
Research Article
Austin J Psychiatry Behav Sci. 2016; 3(2): 1055.
Incidence of Hyperprolactinemia Induced by Atypical Antipsychotics
Amaladoss AS¹*, Balram C² and Wang A²
¹Department of Psychiatry, Fredericton Mental Health Centre, Canada
²Department of Health & Wellness, Fredericton Mental Health Centre, Canada
*Corresponding author: Amaladoss AS, Department of Psychiatry, Fredericton Mental Health Centre, Fredericton, New Brunswick, Canada
Received: June 29, 2016; Accepted: August 27, 2016; Published: September 07, 2016
Abstract
Background: Evidence support that Atypical Antipsychotics (AAPS) are effective in various psychiatric conditions, yet, evidence t1-t hyperprolactinemia induced atypical antipsychotics alters their benefit and risk ratio.
Objective: Prospective study was undertaken in a community setting, to determine the incidence of Hyperprolactinemia with atypical antipsychotics treatment.
Method: Patients were started on atypical antipsychotic for both schizophrenic and non-schizophrenic conditions. Serum Prolactin/monitored periodically from the baseline for one year duration. Total of 121 enrolled in the study, only 119 completed THE l year follow up. MALE 69 FEMALES 50; Olanzapine= 50; Risperidone= 59; Quetiapine= 8; Clozapine= 1. One patient on Olanzapine was detected with Pituitary Adenoma, hence omitted.
Data analysis: Descriptive and inferential analyses were done, except for clozapine, to ascertain the incidence of hyperprolactinemia and the relationship to age, gender and disease.
Results: % Hyperprolactinemia: Risperidone 69.49%>Olanzapine 32%> quetiapine12.5%
Male: Risperidone 64.86%>Olanzapine 23.33%>Quetiapine 0%
Female: Risperidone 77.27% >Olanzapine 45%> quetiapine 20% differences all statistically significant at 0.01 level. Schizophrenia 27.12%>Attention Deficit Disorder 20.34%>Bipolar Disorder18.64 Male 31.25%>Female 7.4% in attention deficit disorder Male 31.25%>Female 22% in Schizophrenia.
Mean prolactin: Male: Risperidone (21.33)>Olanzapine (14.81) Female: Risperidone (50.63)>Olanzapine (25.46) Male: Risperidone (22.31)> Olanzapine (15.47) in 3 months. Female: Risperidone (46.36)>Olanzapine (24.13) Highest LEVEL IN 41- 60 age with Risperidone = 52.03uG/I In 61+ AGE with Risperidone = 40.33uG/I
OR Olanzapine vs. Risperidone= 0.21 Male OR = 0.16 Female OR = 0.24.
Conclusion: Hyperprolactinemia may have significant HEALTH consequences both emotionally and physically and it is prudent to CHECK prolactin level periodically.
Keywords: Hyperprolactinemia; Antipsychotics; Incidence
Introduction
Hyperprolactinemia has been shown to have many physiological consequences some of them quite severe including sexual dysfunction osteoporosis breast cancer insulin resistance syndrome cardiovascular morbidity and severe emotional effects (hostility depression and anxiety) [1] (Figure 1).
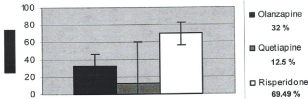
Figure 1: Percentage distribution of hyperprolactinemia by drugs for gender
Combined with 95% of confidence interval.
Hyperprolactinemia is a common side effect of conventional antipsychotics and is also associated with the use of atypical antipsychotics [2,3].
Conventional antipsychotics are associated with two to tenfold increases in prolactin level 4 and atypical antipsychotics produce lower increase than the conventional yet it occurs [2,6-8].
Objective
To determine the incidence of hyperprolactinemia induced by atypical antipsychotics and the relationship to age gender and disease which may enhance adequate follow up management of the patients who are treated with atypical antipsychotics.
Method
Patients were started on atypical antipsychotics for both schizophrenic and non-schizophrenic conditions Serum Prolactin has been monitored periodically from the baseline for one year duration total of 121 enrolled in the study but only 119 completed the one year follow-up There was about 69 males and 50 females the treatment breakdowns were as follows Olanzapine 50; Risperidone 59
Quetiapine 8 Clozapine 1 (Figure 2). One patient on Olanzapine was detected with Pituitary Adenoma in the follow-up hence he has been omitted from the study.
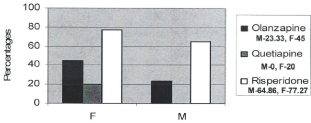
Figure 2: Percentage distribution of hyperprolactinemia by gender and drugs.
It should be noted that polypharmacy and dosage of the drugs have not been taken into consideration.
Data analysis
Descriptive and inferential analysis were done except for Clozapine to ascertain the incidence of hyperprolactinemia (Prolactin level>23ug/1) and the relationship to age gender and disease (Tables 1-4).
Number of Patients
F
M
Clozapine
1
0
Olanzapine
20
31
Quetiapine
5
3
Risperidone
22
37
Table 1: Frequency distribution of drug use by gender.
Number of Patients
Age Groups
Olanzapine
Quetiapine
Risperidone
0-19
3
2
20
20-40
18
1
14
41-60
17
5
16
61+
13
9
Total
51
8
59
Table 2: Frequency distribution of drug use by age groups – gender combined.
Count
Percent
Attention Deficit Disorder
17
14.29
Anxiety Disorder
4
3.36
Behavioural Disorder
2
1.68
Bipolar Disorder
21
17.65
Mood Disorder
23
19.33
Organic Brain Syndrome
9
7.56
PDD
1
0.84
Schizophrenia
41
34.45
Schizophrenia with diabetes
1
0.84
Total
119
100
Table 3: Frequency distribution of patients by diagnosis.
Clozapine
Olanzapine
Quetiapine
Risperidone
Total
Attention Deficit Disorder
17 (100%)
17 (100%)
Anxiety Disorder
1 (25%)
3 (75%)
4 (100%)
Behavioural Disorder
1 (50%)
1 (50%)
2
Bipolar Disorder
8 (38.1%)
4 (19.05%)
9 (42.86%)
21 (100%)
Mood Disorder
8 (34.78%)
2 (8.7%)
13 (56.52%)
23 (100%)
Organic Brain Syndrome
3 (33.33%)
1 (11.11%)
5 (55.56)
9 (100%)
PDD
1 (100%)
1 (100%)
Schizophrenia
1 (2.44%)
31 (75.61%)
9 (21.95)
41 (100%)
Schizophrenia with diabetes
1 (100%)
1 (100%)
Total
Table 4: Frequency (count and percentage) distribution of patients by diagnosis and drugs.
Results
Study findings reveal the percentage of hyperprolactinemia has been seen with Risperidone 69.49% Olanzapine 32% and with Quetiapine 12.5% in gender combined. In male the percentage of hyperprolactinemia has been seen with Risperidone 64.86% Olanzapine 23.33% Quetiapine 0%. In female the percentage of hyperprolactinemia has been seen with Risperidone 77.27% Olanzapine 45% and Quetiapine 20%. Significant testing of the differences in all three is statistically significant at 0.01 levels (Figure 3). The mean prolactin in male with Risperidone is 21.33 ug/I compared with Olanzapine 14.8lug/1 and in female with Risperidone is 50.63ug/lcompared with Olanzapine 25.46ug/I. In three months period mean prolactin has been seen in males with Risperidone 22.3lug/1 compared to Olanzapine 15.47ug/I whereas in female with Risperidone 46.36ug/I compared to Olanazapine 24.13ug/I. The percentage of hyperprolactinemia in schizophrenia group is 27.12% and with attention deficit disorder 20.34% and with bipolar disorder 18.64%. It is interesting to note that in males who suffer from attention deficit disorder the percentage of hyperprolactinemia has been seen 31.25% compared to females 7.4% and in schizophrenia in male the percentage of hyperprolactinemia is 31.25% compared to female 22%. The highest level of mean prolactin in the age group between 41 to 60 with Risperidone 52.03ug/I and in 61+ age group the mean prolactin has been seen with Risperidone is 40.33ug/I. For gender combined Odd ratio Olanzapine vs. Risperidone is 0.21, 95%. CI (-24.73,1.51) For male odd ratio is 0.16, 95% CI (- 9.18,3.51) and for female odd ratio is 0.24, 95% CI (-24.73,1.51) (Figure 4).
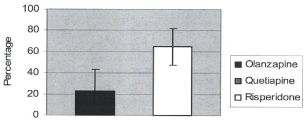
Figure 3: Percentage distribution of hyperprolactinemia by drugs for males
with 95% confidence interval.
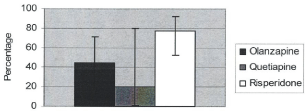
Figure 4: Percentage distribution of hyperprolactinemia by drugs for females
with 95% confidence interval.
Discussion
The findings in this study reveal that all three antipsychotics do affect prolactin level at varying degree and Resperidone seems to have higher propensity to induce hyperprolactinemia compared to Olanzapine and Quetiapine.
Female seems to be more affected than male and the elevation is observed in 3 months itself.
Higher percentage of hyperprolactinemia has been seen in Schizophrenia and Attention Deficit Disorder compared to other conditions.
In both conditions, hyperprolactinemia has been seen more in male than female and this evidence hitherto has not been reported in the literature. This may be taken into consideration in clinical evaluation in follow up assessment of patients who may present with mood and behavioural disturbances.
Further, the findings of highest level of mean prolactin seen with resperidone in 41-60 years as well in 61+ years age group, warrant close monitoring in view of physiological consequences, some of them are quite severe like osteoporosis, breast cancer, insulin resitance, cardiovascular morbidity and mood disturbances.
Conclusion
This study reveals varying incidence of hyperprolactimeia in relation to age, gender and disease apart from the drugs and has significant clinical implications. It is crucial to bear in mind that hyperprolactinemia may occur in patients who are treated with atypical antipsychotics which may have consequences in both emotional and physical condition of the patients. Hence it is advisable to check prolactin level in the follow up management.
References
- Halbreich U, Kinon BJ, Gilmore JA, Kahn LS. Elevated Prolactin levels in patients Schizophrenia: mechanisms and related adverse effects. Psychoneuroendocrinology. 2003; 28: 53-67.
- Goodnick PJ, Rodriguez L, Santana O. Antipsychotics: impact on prolactin levels. Expert Opin Pharmacother. 2002; 3: 1381-1391.
- Hamner M. The effects of atypical antipsychotics on prolactin levels. Ann Clin Psychiatry. 2002; 14: 163-173.
- Meltzer HY, Fang VS. The effect of neuroleptics on serum prolactin in schizophrenic patients. Arch Gen Psychiatry. 1976; 33: 279-286.
- Gruen PH, Sachar EJ, Langer G, Altman N, Leifer M, Franz A, et al. Prolactin responses to neuroleptics in normal and schizophrenic subjects. Arch Gen Psychiatry. 1978; 35: 108-116.
- Wudarsky M, Nicolson R, Hamburger SD, Spechler L, Gochman P, Bedwell J, et al. Elevated prolactin in pediatric patients on typical and atypical antipsychotics. J child Adolesc Psychopharmacol. 1999; 9: 239-245.
- Kleinberg DL, Davis JM, De Coster R, Van Baelen B, Brecher M. Prolactin levels and adverse events in patients treated with risperidone. J Clin Psychopharmacol. 1999; 19: 57-61.
- Schultz E, Fleischhaker C, Remschmidt HE. Correlated changes in symptoms and neurotransmitter indices during maintenance treatment with Clozapine or conventional neuroleptics in adolescents and young adults with schizophrenia. J Child Adolesc Psychopharmacol. 1996; 6: 119-131.