagnosed with severe mental illness: successes and challenges. Community Ment Health J. 2004; 40: 133-150.
- Baumgartner JN, Herman DB. Community integration of formerly homeless men and women with severe mental illness after hospital discharge. Psychiatr Serv. 2012; 63: 435-437.
- Sadowski LS, Kee RA, VanderWeele TJ, Buchanan D. Effect of a housing and case management program on emergency department visits and hospitalizations among chronically ill homeless adults: a randomized trial. JAMA. 2009; 301: 1771-1778.
- Bond GR, Salyers MP, Rollins AL, Rapp CA, Zipple AM. How evidence-based practices contribute to community integration. Community Ment Health J. 2004; 40: 569-588.
- Prince PN, Gerber GJ. Subjective well-being and community integration among clients of assertive community treatment. Qual Life Res. 2005; 14: 161-169.
- Townley G, Kloos B, Wright PA. Understanding the experience of place: expanding methods to conceptualize and measure community integration of persons with serious mental illness. Health Place. 2009; 15: 520-531.
- Won YL, Solomon PL. Community integration of persons with psychiatric disabilities in supportive independent housing: a conceptual model and methodological considerations. Ment Health Serv Res. 2002; 4: 13-28.
- Tsai J, Mares AS, Rosenheck RA. A multisite comparison of supported housing for chronically homeless adults: "Housing First" versus "residential treatment first". Am J Community Psychol. 2011; 48: 341-351.
- Nemroff R, Aubry T, Klodowsky F. From homelessness to community: Psychological integration of women who have experienced homelessness. J Community Psychol. 2011; 39: 1003-1018.
- Tsai J, Rosenheck RA. Conceptualizing social integration among formerly homeless adults with severe mental illness. J Community Psychol. 2012; 40: 456-467.
- Yanos PT, Felton BJ, Tsemberis S, Frye VA. Exploring the role of housing type, neighborhood characteristics, and lifestyle factors in the community integration of formerly homeless persons diagnosed with mental illness. J of Ment Health. 2007; 16: 703-717.
- Iwarsson S, Ståhl A. Accessibility, usability and universal design--positioning and definition of concepts describing person-environment relationships. Disabil Rehabil. 2003; 25: 57-66.
- Ståhl A, Carlsson G, Hovbrandt P, Iwarsson S. "Let's go for a walk!": identification and prioritisation of accessibility and safety measures involving elderly people in a residential area. Eur J Ageing. 2008; 5: 265-273.
- Kloos B, Shah S. A social ecological approach to investigating relationships between housing and adaptive functioning for persons with serious mental illness. Am J Community Psychol. 2009; 44: 316-326.
- Townley G, Kloos B. Development of a measure of sense of community for individuals with serious mental illness residing in community settings. J Community Psychol. 2009; 37: 362-380.
- Abdallah C, Cohen CI, Sanchez-Almira M, Reyes P, Ramirez P. Community integration and associated factors among older adults with schizophrenia. Psychiatr Serv. 2009; 60: 1642-1648.
- Gulcur L, Tsemberis S, Stefancic A, Greenwood RM. Community integration of adults with psychiatric disabilities and histories of homelessness. Community Ment Health J. 2007; 43: 211-228.
- Davis BA, Townley G, Kloos B. The roles of clinical and nonclinical dimensions of recovery in promoting community activities for individuals with psychiatric disabilities. Psychiatr Rehabil J. 2013; 36: 51-53.
- Yanos PT, Stefancic A, Tsemberis S. Objective community integration of mental health consumers living in supported housing and of others in the community. Psychiatr Serv. 2012; 63: 438-444.
- Kloos B, Townley G. Investigating the relationship between neighborhood experiences and psychiatric distress for individuals with serious mental illness. Adm Policy Ment Health. 2011; 38: 105-116.
- Bean KF, Shafer MS, Glennon M. The impact of housing first and peer support on people who are medically vulnerable and homeless. Psychiatr Rehabil J. 2013; 36: 48-50.
- Martinez TE, Burt MR. Impact of permanent supportive housing on the use of acute care health services by homeless adults. Psychiatr Serv. 2006; 57: 992-999.
- Padgett DK. There's no place like (a) home: ontological security among persons with serious mental illness in the United States. Soc Sci Med. 2007; 64: 1925-1936.
- Wong YI, Hadley TR, Culhane DP, Poulin SR, Davis MR, Cirksey BA, et al. Predicting staying or leaving in permanent supportive housing that serves homeless people with serious mental illness. Washington, D.C.: U.S. Department of Housing and Urban Development; Office of Policy and Development Research. 2006.
- Lemaire GS, Mallik K. Barriers to community integration for participants in community-based psychiatric rehabilitation. Arch Psychiatr Nurs. 2005; 19: 125-132.
- Wong DW, Shaw SL. Measuring segregation: an activity space approach. J Geogr Syst. 2011; 13: 127-145.
- Zenk SN, Schulz AJ, Matthews SA, Odoms-Young A, Wilbur J, Wegrzyn L, et al. Activity space environment and dietary and physical activity behaviors: a pilot study. Health Place. 2011; 17: 1150-1161.
- Nemet GF, Bailey AJ. Distance and health care utilization among the rural elderly. Soc Sci Med. 2000; 50: 1197-1208.
- Chan DV, Helfrich CA, Hursh NC, Rogers ES, Gopal S. Measuring community integration using Geographic Information Systems (GIS) and participatory mapping for people who were once homeless. Health Place. 2014; 27: 92-101.
- Zimolag U, Krupa T. Pet ownership as a meaningful community occupation for people with serious mental illness. Am J Occup Ther. 2009; 63: 126-137.
- Helfrich CA. Food management: A life skills intervention. Chicago: University of Illinois at Chicago. 2006a.
- Helfrich CA. Money management: A life skills intervention. Chicago: University of Illinois at Chicago. 2006b.
- Helfrich CA. Room and self care: A life skills intervention. Chicago: University of Illinois at Chicago. 2006c.
- Helfrich CA. Safe community participation: A life skills intervention. Chicago: University of Illinois at Chicago. 2006d.
- Segal SP, Aviram U. The mentally ill in community-based sheltered care: A study of community care and social integration. New York: John Wiley & Sons, Inc. 1978.
- United States Census Bureau. Survey of Income and Program Participation (SIPP). 2012. Retrieved. 2009.
- Brown M, Dijkers MP, Gordon WA, Ashman T, Charatz H, Cheng Z. Participation Objective, Participation Subjective: A measure of participation combining outsider and insider perspectives. J Head Trauma Rehabil. 2004; 19: 459-481.
- McColl MA, Davies D, Carlson P, Johnston J, Minnes P. The community integration measure: development and preliminary validation. Arch Phys Med Rehabil. 2001; 82: 429-434.
- Acosta O, Toro PA. Let's ask the homeless people themselves: a needs assessment based on a probability sample of adults. Am J Community Psychol. 2000; 28: 343-366.
- Herman DB, Struening EL, Barrow SM. Self-reported needs for help among homeless men and women. Eval Program Plann. 1994; 17: 249-256.
- Mosher-Ashley PM, Henrikson N. Shelter-based services in Massachusetts for homeless adult individuals. Soc Work Health Care. 1997; 26: 15-32.
- Sullivan G, Burnam A, Koegel P, Hollenberg J. Quality of life of homeless persons with mental illness: results from the course-of-homelessness study. Psychiatr Serv. 2000; 51: 1135-1141.
- Nelson G, Clarke J, Febbraro A, Hatzipantelis M. A narrative approach to the evaluation of supportive housing: stories of homeless people who have experienced serious mental illness. Psychiatr Rehabil J. 2005; 29: 98-104.
- Pathways to Housing, Inc., New York. 2005 APA Gold Award: Providing housing first and recovery services for homeless adults with severe mental illness. Psychiatr Serv. 2005; 56: 1303-1305.
- Basu A, Kee R, Buchanan D, Sadowski LS. Comparative cost analysis of housing and case management program for chronically ill homeless adults compared to usual care. Health Serv Res. 2012; 47: 523-543.
- Nath SB, Irene Wong YL, Marcus SC, Solomon P. Predictors of Health Services Utilization among Persons with Psychiatric Disabilities Engaged in Supported Independent Housing. PsychiatrRehabil J. 2012; 35: 315-323.
- Davis E, Tamayo A, Fernandez A. "Because somebody cared about me. That's how it changed things": homeless, chronically ill patients' perspectives on case management. PLoS One. 2012; 7: e45980.
- O'Connell MJ, Kasprow W, Rosenheck RA. Rates and risk factors for homelessness after successful housing in a sample of formerly homeless veterans. Psychiatr Serv. 2008; 59: 268-275.
- Salter AR, Cutter GR, Tyry T, Marrie RA, Vollmer T. Impact of loss of mobility on instrumental activities of daily living and socioeconomic status in patients with MS. Curr Med Res Opin. 2010; 26: 493-500.
- Tryssenaar J, Jones EJ, Lee D. Occupational performance needs of a shelter population. Can J Occup Ther. 1999; 66: 188-196.
- Gadermann AM, Hubley AM, Russell LB, Palepu A. Subjective health-related quality of life in homeless and vulnerably housed individuals and its relationship with self-reported physical and mental health status. Soc Indic Res. 2014; 116: 341 - 352.
- Mojtabai R. Perceived reasons for loss of housing and continued homelessness among homeless persons with mental illness. Psychiatr Serv. 2005; 56: 172-178.
- Orwin RG, Scott CK, Arieira C. Transitions through homelessness and factors that predict them: three-year treatment outcomes. J Subst Abuse Treat. 2005; 28: S23-39.
- Shinn M, Weitzman BC, Stojanovic D, Knickman JR, Jiménez L, Duchon L, et al. Predictors of homelessness among families in New York City: from shelter request to housing stability. Am J Public Health. 1998; 88: 1651-1657.