
Research Article
Austin J Radiol. 2015;2(5): 1030.
Urinalysis in Pyonephrosis: Does a Normal Result Rule Out Pyonephrosis?
Mougnyan Cox¹*, Ifechi Momah², Huan Dong¹ and Santosh Selvarajan¹
¹Radiology Resident, Thomas Jefferson University, USA
²Radiology Resident, Georgetown University, USA
*Corresponding author: Mougnyan Cox, Radiology Resident, Thomas Jefferson University, 132 South 10th Street, Philadelphia, PA 19107, USA
Received: July 20, 2015; Accepted: August 14, 2015; Published: August 18, 2015
Abstract
Purpose: To determine if a normal preprocedural urinalysis rules out Pyonephrosis.
Methods: Urinalysis results, white cell count, and bandemia obtained within 24 hours of subsequent percutaneous nephrostomy were reviewed in patients with documented Pyonephrosis.
Results: 26 out of 27 patients with Pyonephrosis had an abnormal urinalysis. One patient with Pyonephrosis had a negative urinalysis and subsequently grew Candida albicaans on urine cultures.
Conclusion: A normal preprocedural urinalysis does not rule out Pyonephrosis.
Keywords: Nephrostomy; Percutaneous; Pyonephrosis; Urinalysis
Introduction
Pyonephrosis is a medical emergency, and is defined as the presence of pus in an obstructed renal collecting system [1]. Patients usually present with fever, flank pain, leukocytosis, and an abnormal urinalysis [2]. Patients with proven Pyonephrosis may be a febrile [2], and ultrasound was only 62% sensitive for detecting Pyonephrosis in one study with some patients have frank pus on urine aspiration despite an anechoic renal collecting system [3]. Due to the high morbidity and mortality associated with Pyonephrosis, intravenous administration of broad-spectrum antibiotics and prompt urinary drainage is indicated whenever the diagnosis is suspected [2,4]. While it is known that patients with Pyonephrosis may not always present with fever or an elevated white count, it is less clear whether a normal Urinalysis (UA) in a patient with a dilated renal collecting system rules out the presence of Pyonephrosis. The purpose of our study was to determine the sensitivity of a preprocedural urinalysis for aspiration-proved Pyonephrosis.
Methods
After Institutional Review Board approval was obtained, a retrospective review of an imaging database and clinical charts from 2006-2014 was performed. Patients were selected on the basis of percutaneous aspiration procedure results specifying the presence of pus at the time of aspiration. The clinical charts of these patients were also reviewed for relevant clinical history as well as inflammatory markers (leukocytosis, bandemia) and results of preprocedural urinalysis performed up to 24 hours prior to aspiration.
All Percutaneous urinary interventions were performed by 5 fellowship-trained interventional radiologists with 60 years of cumulative experience. The results of urine cultures from samples obtained at the time of aspiration were recorded when available.
Results
Thirty patients were found to have Pyonephrosis, confirmed by aspiration of grossly purulent urine at the time of Percutaneous Nephrostomy (PCN). There were 23 female and 7 male patients. The average age of the patients was 58, with a range of 23 to 96 years. Renal stones were implicated as the cause of Pyonephrosis in 16 out of 30 patients (53%). An additional 10 patients had Pyonephrosis in the setting of a pelvic malignancy (33%), most commonly cervical cancer, present in four patients. There was a notably high rate of paraplegia/tetraplegia (5 out of 30 cases or 17%) in our patients with Pyonephrosis. This may be Multifactorial, with bladder dysfunction and frequent access of the urinary collecting system contributing to various degrees. Two patients had a pregnancy complicated by Pyonephrosis, and were in their second trimester at the time of intervention (Figure 1&2).
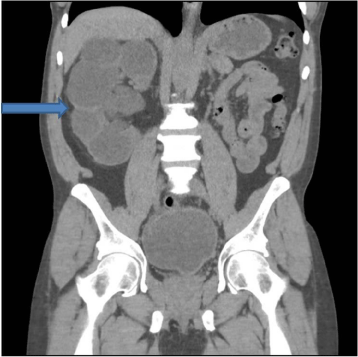
Figure 1: Figure 1 is a coronal CT scan of the abdomen and pelvis showing
severe hydronephrosis with renal cortical thinning in a patient with right flank
pain and fever.
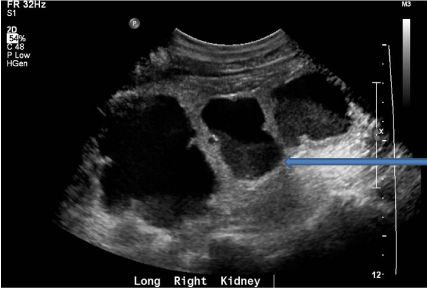
Figure 2: Ultrasound of the paient in Figure 1 shows dilated renal calyces
with layering debris. Percutenous aspiration revealed frank pus.
A preprocedural urinalysis was obtained in 27 out of 30 patients. The urinalysis was positive in 26 out of 27 cases (96%). Only one patient with Pyonephrosis had a negative urinalysis, and the culture obtained from urinary aspiration was positive for Candida. The white blood cell count was abnormally elevated in 18 out of 29 cases (62%), and bandemia was present in 13 out of 28 patients (46%). Neutropenia was present in one patient. Of note, no patient with Pyonephrosis had a triple-negative clinical finding (normal white cell count, normal urinalysis and no bandemia). Both bandemia and leukocytosis were present in the patient with Pyonephrosis and a normal urinalysis.
Overall, urine aspirate cultures were positive in 24 out of 27 cases in which they were obtained (89%). The most common organism in our patient population was Escherichia coli, present in 8 out of 27 cases (30%). Four patients had Pseudomonas (15%), and another 4 had Proteus.
Discussion
Fever, flank pain, leukocytosis, and a dilated renal collecting system are the typical findings in a patient with Pyonephrosis. However some patients may not present with an elevated white count or a fever, particularly in the very old or young, or in the setting of immunocompromised. Our findings suggest that while the urinalysis is usually positive in patients with Pyonephrosis, a normal UA does not completely rule out Pyonephrosis. A normal urinalysis in the setting of Pyonephrosis could potentially be caused by complete obstruction of the infected portion of the collecting system. It is also notable that the only patient with Pyonephrosis and a normal urinalysis was the patient with a fungal infection (Candida). It may be that the immune response to bacterial infections is more robust with greater inflammatory debris in the collect in system. The turbidity and cloudiness seen during aspiration of Candida infected dilated collecting system may in part be due to the presence of fungal hyphae. Candida is a known cause of fungus ball in the renal collecting system [5,6], with brownish debris on pyelotomy correlating with fungal hyphae on microbiologic analysis of the urine aspirate. In 2002, Kale et al also reported a case of renal candidiasis in a boy with fever, flank pain, chills and hydronephrosis on renal ultrasound. The treatment was similar to a patient with Pyonephrosis, with prompt drainage and decompression of the collecting system; the main difference was that, antifungal therapy substituted for antibacterial agents (Figure 3).
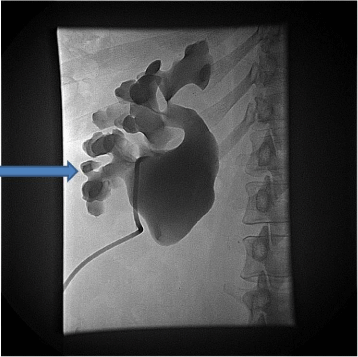
Figure 3: Injection of contrast into the collecting system via a nephrostomy
tube in a patient with flank pain and fever shows a dilated renal collecting
system due to congenital ureteropelvic junction obstruction.
Since Pyonephrosis is a medical emergency, all patients with a dilated renal collecting system and clinical suspicion for infection should undergo further evaluation with urinary aspiration for decompression of the collecting system and microbiologic analysis (Figure 4).
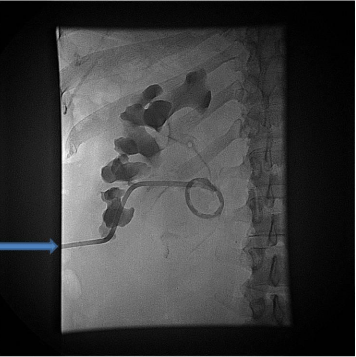
Figure 4: Follow-up contrast injection several days later following tube
exchange shows interval decompression of the collecting system with a
decrease in the size of renal calyces and pelvis.
Conclusion
A negative preprocedural urinalysis does not definitively rule out Pyonephrosis. Prompt decompression of the renal collecting system is indicated if the index of clinical suspicion remains high.
References
- Li A, Regalado S. Emergent percutaneous nephrostomy for diagnosis and management of pyonephrosis. Seminars in Interventional Radiology. 2012; 29: 218-225.
- Yoder I, Pfister R, Lindofors K, Newhouse J. Pyonephrosis: imaging and intervention. American Journal of Roentgenology. 1983; 141: 735-740.
- Jeffrey R, Laing F, Wing V, Hoddick W. Sensitivity of sonography in Pyonephrosis: a re-evaluation. American Journal of Roentgenology. 1985; 144: 71-73.
- Lowe LH, Zagoria RJ, Baumgartner BR, Dyer RB. Role of imaging and intervention in complex infections of the urinary tract. American Journal of Roentgenology. 1994; 163: 363–367.
- Stuck K, Silver T, Jaffe M, Bowerman R. Sonographic demonstration of renal fungus balls. Radiology 1982; 142: 473-474.
- Kale H, Narlawar R, Rathod K. Renal fungus ball: an unusual sonographic finding. Journal of Clinical Ultrasound. 2002; 30: 178-180.